Eyelid Layers - Skin Deep Beauty
 Anterior to posterior:
Anterior to posterior:
- Skin: Thinnest in body.
- Subcutaneous tissue: Loose, avascular.
- Orbicularis Oculi: Closes lid (palpebral, orbital). Muscle of Riolan at margin.
- Submuscular areolar tissue: Loose connective; neurovascular plane.
- Orbital Septum & Preaponeurotic Fat: Septum (barrier), fat (cushion).
- Levator Aponeurosis & Müller’s muscle: Elevate upper lid (LPS main, Müller's accessory).
- Tarsal Plate: Dense connective tissue; structure, Meibomian glands. Height: Sup. ~10mm, Inf. ~4mm.
- Palpebral Conjunctiva: Inner mucous membrane.
📌 Mnemonic: SC O SMOrc TCo (Skin, SubCut, Orbicularis, SubMusc, Orbital Septum, (Fat), Tarsus, Conjunctiva)
⭐ The grey line, an important surgical landmark, is the mucocutaneous junction and represents the anterior-most extent of the muscle of Riolan (part of orbicularis oculi).
Eyelid Muscles & Movements - Muscle Power
- Protraction (Eyelid Closure):
- Orbicularis Oculi (Innervation: CN VII)
- Palpebral part: Gentle closure, blinking.
- Orbital part: Forced closure (e.g., against light, threat).
- Lacrimal part (Horner's muscle): Compresses lacrimal sac, aids tear drainage.
- Orbicularis Oculi (Innervation: CN VII)
- Retraction (Eyelid Opening):
- Levator Palpebrae Superioris (LPS) (Innervation: CN III, superior division): Main elevator of upper lid.
- Müller's muscle (Sympathetic fibers): Contributes approx. 2mm to upper lid elevation.
- Inferior Rectus muscle connections & Inferior Tarsal muscle (sympathetic): Lower lid retraction.
- 📌 Mnemonic: LOC (LPS Opens, Orbicularis Closes).
- Blinking: Spontaneous, reflex (e.g., corneal, dazzle, menace), voluntary.
- Bell's Phenomenon: Eyeball rolls up & out on attempted forced closure (protective).
- Key Measurements:
- Palpebral Fissure Height (PFH): 8-12mm.
- Margin Reflex Distance 1 (MRD1): 4-4.5mm.
- Margin Reflex Distance 2 (MRD2): 5-5.5mm.
- Levator Function (LF): >12mm (Good).
⭐ Müller's muscle, innervated by sympathetic fibers, contributes approximately 2mm to upper eyelid elevation and is responsible for lid lag in thyroid eye disease.

Eyelid Glands - Secretion Station

- Eyelids house several glands crucial for tear film stability and ocular surface health.
| Gland | Location | Type | Secretion | Function | Clinical Relevance |
|---|---|---|---|---|---|
| Meibomian | Tarsal plates | Sebaceous | Lipid (sebum) | Prevents tear evaporation; tear film stability | Chalazion (chronic inflammation), Hordeolum internum (acute infection) |
| Zeis | Associated with eyelash follicles | Sebaceous | Sebum | Lubricates eyelashes | Hordeolum externum (stye) |
| Moll | Empties into lash follicle or Zeis gland duct | Apocrine sweat | Sweat | Unknown; ?antimicrobial | Hordeolum externum (stye), Cyst of Moll |
| Krause & Wolfring | Conjunctival fornices & tarsal border | Accessory Lacrimal (Serous) | Aqueous | Contribute to aqueous layer of tear film | Dry eye syndrome |
📌 Meibomian = Main oil; Zeis = Zits on lashes; Moll = Moisture (sweat).
Neurovascular Supply - Vital Lines
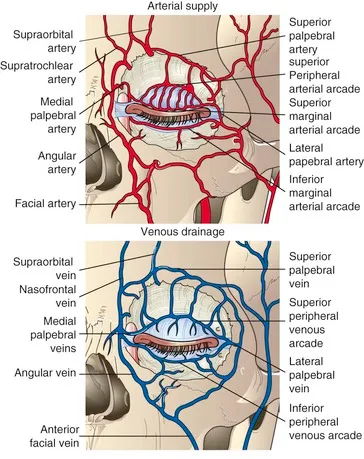
- Arterial Supply:
- Branches: Lateral palpebral a. (from lacrimal a.), Medial palpebral a. (from ophthalmic a.).
- Form marginal & peripheral arterial arcades.
- Venous Drainage:
- Pretarsal (anterior to tarsus): Anterior facial vein.
- Posttarsal (posterior to tarsus): Ophthalmic veins, pterygoid plexus.
- Lymphatic Drainage:
- Medial structures: Submandibular lymph nodes.
- Lateral structures: Preauricular (superficial parotid) lymph nodes.
- Sensory Innervation:
- Upper Lid (V1 - Ophthalmic division): Lacrimal, Supraorbital, Supratrochlear, Infratrochlear nerves.
- Lower Lid (V2 - Maxillary division): Infraorbital, Infratrochlear nerves.
- Motor Innervation:
- Levator Palpebrae Superioris (LPS): CN III (Oculomotor N.).
- Orbicularis Oculi: CN VII (Facial N.).
- Müller's Muscle: Sympathetic fibers.
⭐ The sensory innervation of the upper eyelid is primarily from the ophthalmic division (V1) of the trigeminal nerve, while the lower eyelid is supplied by the maxillary division (V2).
High‑Yield Points - ⚡ Biggest Takeaways
- Eyelid layers: Skin, Subcutaneous, Orbicularis oculi (CN VII), Submuscular areolar, Tarsal plate (Meibomian glands), Conjunctiva.
- Lid elevation: Levator Palpebrae Superioris (LPS) (CN III) and Muller’s muscle (sympathetic).
- Lid closure: Orbicularis oculi (CN VII).
- Key glands: Meibomian (tarsus, sebaceous), Zeis (lashes, sebaceous), Moll (lashes, apocrine).
- Sensory nerves: Upper lid by V1 (Ophthalmic); Lower lid by V2 (Maxillary).
- Grey line: Surgical landmark; divides anterior & posterior lamellae.
- Blinking reflex: Afferent CN V, Efferent CN VII.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

