Overview & Definitions - Twitchy Twins Intro
- Blepharospasm (Benign Essential Blepharospasm - BEB): Involuntary, bilateral, repetitive, forceful eyelid closure. A focal dystonia affecting orbicularis oculi.
- Hemifacial Spasm (HFS): Unilateral, intermittent, involuntary contractions of muscles innervated by CN VII (facial nerve), typically starting around the eye.
- Primary Cause Distinction:
- BEB: Mostly idiopathic; rarely secondary to drugs (e.g., neuroleptics) or basal ganglia lesions.
- HFS: Often vascular compression of facial nerve root exit zone; less commonly tumors or post-Bell's palsy.

⭐ Blepharospasm typically bilateral, HFS unilateral.
Essential Blepharospasm (BEB) - Squeezy Eye Saga
- Bilateral, involuntary, progressive, spasmodic eyelid closure; idiopathic focal dystonia.
- Onset: Typically 50-70 years, F > M.
- Symptoms: ↑ blinking → forceful spasms, photophobia, difficulty keeping eyes open; can lead to functional blindness.
- Aggravated by: Bright light, stress, fatigue.
- Relieved by: Sleep, relaxation, sensory tricks (geste antagoniste).
- 📌 BEB: Bilateral Eyelid spasms, Botox is best.
⭐ Associated with Meige syndrome (oromandibular dystonia + blepharospasm).
- Treatment:
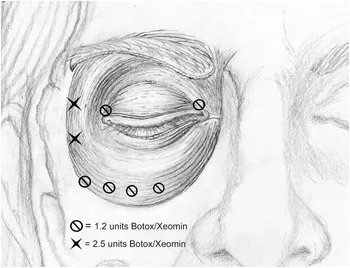
- 1st line: Botulinum toxin A injections (orbicularis oculi, procerus, corrugator) q 3-4 months.
- 2nd line: Surgical (limited myectomy) if botox fails.
Hemifacial Spasm (HFS) - One-Sided Winks
- Unilateral, involuntary, intermittent contractions (clonic/tonic) of facial nerve (CN VII) muscles.
- Etiology:
- Primary (Idiopathic): Most common.
⭐ Most common cause: vascular compression of CN VII root exit zone (REZ) by aberrant vessel (AICA, PICA).
- Secondary: Post-facial palsy, CPA tumors, MS, trauma.
- Primary (Idiopathic): Most common.
- Clinical Features:
- Starts orbicularis oculi, spreads ipsilaterally.
- "Other Babinski sign": Eyebrow lift with forced eye closure.
- Persists during sleep.

- Investigations:
- MRI Brain/Brainstem: Rule out secondary causes.
- Treatment:
- Botulinum toxin A injections (first-line).
- Medical: Carbamazepine, gabapentin (less effective).
- Surgical: Microvascular Decompression (MVD) if refractory_cases_with_identified_vascular_loop_
Differentiating Spasms - Twitch Tell-Tale
| Feature | Essential Blepharospasm (BEB) | Hemifacial Spasm (HFS) |
|---|---|---|
| Laterality | Typically bilateral, symmetric onset | Strictly unilateral |
| Muscles Involved | Orbicularis oculi; may spread (Meige's) | Muscles innervated by CN VII (one side) |
| During Sleep | Spasms usually cease | Spasms often persist |
| Common Etiology | Often idiopathic; drug-induced; dystonia | Vascular compression (CN VII root); post-Bell's |
| Other Facial Areas | May involve lower face/neck (Meige's) | Progresses: eye → cheek → mouth → neck |
Treatment Toolkit - Taming The Twitches
⭐ Botulinum toxin A is the first-line treatment for both BEB and symptomatic HFS.
- Botulinum Toxin A (BoNT-A):
- Gold standard; inhibits acetylcholine release.
- Repeated injections every 3-4 months.
- Target muscles: Orbicularis oculi, procerus, corrugator.
- Supportive Measures: Dark glasses, FL-41 tinted lenses, stress reduction.
- Surgical Options (for refractory cases):
- BEB: Limited myectomy or frontalis suspension.
- HFS: Microvascular Decompression (MVD) of facial nerve.
High‑Yield Points - ⚡ Biggest Takeaways
- Blepharospasm: Bilateral, involuntary orbicularis oculi spasms; can cause functional blindness. Botulinum toxin (BoNT-A) is first-line.
- Hemifacial Spasm: Unilateral facial muscle (CN VII) twitching; often from vascular compression of the facial nerve.
- Key differentiator: Hemifacial Spasm persists during sleep.
- BoNT-A is the primary treatment for both; Microvascular Decompression (MVD) is curative for Hemifacial Spasm.
- Meige Syndrome: Blepharospasm combined with oromandibular dystonia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

