TON: Definition & Types - Nerve Under Siege
- Traumatic Optic Neuropathy (TON): Acute optic nerve dysfunction and vision loss following ocular or craniofacial trauma.
- Classification:
- Direct TON:
- Mechanism: Direct penetration or impingement by foreign body, bony fragment.
- Causes: Orbital fractures, penetrating injuries (e.g., pellets).
- Indirect TON (iTON):
- Mechanism: Shearing forces, contusion, edema, or vascular compromise transmitted from a remote impact site.
- Causes: Blunt head trauma (frontal, periorbital blows).
- Anatomical Location:
- Anterior TON: Involves optic nerve head.
- Posterior TON: Injury behind globe (orbital, canalicular, intracranial).
- Direct TON:
⭐ Indirect TON is more common than direct TON and can occur with closed head injury without direct orbital trauma.
TON: Pathophysiology - Damage Unveiled
- Primary Injury (Immediate Impact):
- Direct: Optic nerve laceration, contusion, avulsion from penetrating trauma/orbital fractures.
- Indirect: Shearing forces (acceleration-deceleration) transmitted to optic nerve. Intracanalicular segment, fixed in bony optic canal, is most vulnerable.
- Secondary Injury (Delayed, Progressive Damage):
- Edema & swelling → ↑ intra-canalicular pressure, causing compartment syndrome.
- Ischemia: From vasospasm, direct vascular compression, or thrombosis.
- Inflammation: Release of inflammatory mediators (cytokines).
- Excitotoxicity (e.g., glutamate) & Apoptosis (programmed cell death of RGCs).
⭐ Indirect TON is more common than direct TON, potentially occurring without direct globe injury or orbital fractures.
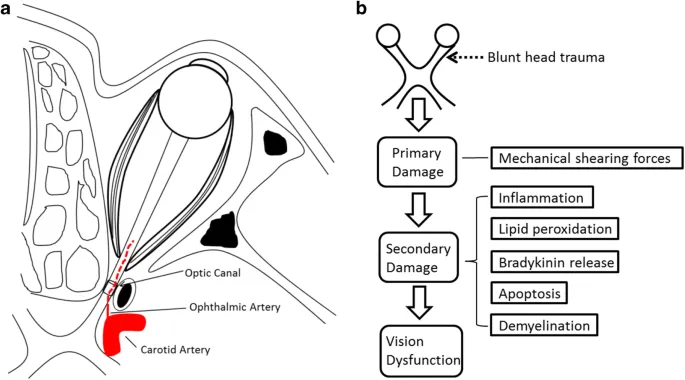
TON: Clinical Picture - Vision Vanishing
-
Symptoms:
- Sudden, often severe, vision loss (key feature).
- Blurred vision.
- Dyschromatopsia (impaired color vision).
-
Key Signs:
- Relative Afferent Pupillary Defect (RAPD) / Marcus Gunn Pupil.
- ↓ Visual Acuity (VA).
- Visual field defects: central, paracentral, altitudinal.
- Optic disc: Initially normal; pallor/atrophy develops later (weeks).
-
Associated Findings:
- Proptosis.
- Ophthalmoplegia.
- Periorbital hematoma/ecchymosis.
⭐ RAPD is often the earliest and most reliable sign of TON, even with minimal VA loss.
TON: Diagnostic Clues - Finding the Fault
- History: Nature of trauma (direct/indirect impact, e.g., blow to brow).
- Ophthalmic Exam:
- ↓Visual Acuity (VA) significantly.
- Relative Afferent Pupillary Defect (RAPD) (+) is a hallmark.
- ↓Color vision (dyschromatopsia).
- Visual Field (VF) defects (e.g., altitudinal, central scotoma).
- Fundoscopy: Optic disc may be normal initially; edema or pallor develops later (pallor after 3-6 weeks).
- Imaging:
- CT Scan (orbital/cranial, thin cuts through optic canal): Essential for bony injury (optic canal fracture), foreign bodies.
- MRI: Superior for direct optic nerve visualization (edema, hemorrhage, contusion, transection).
- VEP (Visual Evoked Potential): ↓Amplitude, ↑latency. Objective assessment of optic nerve conduction; prognostic utility, but limited in acute settings or uncooperative patients.
⭐ RAPD is often the most reliable objective sign in TON, especially if the patient is uncooperative or fundus is initially normal.
TON: Management & Fate - Rescue & Reality
- Management (Controversial):
- Observation: Mild, non-progressive cases.
- Medical: High-dose corticosteroids (e.g., NASCIS II/III protocols, Methylprednisolone 30 mg/kg IV bolus); evidence debated (CRASH trial).
- Surgical: Optic Nerve Decompression (OND) for bony impingement or failed medical Rx; efficacy debated.
- Supportive care.
- Prognostic Factors: Initial VA (most critical), RAPD presence, direct vs. indirect injury, intervention timing, CT (canal fracture). ⭐> Initial Visual Acuity is the single most important prognostic factor in Traumatic Optic Neuropathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Indirect TON is more common, often from blunt head trauma.
- Key signs: ↓VA, RAPD, dyschromatopsia, visual field defects.
- CT orbit/brain essential to exclude bony compression or hematoma.
- High-dose IV corticosteroids (e.g., methylprednisolone) are often first-line, though evidence is debated.
- Optic canal decompression surgery considered for bony impingement or steroid failure.
- Prognosis is variable; initial VA is a strong predictor of outcome.
- Always rule out globe rupture or orbital compartment syndrome concurrently.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

