Ocular Trauma

On this page
👁️ The Trauma Spectrum: Ocular Injury Mastery
The eye's exquisite anatomy makes it remarkably vulnerable-blunt force, penetrating objects, chemical burns, and blast injuries can devastate vision in seconds. You'll master the complete spectrum of ocular trauma, from rapid triage that distinguishes sight-threatening emergencies to pattern recognition that reveals hidden globe ruptures, then build surgical decision-making skills that determine when to intervene versus observe. By integrating assessment techniques, damage grading systems, evidence-based treatments, and rehabilitation strategies, you'll develop the clinical architecture needed to preserve vision when every minute counts.
Ocular trauma represents one of the leading causes of monocular blindness worldwide, affecting approximately 2.4 million people annually in the United States alone. The complexity of eye injuries spans from simple corneal abrasions to devastating globe ruptures, each requiring specific diagnostic approaches and treatment protocols. Master the trauma classification systems, and you unlock the ability to predict outcomes, guide treatment decisions, and communicate effectively with subspecialists.
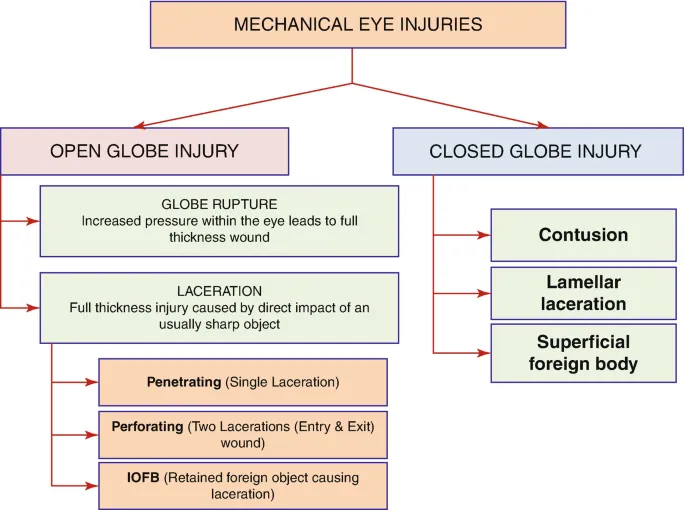
The eye's unique anatomy creates vulnerability patterns that follow predictable injury mechanisms. Understanding these relationships transforms chaotic emergency presentations into systematic diagnostic challenges with clear management pathways.
📌 Remember: SIGHT for major trauma categories - Surface injuries, Intraocular foreign bodies, Globe rupture, Hyphema, Thermal burns. Each category has specific visual acuity thresholds and time-sensitive interventions that determine final outcomes.
| Trauma Type | Incidence Rate | Vision Threat Level | Emergency Timeline | Key Diagnostic Sign | Treatment Priority |
|---|---|---|---|---|---|
| Corneal Abrasion | 45% of all trauma | Low | 24-48 hours | Fluorescein uptake | Pain control + healing |
| Hyphema | 12% of blunt trauma | Moderate-High | 6-8 hours | Blood in anterior chamber | IOP monitoring |
| Globe Rupture | 3% of all trauma | Severe | <2 hours | Seidel sign positive | Immediate surgery |
| IOFB | 8% of penetrating | High | 4-6 hours | CT metallic density | Surgical removal |
| Chemical Burns | 7% of all trauma | Variable | Minutes | pH <7 or >11.5 | Immediate irrigation |
⭐ Clinical Pearl: Globe rupture occurs in 15-20% of severe blunt trauma cases when impact force exceeds 3,000 pounds per square inch. The "rule of 5s" applies: 5mm pupil irregularity, 5+ IOP difference between eyes, and visual acuity worse than 5/200 suggest rupture until proven otherwise.
- Mechanism-Based Injury Patterns
- High-velocity projectiles: >100 mph create penetrating injuries with posterior segment involvement in 65% of cases
- Blunt force trauma: >50 pounds force causes contusion injuries with angle recession in 40% of cases
- Sports-related: Basketball 35%, baseball 25%, tennis 15% of recreational injuries
- Motor vehicle accidents: Airbag deployment reduces injury by 85% but creates specific burn patterns
- Chemical exposure: Alkali burns penetrate deeper than acids, with pH >11.5 causing full-thickness damage within 15 seconds
💡 Master This: The "20-20-20 rule" for trauma assessment - 20 seconds for primary survey, 20 minutes for detailed examination, 20% vision loss threshold for subspecialty consultation. Every trauma patient requires bilateral examination since 12% have fellow eye involvement.
Understanding trauma epidemiology reveals that males aged 20-30 account for 60% of severe injuries, with workplace accidents representing 40% of penetrating trauma. Alcohol involvement occurs in 35% of cases and correlates with delayed presentation and worse outcomes.
Connect these foundational trauma patterns through systematic assessment protocols to understand how rapid triage decisions determine visual outcomes.
👁️ The Trauma Spectrum: Ocular Injury Mastery
🎯 Rapid Assessment Arsenal: Emergency Triage Mastery
📌 Remember: PERRL-A assessment - Pupils, Extraocular movements, Red reflex, Retinal examination, Lids/lashes, Anterior chamber. Each component has specific abnormality thresholds that trigger immediate subspecialty consultation.
| Assessment Component | Normal Finding | Abnormal Threshold | Clinical Significance | Action Required | Time Sensitivity |
|---|---|---|---|---|---|
| Visual Acuity | 20/20 to 20/40 | >2 line decrease | Significant injury | Detailed exam | <30 minutes |
| Pupil Response | 2-4mm, reactive | >1mm difference | Neurologic/structural | Imaging + consult | <15 minutes |
| Intraocular Pressure | 10-21 mmHg | <5 or >30 mmHg | Globe integrity | Immediate action | <10 minutes |
| Anterior Chamber | Clear, formed | Blood, shallow, flat | Penetrating injury | Surgical consult | <5 minutes |
| Red Reflex | Bright, symmetric | Absent or asymmetric | Media opacity | Urgent evaluation | <20 minutes |
⭐ Clinical Pearl: The "Seidel test" using 2% fluorescein reveals aqueous humor leakage in 95% of full-thickness corneal lacerations. Positive streaming under cobalt blue light indicates immediate surgical repair within 6-8 hours for optimal outcomes.
- Priority-Based Examination Sequence
- Primary Survey (<2 minutes)
- Globe integrity assessment using indirect visualization
- Lid retraction without pressure to assess anterior chamber depth
- Pupil reactivity testing with penlight examination
- Secondary Survey (5-10 minutes)
- Visual acuity measurement using Snellen chart or finger counting
- Visual field confrontation testing for gross defects
- Extraocular movement assessment for diplopia or restriction
- Intraocular pressure measurement only if globe integrity confirmed
- Primary Survey (<2 minutes)
💡 Master This: The "Rule of 4s" for trauma severity - 4mm pupil asymmetry, 4+ quadrants of subconjunctival hemorrhage, 4 lines of visual acuity loss, and 4 hours since injury all correlate with increased surgical intervention requirements and worse visual prognosis.
Chemical injury protocols require immediate irrigation with normal saline or lactated Ringer's solution for minimum 30 minutes, targeting pH normalization between 7.0-7.4. Alkali burns require longer irrigation due to deeper penetration and continued tissue damage for hours after exposure.
Documentation standards require bilateral examination findings, mechanism of injury details, time of injury, first aid measures, and tetanus immunization status. Photography when possible provides medicolegal documentation and subspecialist communication tools.
Connect these rapid assessment techniques through systematic injury classification to understand how specific trauma patterns guide treatment decisions.
🎯 Rapid Assessment Arsenal: Emergency Triage Mastery
🔍 Injury Pattern Recognition: The Trauma Detective's Guide
Mechanism-specific injury patterns follow predictable anatomical distributions based on force vectors, impact velocity, and object characteristics. Understanding these relationships enables reverse engineering of trauma scenarios and anticipation of associated injuries that may not be immediately apparent.
📌 Remember: IMPACT for blunt trauma sequelae - Iris tears, Macular holes, Pupil abnormalities, Angle recession, Cyclodialysis, Trabecular meshwork damage. Each occurs at specific force thresholds and correlates with long-term glaucoma risk of 10-20%.
| Injury Mechanism | Primary Damage | Secondary Effects | Delayed Complications | Recognition Signs | Risk Stratification |
|---|---|---|---|---|---|
| High-velocity projectile | Corneal/scleral perforation | Vitreous hemorrhage | Endophthalmitis 5-15% | Entry wound + IOFB | High risk |
| Blunt force >50 lbs | Angle recession | IOP elevation | Glaucoma 10-20% | Hyphema + mydriasis | Moderate risk |
| Sharp object penetration | Lens capsule rupture | Traumatic cataract | Phacogenic uveitis | Cortical material leak | High risk |
| Chemical splash | Corneal epithelial loss | Limbal ischemia | Corneal perforation | pH <7 or >11.5 | Variable risk |
| Thermal exposure | Lid/conjunctival burns | Symblepharon formation | Dry eye syndrome | Tissue blanching | Low-moderate risk |
⭐ Clinical Pearl: "Sympathetic ophthalmia" occurs in 0.2-0.5% of penetrating injuries involving uveal tissue exposure. Risk factors include delayed repair >24 hours, retained foreign material, and extensive uveal prolapse. Prophylactic enucleation consideration applies when no light perception and extensive damage present.
- Blunt Trauma Injury Cascade
- Primary Impact Effects (immediate)
- Corneal abrasions in 85% of cases with epithelial disruption
- Subconjunctival hemorrhage masking underlying scleral rupture in 5%
- Anterior chamber reaction with cell and flare within 2-4 hours
- Secondary Pressure Effects (minutes to hours)
- Hyphema formation from iris vessel rupture in 20-30% of severe cases
- Lens subluxation with zonular fiber disruption requiring >1000 lbs force
- Vitreous hemorrhage from retinal vessel avulsion in 15% of posterior injuries
- Tertiary Inflammatory Response (days to weeks)
- Traumatic uveitis with IOP fluctuations and synechiae formation
- Proliferative vitreoretinopathy in 10-15% of severe posterior segment injuries
- Primary Impact Effects (immediate)
💡 Master This: The "Berlin Edema" pattern indicates commotio retinae from blunt trauma, appearing as grayish-white retinal opacity that resolves spontaneously in 80% of cases within 2-4 weeks. Persistent changes suggest permanent photoreceptor damage with visual field defects.
Chemical injury severity correlates with pH extremes, contact duration, and penetration depth. Alkali burns (pH >11.5) cause liquefactive necrosis with continued tissue destruction, while acid burns (pH <2.5) create coagulative necrosis with self-limiting damage.
Sports-related injury patterns vary by activity: Basketball causes blunt trauma with orbital fractures in 25%, Baseball creates high-velocity impact with globe rupture risk, and Racquet sports produce penetrating injuries from string/frame contact.
Connect these injury recognition patterns through systematic damage assessment to understand how anatomical disruption guides surgical intervention decisions.
🔍 Injury Pattern Recognition: The Trauma Detective's Guide
⚖️ Damage Assessment Matrix: Surgical Decision Architecture
Tissue viability assessment follows zone-based evaluation principles, where Zone 1 (cornea/anterior chamber) injuries have >90% salvage rates, Zone 2 (lens/anterior vitreous) injuries show 60-80% functional preservation, and Zone 3 (posterior retina/optic nerve) injuries carry <40% useful vision restoration potential.
📌 Remember: SAVE-IT for surgical decision criteria - Sight potential assessment, Anatomical integrity evaluation, Viability of tissues, Enucleation vs repair decision, Infection risk stratification, Timing optimization. Each factor has quantitative thresholds that determine surgical approach and expected outcomes.
| Damage Severity | Anatomical Findings | Functional Prognosis | Surgical Approach | Success Rate | Complication Risk |
|---|---|---|---|---|---|
| Grade 1 (Mild) | Superficial abrasions | VA >20/40 expected | Conservative management | >95% healing | <5% complications |
| Grade 2 (Moderate) | Partial thickness injury | VA 20/40-20/200 | Primary repair | 80-90% success | 10-15% complications |
| Grade 3 (Severe) | Full thickness laceration | VA 20/200-CF | Complex reconstruction | 60-75% success | 20-30% complications |
| Grade 4 (Critical) | Multiple zone involvement | VA CF-LP | Salvage procedures | 30-50% success | 40-60% complications |
| Grade 5 (Devastating) | Globe disruption | NLP likely | Enucleation consideration | <20% vision | >70% complications |
⭐ Clinical Pearl: The "Golden Hour" concept applies to chemical burns and globe ruptures, where intervention within 60 minutes significantly improves outcomes. Chemical irrigation effectiveness decreases exponentially after 30 minutes, while globe repair success rates drop 15-20% for each 6-hour delay.
- Surgical Complexity Stratification
- Simple Repairs (<2 hours operative time)
- Corneal lacerations <5mm with regular wound edges
- Conjunctival tears without underlying scleral involvement
- Lid margin repairs with <25% tissue loss
- Complex Reconstructions (2-4 hours operative time)
- Scleral lacerations >10mm with uveal prolapse
- Lens capsule ruptures requiring cataract extraction
- Retinal detachments with proliferative vitreoretinopathy
- Salvage Procedures (>4 hours operative time)
- Multiple zone injuries with >50% tissue loss
- Posterior segment reconstruction with silicone oil tamponade
- Orbital reconstruction with synthetic implants
- Simple Repairs (<2 hours operative time)
💡 Master This: "Enucleation criteria" include no light perception with extensive tissue destruction, >50% scleral laceration, complete lens extrusion, and posterior segment disruption. Evisceration preserves orbital volume but carries sympathetic ophthalmia risk of 0.1-0.2%.
Infection prevention protocols require broad-spectrum antibiotics within 2 hours of injury, tetanus prophylaxis updates, and surgical debridement of devitalized tissue. Endophthalmitis prophylaxis uses intravitreal antibiotics for high-risk penetrating injuries with >90% prevention efficacy.
Outcome prediction models incorporate initial visual acuity, wound location, tissue loss extent, and time to repair to calculate final vision probability. The Ocular Trauma Score provides 85-90% accuracy for 6-month visual outcomes across all injury types.
Connect these surgical decision frameworks through evidence-based treatment protocols to understand how intervention timing and technique selection optimize visual rehabilitation outcomes.
⚖️ Damage Assessment Matrix: Surgical Decision Architecture
🔧 Treatment Protocol Mastery: Evidence-Based Intervention Arsenal
Treatment protocol selection follows injury-specific algorithms that integrate damage severity, anatomical location, patient factors, and resource availability. Level 1 evidence supports specific interventions for each trauma category, with outcome improvements ranging from 15-40% when protocols are followed systematically.

📌 Remember: TREAT-NOW for immediate interventions - Tetanus prophylaxis, Rigid eye shield, Emergent irrigation, Antibiotic prophylaxis, Time-sensitive surgery, Neurologic assessment, Ophthalmology consultation, Wound protection. Each intervention has specific time windows for maximum effectiveness.
| Treatment Category | Intervention Protocol | Evidence Level | Success Rate | Time Window | Monitoring Requirements |
|---|---|---|---|---|---|
| Chemical Burns | pH neutralization + irrigation | Level 1 | 85-95% if <30 min | Immediate | pH q15min x 2 hours |
| Globe Rupture | Shield + emergent repair | Level 1 | 60-80% if <6 hours | <2 hours | IOP q4h x 48 hours |
| Penetrating Injury | Antibiotics + surgical repair | Level 1 | 70-85% if <8 hours | <6 hours | Infection signs q8h |
| Blunt Trauma | IOP control + monitoring | Level 2 | 80-90% prevention | <24 hours | IOP daily x 1 week |
| Thermal Burns | Cooling + lubrication | Level 2 | 75-85% healing | <1 hour | Epithelial healing q2d |
⭐ Clinical Pearl: "Steroid timing" is critical in trauma management - contraindicated in suspected infection or epithelial defects, but beneficial for traumatic uveitis after 48-72 hours. Prednisolone acetate 1% every 4 hours reduces inflammatory complications by 30-40% when used appropriately.
- Phase-Based Treatment Approach
- Acute Phase (0-72 hours)
- Globe stabilization with rigid shields and head elevation 30 degrees
- Pain management using topical anesthetics (proparacaine 0.5%) and systemic analgesics
- Infection prevention with antibiotic prophylaxis and wound cleansing
- IOP management avoiding carbonic anhydrase inhibitors in suspected rupture
- Subacute Phase (3-14 days)
- Inflammation control with topical steroids after infection clearance
- Wound healing optimization using artificial tears and protective measures
- Complication monitoring for secondary glaucoma and retinal detachment
- Chronic Phase (>2 weeks)
- Visual rehabilitation with optical correction and low vision aids
- Surgical reconstruction for persistent defects and functional limitations
- Long-term monitoring for delayed complications and sympathetic ophthalmia
- Acute Phase (0-72 hours)
💡 Master This: "Sympathetic ophthalmia prevention" requires enucleation within 14 days of no light perception injuries with extensive uveal involvement. Risk factors include delayed repair, retained foreign material, and chronic inflammation. Incidence is 0.2-0.5% but bilateral blindness occurs in 65% of cases.
Pain management protocols balance patient comfort with diagnostic accuracy. Topical anesthetics provide immediate relief but mask protective reflexes and delay healing. Systemic analgesics (acetaminophen 1000mg q6h + ibuprofen 600mg q8h) provide effective pain control without compromising examination.
Surgical technique optimization includes microsurgical approaches for corneal repairs, vitreoretinal techniques for posterior segment injuries, and oculoplastic methods for lid reconstruction. Success rates improve 20-30% with subspecialty expertise and appropriate instrumentation.
Complication prevention strategies target infection (<5% incidence with proper prophylaxis), glaucoma (10-20% risk in angle recession), and retinal detachment (15-25% risk in posterior injuries). Early recognition and prompt treatment reduce permanent vision loss by 40-60%.
Connect these evidence-based treatment protocols through systematic rehabilitation approaches to understand how comprehensive care optimizes long-term visual outcomes and quality of life restoration.
🔧 Treatment Protocol Mastery: Evidence-Based Intervention Arsenal
🎯 Rehabilitation Roadmap: Vision Recovery Architecture
Visual rehabilitation protocols follow evidence-based progression from basic light perception to complex visual tasks, with measurable milestones at 2-week intervals. Success rates vary from 85-95% for mild injuries to 30-50% for severe trauma, but systematic rehabilitation improves outcomes by 25-40% across all severity levels.

📌 Remember: RESTORE for rehabilitation components - Refraction optimization, Eye movement training, Sensory substitution, Technology integration, Orientation mobility, Reading skills, Emotional support. Each component requires specific timeframes and measurable objectives for maximum benefit.
| Rehabilitation Phase | Duration | Primary Goals | Success Metrics | Technology Tools | Expected Outcomes |
|---|---|---|---|---|---|
| Acute Recovery | 0-6 weeks | Wound healing + basic function | VA improvement >2 lines | Protective devices | 85-90% achieve goals |
| Early Adaptation | 6-12 weeks | Visual skills training | Reading speed >50 wpm | Magnification aids | 70-80% achieve goals |
| Skill Development | 3-6 months | Complex task mastery | ADL independence >80% | Electronic aids | 60-70% achieve goals |
| Long-term Optimization | 6-12 months | Vocational readiness | Return to work >60% | Computer adaptations | 40-60% achieve goals |
| Maintenance | Ongoing | Function preservation | Stable performance | Updated technology | >90% maintain gains |
⭐ Clinical Pearl: "Eccentric viewing training" teaches patients to use peripheral retina when central vision is compromised. Success rates reach 75-85% with structured training, improving reading speed by 150-200% and mobility confidence by 60-80% within 3-6 months.
- Comprehensive Rehabilitation Components
- Visual Function Assessment (baseline + monthly)
- Visual acuity measurement using ETDRS charts for precise tracking
- Visual field testing with Goldmann perimetry for functional mapping
- Contrast sensitivity evaluation using Pelli-Robson charts for real-world correlation
- Color vision testing with Ishihara plates for occupational planning
- Adaptive Skills Training (weekly sessions x 12 weeks)
- Orientation and mobility with white cane techniques and guide dog training
- Activities of daily living including cooking, cleaning, and personal care
- Communication skills using Braille, large print, and audio formats
- Technology proficiency with smartphones, computers, and assistive devices
- Visual Function Assessment (baseline + monthly)
💡 Master This: "Neuroplasticity windows" are most active in the first 6 months post-injury, when visual cortex reorganization can improve functional outcomes by 30-50%. Intensive training during this period using perceptual learning techniques maximizes recovery potential.
Psychological support protocols address depression (40-60% incidence), anxiety (30-50% incidence), and adjustment disorders (70-80% incidence) that commonly follow severe visual loss. Cognitive behavioral therapy combined with peer support groups reduces psychological distress by 40-60% and improves rehabilitation compliance by 25-35%.
Vocational rehabilitation focuses on workplace modifications, job retraining, and career transition support. Return-to-work rates vary from 80-90% for mild injuries to 30-40% for severe vision loss, but comprehensive programs improve employment outcomes by 20-30% across all categories.
Family education and caregiver training are essential components, as family support correlates with better rehabilitation outcomes and higher quality of life scores. Training programs lasting 4-6 sessions improve family coping by 50-70% and reduce patient dependence by 30-40%.
This comprehensive rehabilitation framework transforms trauma survivors from passive patients into active participants in their visual recovery journey, maximizing functional independence and quality of life regardless of injury severity.
🎯 Rehabilitation Roadmap: Vision Recovery Architecture
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app








