Ocular Drug Toxicity: Intro - Eye Trouble Origins
- Systemic medications can affect any ocular structure: cornea, lens, retina, optic nerve.
- Mechanisms of damage:
- Direct cellular toxicity.
- Hypersensitivity reactions.
- Idiosyncratic responses.
- Indirect effects (e.g., tear film alteration, ↑IOP).
- Risk factors: dose, duration of use, patient susceptibility (e.g., genetics, renal/hepatic status).
⭐ Many drugs, like chloroquine and thioridazine, bind to melanin in the uveal tract (iris, ciliary body, choroid), leading to accumulation and potential toxicity over time (uveal toxicity).
Corticosteroids: Ocular Effects - Sneaky Sight-Stealers
- Posterior Subcapsular Cataract (PSC): Most common; dose & duration-dependent. Irreversible.
- Steroid-induced Glaucoma: ↑IOP, mimics POAG; higher risk with topical, genetic predisposition.
- Central Serous Chorioretinopathy (CSCR): Can precipitate or worsen existing.
- Infections: Increased risk & severity (e.g., HSV keratitis reactivation, fungal keratitis).
- Delayed Wound Healing: Especially post-ocular surgery.
- Papilledema: Rare, associated with rapid withdrawal (pseudotumor cerebri).
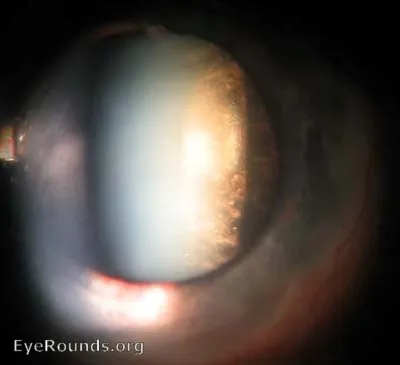
⭐ PSC is the most common ocular side effect of long-term systemic corticosteroid use.
Antimalarials: Retinopathy - Bullseye Beware!
- Chloroquine (CQ) & Hydroxychloroquine (HCQ) can cause irreversible retinopathy.
- Classic sign: Bull's eye maculopathy (late stage).
- Risk factors:
- HCQ dose > 5 mg/kg/day (actual body weight)
- CQ dose > 2.3 mg/kg/day
- Duration of use > 5 years
- Cumulative dose (e.g., HCQ > 1000g)
- Renal disease, tamoxifen co-therapy.
- Screening: Baseline exam within 1st year, then annual screening after 5 years of use (or earlier if high risk).
- Key tests: SD-OCT (detects earliest changes), automated visual fields (10-2).

⭐ Early HCQ retinopathy often manifests as parafoveal RPE disruption or loss of the photoreceptor inner/outer segment junction on SD-OCT (e.g., "flying saucer sign") before visual symptoms or the classic bull's eye maculopathy appears funduscopically. This makes SD-OCT crucial for early detection.
Ethambutol & Amiodarone: Toxicities - Nerve & Cornea Concerns
- Ethambutol:
- Optic neuropathy (retrobulbar neuritis); dose-dependent (>15-25 mg/kg/day).
- Symptoms: ↓ VA, red-green dyschromatopsia, central/centrocaecal scotoma.
- Reversible if detected early; regular vision monitoring is crucial.
- 📌 "E"thambutol affects "E"yes (optic nerve).
- Amiodarone:
- Corneal deposits (vortex keratopathy/cornea verticillata); common, dose-related.
- Usually asymptomatic or mild (halos, glare); reversible upon discontinuation.
- Optic neuropathy (NAION-like) is rare but serious.
⭐ Amiodarone-induced vortex keratopathy, though common (seen in >70% of patients on long-term therapy), rarely causes significant visual impairment.
Other Systemic Drugs: Ocular Risks - Diverse Eye Dramas
| Drug | Key Ocular Side Effect(s) |
|---|---|
| Digoxin | Xanthopsia (yellow halos), chromatopsia, blurred vision, "snowy" vision |
| Phenothiazines | Pigmentary retinopathy (Thioridazine >800mg/day), corneal/lens deposits (Chlorpromazine) |
| Tamoxifen | Crystalline retinopathy, macular edema, subcapsular cataracts, corneal changes |
| Amiodarone | Vortex keratopathy (corneal verticillata), optic neuropathy (rare) |
| Sildenafil | Cyanopsia (blue vision), photophobia, blurred vision, NAION risk |
| Isotretinoin | Severe dry eye, blepharoconjunctivitis, ↓night vision, corneal opacities |
Drug Toxicity: Monitoring - Safe Sight Steps
- Pre-Tx: Baseline exam (VA, fundus, special tests). Counsel on symptoms.
- On-Tx: Drug-specific scheduled follow-ups & testing.
- Action: Suspected toxicity? Confirm, stop/modify drug with prescriber, manage.
⭐ Hydroxychloroquine: Annual screening (SD-OCT, VF 10-2) after 5 yrs use, or earlier if high risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Chloroquine/HCQ: Bull's eye maculopathy (irreversible retinal toxicity), corneal verticillata (reversible).
- Ethambutol: Dose-dependent optic neuropathy; presents as retrobulbar neuritis, red-green dyschromatopsia.
- Amiodarone: Corneal verticillata (whorl-like keratopathy, most common), optic neuropathy (less common).
- Corticosteroids: Posterior subcapsular cataract (PSC), ↑IOP leading to steroid-induced glaucoma.
- Tamoxifen: Crystalline retinopathy (refractile deposits), macular edema, corneal opacities.
- Vigabatrin: Bilateral, irreversible, concentric visual field constriction; regular perimetry essential.
- Digitalis: Xanthopsia (yellow-tinged vision), chromatopsia, blurred vision, scotomas.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

