Diabetes Mellitus - Sugar-Coated Sight Stealers
Pathophysiology: Chronic hyperglycemia → sorbitol pathway, Advanced Glycation End-products (AGEs) → microvascular damage, osmotic stress.
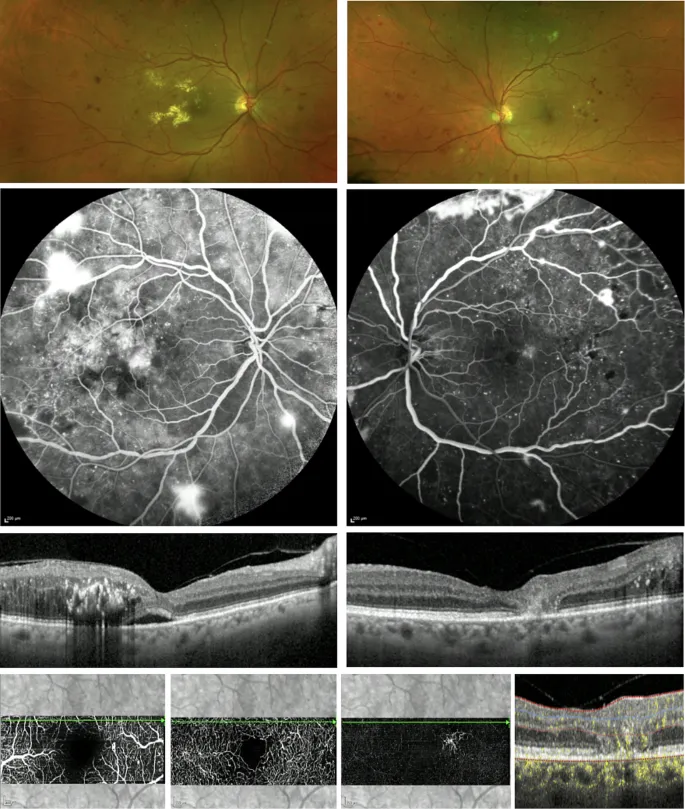
Diabetic Retinopathy (DR)
- Non-Proliferative DR (NPDR):
- Microaneurysms (earliest sign)
- Dot & blot hemorrhages, hard exudates
- Cotton Wool Spots (CWS), Intraretinal Microvascular Abnormalities (IRMA)
- Severe NPDR: 📌 4:2:1 rule (hemorrhages/microaneurysms in 4 quadrants, venous beading in 2 quadrants, IRMA in 1 quadrant)
- Proliferative DR (PDR):
- Neovascularization: NVD (disc), NVE (elsewhere)
- Vitreous hemorrhage, tractional retinal detachment (TRD)
- Diabetic Macular Edema (DME)/Clinically Significant Macular Edema (CSME): Major cause of visual loss in diabetics.
Other Ocular Manifestations
- Cataract: True diabetic "snowflake" cataract (acute, young Type 1 DM); earlier onset & progression of senile cataract.
- Refractive changes: Transient hyperopic or myopic shifts.
- Cranial nerve palsies: III (often pupil-sparing), IV, VI.
- Rubeosis iridis, neovascular glaucoma.
⭐ Diabetic retinopathy is the leading cause of new blindness in adults aged 20-74 years.
Wilson, Galactosemia, Cystinosis - Copper, Crystals, Cataracts
-
Wilson's Disease (ATP7B gene)
- Kayser-Fleischer (K-F) ring: Copper in Descemet's membrane (superiorly first).
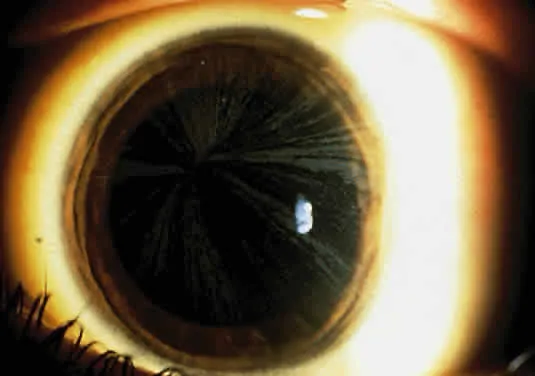
- Sunflower cataract (anterior/posterior subcapsular).
- 📌 Mnemonic: Copper Is HEavy MEtal (K-F ring, Hepatitis, Extrapyramidal, MEmory).
⭐ The Kayser-Fleischer ring in Wilson's disease is a golden-brown copper deposit in Descemet's membrane, best seen with gonioscopy.
-
Galactosemia (GALT/GALK/GALE deficiency)
- Oil-drop cataract: Reversible, due to galactitol accumulation. Onset often within first few days/weeks of life.
- Nuclear and cortical changes.
-
Cystinosis (CTNS gene)
- Corneal crystals: Iridescent, needle-shaped cystine crystals in stroma.
- Photophobia, retinopathy.
- Nephropathic form most common.
Fabry, MPS, Homocystinuria - Storage & Structural Snafus
- Fabry's Disease (GLA gene, α-galactosidase A deficiency)
- Cornea verticillata (whorl-like) 📌 Fabry's Whorls
- Posterior spoke-like cataract
- Vascular tortuosity (conjunctival/retinal)
- Mucopolysaccharidoses (MPS) (GAG accumulation)
- Corneal clouding (e.g., Hurler, Scheie)
- Retinal degeneration/pigmentary retinopathy (e.g., Hunter)
- Optic atrophy, glaucoma
- Homocystinuria (CBS gene defect)
- Ectopia lentis: inferonasal, bilateral
⭐ Inferonasal lens subluxation is characteristic of homocystinuria, contrasting with the superotemporal subluxation seen in Marfan syndrome.
- Marfanoid habitus, ↑ thromboembolism risk
- Glaucoma, optic atrophy
- 📌 LENS: Lens subluxation (down & in), INtellectual disability, N aracnodactyly, Stroke.
- Ectopia lentis: inferonasal, bilateral
Hyperlipidemia, Albinism, Gout - Lipid, Light & Purine Alerts
- Hyperlipoproteinemias:
- Lipemia retinalis: Creamy retinal vessels (triglycerides > 2500 mg/dL).
- Corneal arcus (senilis/juvenilis): Peripheral corneal lipid deposit.
- Xanthelasma: Yellowish eyelid plaques.
- Albinism: (TYR gene for OCA1)
- Types: Oculocutaneous (OCA) & Ocular (OA).
- Key signs: Foveal hypoplasia, nystagmus, iris transillumination, photophobia, ↓ visual acuity, abnormal optic nerve fiber decussation.
⭐ Foveal hypoplasia is the primary determinant of poor visual acuity in individuals with albinism.
- Gout/Hyperuricemia:
- Urate crystal deposition: Cornea, conjunctiva, sclera.
- Ocular signs: Band keratopathy, uveitis, scleritis.
- Eyelid tophi.
A collage displaying lipemia retinalis, corneal arcus, xanthelasma, ocular signs of albinism like iris transillumination, and gouty tophi or band keratopathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Diabetes Mellitus: Key risks are diabetic retinopathy (NPDR/PDR) and macular edema.
- Wilson's Disease: Presents with Kayser-Fleischer ring (corneal copper) and sunflower cataract.
- Galactosemia: Characterized by oil-droplet cataracts in infants, often reversible.
- Fabry Disease: Look for cornea verticillata (whorled keratopathy) and posterior spoke cataracts.
- Homocystinuria: Causes inferonasal lens subluxation (ectopia lentis).
- Thyroid Eye Disease: Features proptosis, diplopia, lid retraction, and optic neuropathy.
- Mucopolysaccharidoses: Often show progressive corneal clouding and retinal degeneration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

