Hypertensive Retinopathy: Pathophysiology - Eye Under Pressure
- Chronic ↑ systemic blood pressure (BP) overwhelms retinal autoregulatory mechanisms.
- Vasoconstrictive Phase (Early):
- Initial response: retinal arterioles undergo vasospasm and diffuse/focal narrowing.
- Changes are often reversible if BP is controlled promptly.
- Sclerotic/Exudative Phase (Chronic):
- Prolonged ↑ BP leads to endothelial damage and thickening/hyalinization of arteriolar walls (arteriolosclerosis).
- Breakdown of the blood-retinal barrier (BRB) causes ↑ vascular permeability.
- Results in: retinal hemorrhages, hard exudates (lipid deposits), and cotton wool spots (CWS; nerve fiber layer infarcts).
- Malignant Hypertension Phase (Severe):
- Fibrinoid necrosis of arterioles.
- Optic disc swelling (papilledema) may occur.
- Increased risk of retinal vascular occlusions.
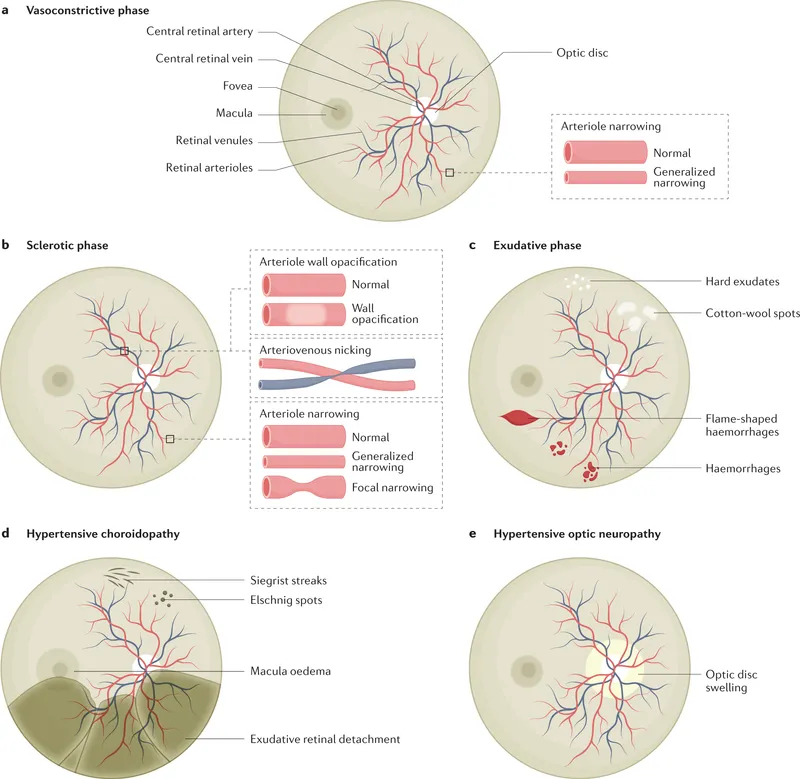
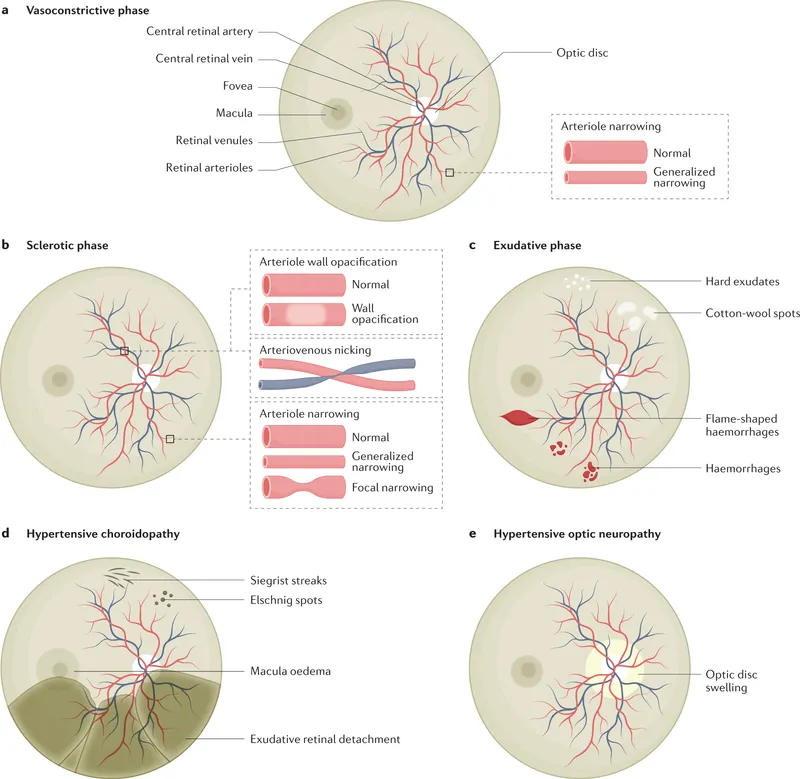
⭐ Cotton wool spots (CWS) are key indicators of retinal ischemia, representing an accumulation of axoplasmic debris in the nerve fiber layer due to obstruction of axoplasmic flow from arteriolar occlusion or severe narrowing aterioles and pre-capillary arterioles due to ischemia from severe hypertension
Hypertensive Retinopathy: KWB Classification - Staging the Strain
- Keith-Wagener-Barker (KWB) system grades severity of retinal changes due to hypertension.
- Grade 1:
- Mild, generalized arteriolar narrowing/attenuation.
- "Copper wiring" appearance of arterioles (broadened light reflex).
- Grade 2:
- More pronounced, focal arteriolar constriction.
- "Silver wiring" appearance (narrowed, sclerosed arterioles).
- Arteriovenous (AV) nipping or Salus' sign (venous constriction at AV crossings).
- Grade 3:
- Signs of Grade 2 PLUS:
- Retinal hemorrhages (flame-shaped, dot & blot).
- Cotton wool spots (soft exudates; nerve fiber layer infarcts).
- Hard exudates (lipid residues; often in a macular star pattern if severe).
- Grade 4: (Malignant Hypertension)
- Signs of Grade 3 PLUS:
- Papilledema (optic disc swelling).
⭐ Grade 4 KWB (papilledema) indicates malignant hypertension, an ophthalmic emergency requiring urgent systemic blood pressure control to prevent irreversible vision loss and systemic complications.
oka
Hypertensive Retinopathy: Fundus Findings - Red Alert Retina
- Early Changes (KWB Grades 1-2):
- Arteriolar narrowing: Generalized & focal.
- ↑ Arterial light reflex.
- Copper wiring (thickened wall, Grade 2).
- Silver wiring (severe sclerosis, advanced Grade 2 / 3).
- AV nipping (Gunn's sign), banking (Bonnet's sign), deflection (Salus' sign).
- Moderate to Severe Changes (KWB Grade 3):
- Retinal hemorrhages: Flame-shaped (NFL), dot & blot.
- Cotton Wool Spots (CWS): NFL infarcts, sign of ischemia.
- Hard exudates: Lipid deposits, may form macular star.
- Retinal edema.
- Malignant Hypertension (KWB Grade 4):
- All Grade 3 signs + Optic disc swelling (papilledema).
- Elschnig spots (choroidal infarcts) may be present.
- 📌 Mnemonic for severe signs: "HERO" - Hemorrhages, Exudates (hard & CWS), Retinal Edema, Optic disc swelling.
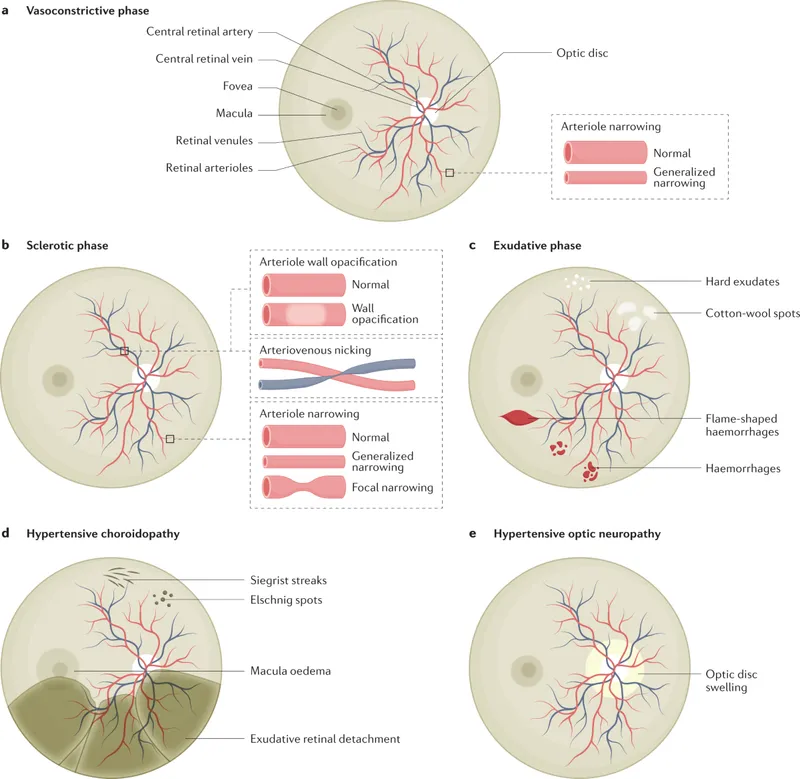
⭐ Papilledema in hypertensive retinopathy (KWB Grade 4) is an ophthalmic emergency, indicating malignant hypertension and risk of systemic organ damage.
Ocular Effects of HTN: Complications & Management - Crisis Control
- Hypertensive Choroidopathy: Elschnig spots (RPE infarcts), Siegrist streaks (sclerosed vessels); indicates severe/acute HTN.
- Hypertensive Optic Neuropathy: Papilledema (malignant HTN), or AION-like picture.
- Vascular Events: ↑ Risk: Retinal Arterial Macroaneurysms (RAM), BRVO, CRVO, BRAO, CRAO.
- Crisis Management:
- Systemic: Urgent, controlled BP reduction (avoid hypoperfusion).
- Ocular: Treat sequelae (e.g., anti-VEGF for edema, laser for RAM).
⭐ Bilateral serous retinal detachments can occur in hypertensive crisis due to severe choroidopathy (Elschnig spots, Siegrist streaks).
High‑Yield Points - ⚡ Biggest Takeaways
- Hypertensive retinopathy is graded using the Keith-Wagener-Barker (KWB) classification.
- Early signs include generalized arteriolar narrowing, focal constrictions, and silver/copper wiring.
- Arteriovenous (AV) nipping is a hallmark finding.
- Cotton wool spots, flame-shaped hemorrhages, and hard exudates indicate advancing retinopathy.
- Papilledema (Grade IV KWB) signifies malignant hypertension and is an ocular emergency.
- Elschnig spots represent choroidal infarcts in severe, acute hypertension.
- Primary management is strict systemic blood pressure control to reverse changes and prevent vision loss.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

