Anemias & Ocular Signs - Pale Views
- Conjunctival pallor: Most common; check lower palpebral conjunctiva.
- Fundoscopic Changes (due to retinal hypoxia):
- Generalized retinal pallor.
- Retinal hemorrhages: All layers; flame-shaped (NFL), dot & blot (INL/OPL).
- Cotton wool spots (CWS): Focal ischemia causing axoplasmic debris.
- Roth spots: Hemorrhages with white centers (platelet-fibrin, cells).
- Venous tortuosity and dilation.
- Optic disc edema: Seen in severe anemia (e.g., Hb < 5-7 g/dL).
- Pernicious Anemia (B12 deficiency): May cause optic neuropathy.
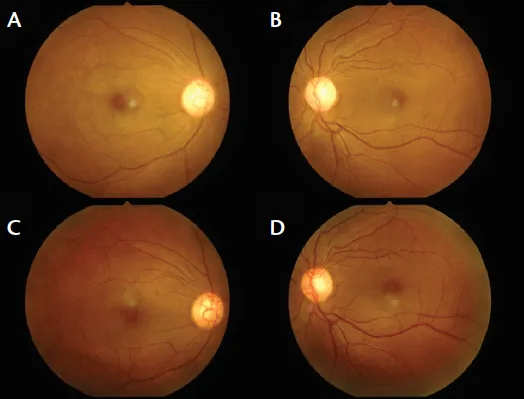
⭐ In severe chronic anemia, particularly with Hb levels below 5 g/dL, bilateral retinal hemorrhages and even papilledema can occur due to a combination of hypoxia and hyperdynamic circulation.
Leukemias/Lymphomas - Eye Infiltrates
- Leukemic Retinopathy: Commonest ocular finding.
- Features: Retinal hemorrhages (all layers), cotton wool spots, Roth spots.
- Vascular changes: Venous dilation/tortuosity, perivascular sheathing.
- Peripheral neovascularization (rare).
- Direct Infiltration by Leukemic Cells:
- Orbit: Proptosis (esp. AML - chloroma/granulocytic sarcoma; childhood ALL).
- Uvea: Iritis, pseudohypopyon (leukemic cells), diffuse choroidal infiltration (yellowish-pink).
- Optic Nerve: Swelling, infiltration, subsequent atrophy.
- Lymphoma-Specific:
- Primary Intraocular Lymphoma (PIOL): Often B-cell, associated with CNS lymphoma. Presents as chronic uveitis, vitritis, sub-RPE infiltrates; a masquerade syndrome.
- Orbital Lymphoma: Typically painless proptosis in older adults.
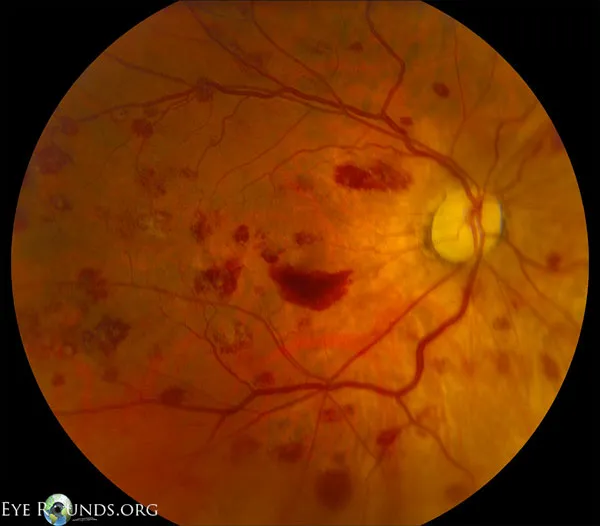
⭐ Optic nerve infiltration in Acute Lymphoblastic Leukemia (ALL) can be an early sign of CNS relapse and carries a poor prognosis.
Hyperviscosity & Polycythemia - Thick Blood, Bad Sight
- Pathophysiology: ↑ blood viscosity (hyperviscosity syndromes like Waldenström's macroglobulinemia, multiple myeloma) or ↑ RBC mass (polycythemia vera) → impaired microcirculation.
- Ocular Features (often bilateral):
- Retinal Veins: Dilation, tortuosity, segmentation ("sausage-link" or "boxcar" appearance).
- Fundus: Dark red/plethoric (esp. polycythemia), retinal hemorrhages (flame, dot/blot), cotton wool spots, microaneurysms.
- Optic Disc: Papilledema, hyperemic disc.
- Vascular Occlusions: ↑ risk of CRVO, BRVO, CRAO.
- Symptoms: Blurred vision, transient visual obscurations (amaurosis fugax), diplopia.
- Anterior Segment: Conjunctival sludging, plethora, secondary glaucoma (rare).
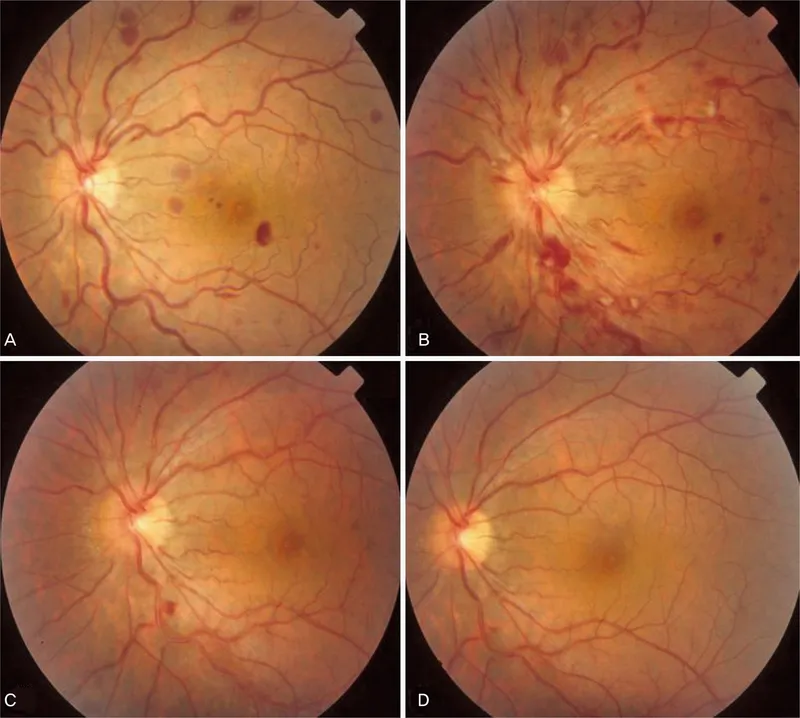
⭐ "Sausage-link" appearance (fundus varicosities) of retinal veins is a classic sign of hyperviscosity retinopathy.
Bleeding & Clotting Issues - Hemorrhage Havoc
- Thrombocytopenia (platelet count < 150,000/μL):
- Retinal hemorrhages (dot, blot, flame-shaped)
- Subconjunctival hemorrhage
- Roth spots (hemorrhage with white center)
- Vitreous hemorrhage (rare)
- Hyphema
- Disseminated Intravascular Coagulation (DIC):
- Widespread microvascular thrombosis & secondary fibrinolysis.
- Ocular: Similar to thrombocytopenia; choroidal infarcts, exudative retinal detachment.
- Often bilateral, severe visual loss.
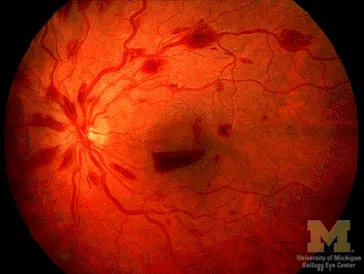
⭐ Roth spots, though non-specific, are classically associated with bacterial endocarditis but can be seen in various hematological disorders causing retinal hemorrhages, including leukemia and severe anemia.
- Other coagulopathies (e.g., Hemophilia, Von Willebrand disease):
- Spontaneous subconjunctival hemorrhage
- Orbital hematoma (post-trauma risk ↑)
- Hyphema
High‑Yield Points - ⚡ Biggest Takeaways
- Sickle Cell Retinopathy: Sea-fan neovascularization is pathognomonic; also salmon-patch hemorrhages, black sunbursts.
- Leukemia: Key signs: Roth spots, retinal hemorrhages, optic nerve infiltration, sometimes proptosis.
- Severe Anemia: Presents with pale conjunctiva, retinal hemorrhages, and cotton wool spots.
- Polycythemia Vera: Features conjunctival/retinal plethora, engorged tortuous veins, and possible papilledema.
- Hyperviscosity Syndromes (Myeloma, Waldenström's): Cause retinopathy with venous tortuosity ("sausage-link" appearance), hemorrhages.
- Thrombocytopenia: Associated with subconjunctival and retinal hemorrhages.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

