Skin-Eye Connection - Kindred Tissues
- Shared Embryology: Skin & eye structures derive from common germ layers.
- Surface Ectoderm: Forms epidermis, corneal & conjunctival epithelium, lens.
- Neural Crest Cells: Contribute to dermis, uveal melanocytes, corneal stroma & endothelium.
- Clinical Link: Dermatological disorders frequently exhibit ocular signs due to this shared origin.
⭐ Neurocutaneous syndromes (phakomatoses) like Neurofibromatosis, Tuberous Sclerosis, Sturge-Weber syndrome classically show skin-eye co-manifestations.
SJS/TEN & Pemphigoid - Bubble Trouble Eyes
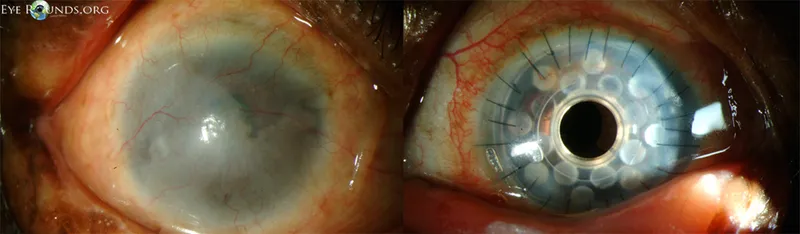
-
Stevens-Johnson Syndrome (SJS) / Toxic Epidermal Necrolysis (TEN)
- Acute, severe mucocutaneous reactions; often drug-induced (e.g., sulfonamides, anticonvulsants).
- Ocular: Acute bilateral conjunctivitis (papillary/membranous/pseudomembranous), lid edema, erosions, keratitis, corneal ulceration/perforation, symblepharon, ankyloblepharon, severe dry eye, trichiasis, entropion.
- Systemic: Fever, malaise, widespread blistering, mucosal involvement (oral, genital).
-
Ocular Cicatricial Pemphigoid (OCP)
- Chronic, autoimmune blistering disease affecting mucous membranes (Type II hypersensitivity).
- Ocular: Progressive conjunctival fibrosis, subepithelial bullae → scarring, symblepharon (key feature), ankyloblepharon, forniceal shortening, trichiasis, entropion, severe dry eye, corneal opacification, blindness.
- Systemic: Oral lesions (desquamative gingivitis), skin, other mucosae.
⭐ Symblepharon (adhesion between palpebral and bulbar conjunctiva) is a hallmark of both severe SJS/TEN sequelae and OCP, leading to restricted ocular motility and dry eye. Early intervention is critical to prevent long-term vision loss.
📌 SJS/TEN: Sudden Jolt Skin / Terrible Epidermal Necrosis. 📌 OCP: Old Cicatrices Persist (chronic scarring).
Atopy, Psoriasis, Rosacea - Inflamed Views
- Atopic Dermatitis (AD): Chronic, itchy skin inflammation.
- Ocular: Atopic keratoconjunctivitis (AKC), eyelid dermatitis/eczema, Dennie-Morgan folds (infraorbital), Hertoghe's sign (lateral eyebrow thinning).
- Complications: Keratoconus, anterior subcapsular cataracts, ↑ risk of retinal detachment.
⭐ AKC is a chronic, bilateral inflammation often associated with vernal-like shield ulcers and limbal Horner-Trantas dots.
- Psoriasis: Chronic inflammatory skin disease.
- Ocular: Chronic non-granulomatous anterior uveitis (most common, often HLA-B27+), conjunctivitis, blepharitis, dry eye, punctate keratitis, madarosis.
- Rosacea: Chronic facial dermatosis.
- Ocular: Ocular rosacea (affects up to 50-75% of patients), posterior blepharitis, meibomian gland dysfunction (MGD), recurrent chalazia/hordeola, marginal keratitis, stromal keratitis, conjunctival hyperemia.
Genodermatoses & Behçet's - Systemic Signs
- Xeroderma Pigmentosum (XP)
- DNA repair defect; ↑ UV sensitivity
- Systemic: Skin cancers (BCC, SCC, melanoma)
- Ichthyosis
- Keratinization disorder; dry, scaly skin
- Systemic: Sjögren-Larsson syndrome (spasticity, intellectual disability)
- Atopic Dermatitis (Eczema)
- Chronic inflammatory skin disease
- Systemic: Allergic rhinitis, asthma (atopic triad)
- Pseudoxanthoma Elasticum (PXE)
- Elastic fiber degeneration
- Systemic: Skin (yellow papules - neck, axillae); Cardiovascular (calcification, hemorrhage); GI bleeds
- Behçet's Disease
- Multisystem vasculitis
- Systemic: Recurrent oral & genital ulcers; Skin lesions (erythema nodosum, papulopustular lesions); Arthritis; GI/CNS involvement
- Pathergy test positive
⭐ Behçet's disease shows a strong association with HLA-B51.
High‑Yield Points - ⚡ Biggest Takeaways
- SJS/TEN: Severe drug reactions; cause cicatricial conjunctivitis, keratinization, symblepharon, severe dry eye.
- Atopic Dermatitis: Linked to atopic keratoconjunctivitis (AKC), anterior subcapsular cataracts, keratoconus.
- Ocular Rosacea: Features chronic blepharitis, MGD, recurrent chalazia, peripheral keratitis.
- Psoriasis: Associated with uveitis (anterior), conjunctivitis, blepharitis, dry eye.
- Ocular Cicatricial Pemphigoid: Autoimmune; causes progressive conjunctival scarring, symblepharon, corneal blindness.
- Xeroderma Pigmentosum: DNA repair defect; high risk of UV-induced ocular surface neoplasms and eyelid cancers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

