Sjögren's & KCS - Desert Eyes Drama
- Autoimmune disorder targeting exocrine glands (lacrimal, salivary) → Keratoconjunctivitis Sicca (KCS) & xerostomia.
- Primary Sjögren's: Sicca symptoms alone (dry eyes, dry mouth).
- Secondary Sjögren's: Associated with other autoimmune diseases (e.g., RA, SLE).
- KCS Symptoms: Dryness, grittiness, burning, foreign body sensation, photophobia, blurred vision.
- Signs: ↓ Tear film, conjunctival injection, corneal erosions (SPKs), filaments, mucus strands.
- Diagnosis: Key tests include:
- Schirmer's test: Measures tear production (<5mm in 5 min is significant).
- Tear Break-Up Time (TBUT): Assesses tear film stability (<10s is abnormal).
- Ocular surface staining: Rose Bengal, Lissamine Green highlight damaged cells.
- Serology: Anti-Ro (SSA) & Anti-La (SSB) antibodies.
- Management: Artificial tears, lubricating ointments, punctal occlusion, topical cyclosporine A, lifitegrast.
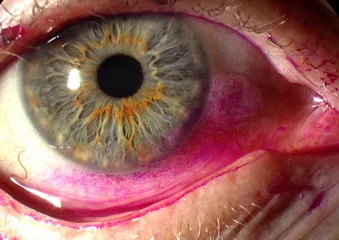
⭐ Schirmer's test I (without topical anesthesia) value of <5mm wetting in 5 minutes is a key diagnostic criterion for aqueous-deficient dry eye, often seen in Sjögren's syndrome.
Rheumatoid Arthritis - Joint & Eye Plight
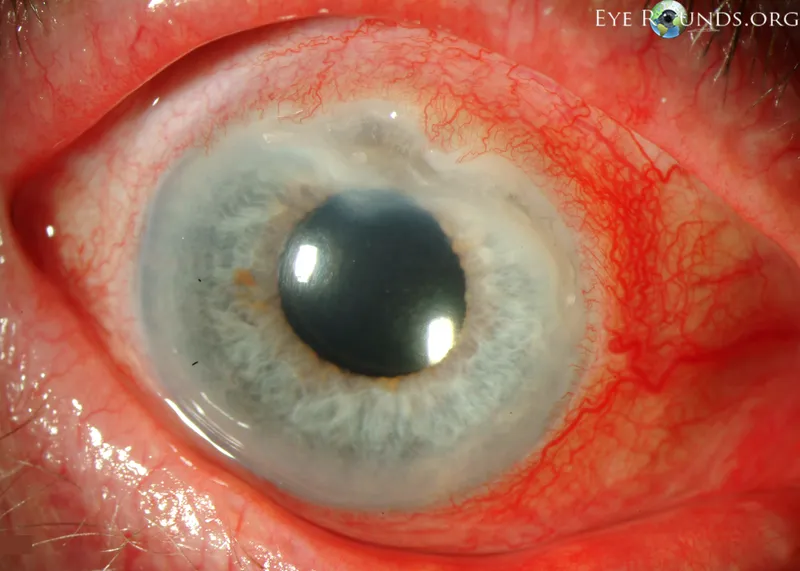
- Keratoconjunctivitis Sicca (KCS): Most common ocular manifestation; results in dry eyes.
- Scleritis: Severe, deep ocular pain. Anterior (diffuse/nodular) most common.
- Necrotizing scleritis: Most severe form; can lead to scleromalacia perforans (painless blue patches, perforation risk).
- Episcleritis: More common than scleritis; often recurrent, self-limiting.
- Peripheral Ulcerative Keratitis (PUK): Crescent-shaped stromal inflammation and thinning at limbus; "corneal melt". High perforation risk.
- Uveitis: Less frequent compared to spondyloarthropathies.
- 📌 Mnemonic: Sicca, Scleritis, PUK for RA.
⭐ Necrotizing scleritis in RA is a severe, sight-threatening condition that can lead to scleromalacia perforans, characterized by areas of scleral thinning and potential globe rupture.
Spondyloarthropathies & Uveitis - HLA-B27's Eye Ire
- Spondyloarthropathies (SpA): Inflammatory diseases (📌 PAIR: Psoriatic arthritis, Ankylosing spondylitis, IBD-arthritis, Reactive arthritis).
- Strong HLA-B27 link.
- Ocular Hallmark: Acute Anterior Uveitis (AAU).
- Most common extra-articular manifestation, esp. in Ankylosing Spondylitis (AS).
- Sudden: pain, redness, photophobia, ↓vision.
- Signs: Ciliary flush, keratic precipitates (KPs), AC cells/flare, hypopyon (sometimes).
- Typically non-granulomatous, recurrent, unilateral; may alternate eyes.
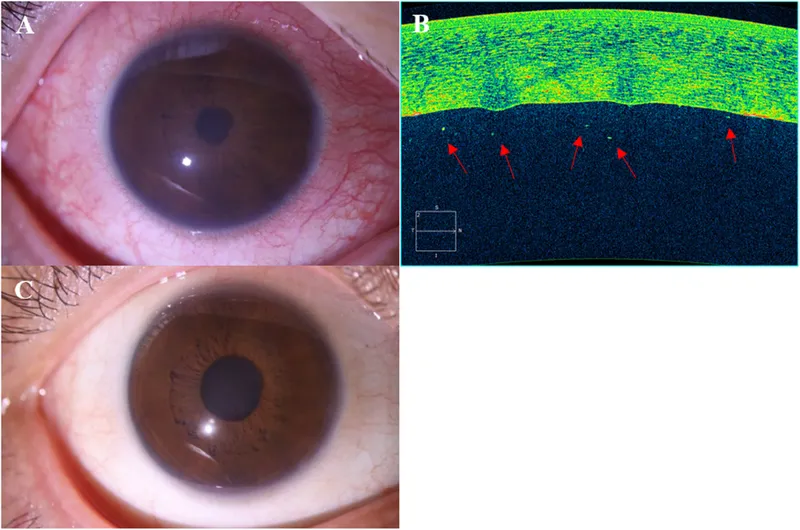
- Reactive Arthritis (Reiter's): Triad "Can't see, can't pee, can't climb a tree" (uveitis/conjunctivitis, urethritis, arthritis).
- Complications: Posterior synechiae, cataract, secondary glaucoma, cystoid macular edema.
⭐ In Ankylosing Spondylitis, AAU occurs in 25-40% of patients.
Giant Cell Arteritis - Vision's Urgent Fright
- Vasculitis of large/medium arteries; age >50 yrs (📌 50/50 rule: Age >50, ESR >50).
- Symptoms: New headache, jaw claudication, scalp tenderness, fever, PMR.
- Ocular EMERGENCY:
- AAION: Sudden, painless, severe vision loss.
- Amaurosis fugax, diplopia.
- Signs: Tender, pulseless temporal artery. AAION: Chalky-white swollen disc, APD.
- Dx: ↑ ESR (>50 mm/hr), ↑ CRP. Temporal Artery Biopsy (TAB) definitive. CDUS: "halo sign".
- Rx: URGENT! Start steroids BEFORE biopsy.
- IV Methylprednisolone (1g/day x 3d) for vision loss.
- Oral Prednisolone (1mg/kg/day).
⭐ Untreated GCA can lead to bilateral blindness in days to weeks; prompt high-dose steroids are vision-saving.
High‑Yield Points - ⚡ Biggest Takeaways
- Sjögren's Syndrome: Keratoconjunctivitis Sicca (KCS) is hallmark; positive Schirmer's/Rose Bengal staining.
- Rheumatoid Arthritis: Scleritis (especially necrotizing), episcleritis, KCS, and corneal melt (PUK).
- SLE: Lupus retinopathy (cotton wool spots, hemorrhages), optic neuropathy, and KCS.
- Ankylosing Spondylitis: Acute anterior uveitis (recurrent, unilateral, often HLA-B27 positive).
- Sarcoidosis: Granulomatous uveitis ("candle wax drippings", mutton-fat KPs), panuveitis, lacrimal gland involvement.
- Behçet's Disease: Recurrent hypopyon uveitis, retinal vasculitis, and occlusive vasculopathy.
- Giant Cell Arteritis: AION is a blinding risk; amaurosis fugax, ↑ESR, immediate high-dose steroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

