Pupil Anatomy & Physiology - Eye's Aperture Show
- Pupil: Central iris aperture; controls retinal light entry.
- Iris Muscles:
- Sphincter Pupillae: Circular fibers.
- Action: Miosis (constriction).
- Innervation: Parasympathetic (CN III, Edinger-Westphal nucleus → ciliary ganglion).
- Dilator Pupillae: Radial fibers.
- Action: Mydriasis (dilation).
- Innervation: Sympathetic (T1 → superior cervical ganglion).
- Sphincter Pupillae: Circular fibers.
- Size: Normal: 2-4 mm (light), 4-8 mm (dark).
- Anisocoria: Unequal pupils; physiological if < 1 mm difference.

⭐ The Edinger-Westphal nucleus provides preganglionic parasympathetic fibers for pupillary constriction via the ciliary ganglion.
Pupillary Reflexes - Pupil's Quick Dance
- Light Reflex: Pupil constricts in response to light.
- Afferent: CN II (Optic N.)
- Efferent: CN III (Oculomotor N. - Parasympathetic via Edinger-Westphal nucleus)
- Direct (same eye) & Consensual (opposite eye) response.
- Near Reflex Triad: For focusing on near objects.
- Accommodation (ciliary muscle contraction → lens thickens)
- Convergence (eyes move inwards)
- Miosis (pupil constriction)
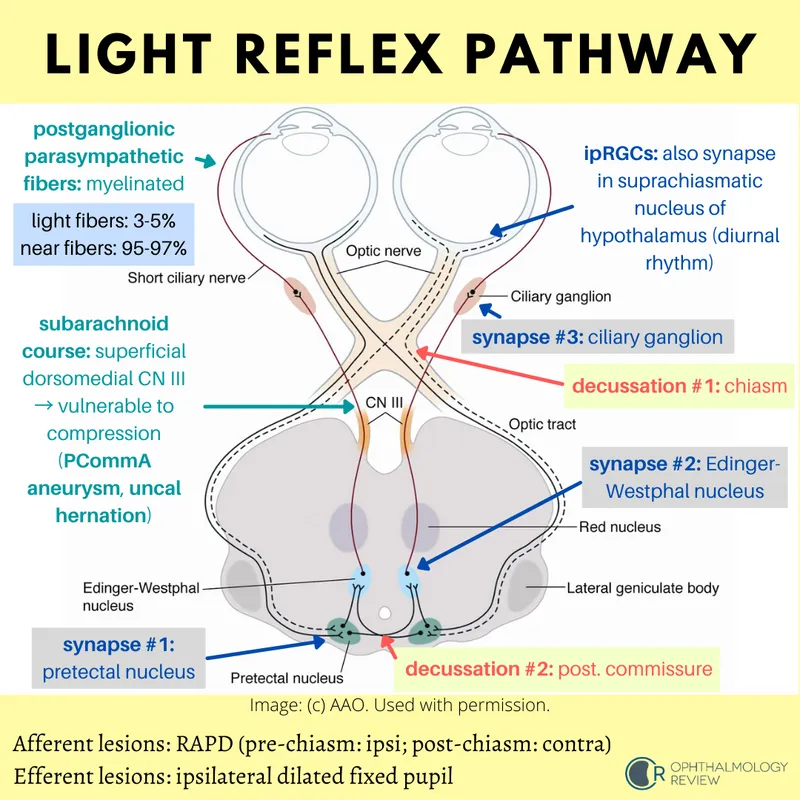
⭐ Relative Afferent Pupillary Defect (RAPD) / Marcus Gunn Pupil: Detected by swinging flashlight test; affected pupil dilates paradoxically or constricts less when light swings from normal to affected eye. Indicates optic nerve disease.
Afferent Pupillary Defect - Gunn's Flashy Clue
- A.k.a. Marcus Gunn Pupil (MGP) / Relative Afferent Pupillary Defect (RAPD).
- Indicates unilateral or asymmetric optic nerve (CN II) / severe retinal disease (pre-chiasmal).
- Mechanism: ↓ afferent input from affected eye → ↓ direct light reflex; consensual reflex intact.
- Swinging Flashlight Test:
- Light on normal eye: both pupils constrict.
- Swing to affected eye: affected pupil shows paradoxical dilation or reduced constriction.
- 📌 RAPD: Relative Afferent Pupil Defect.
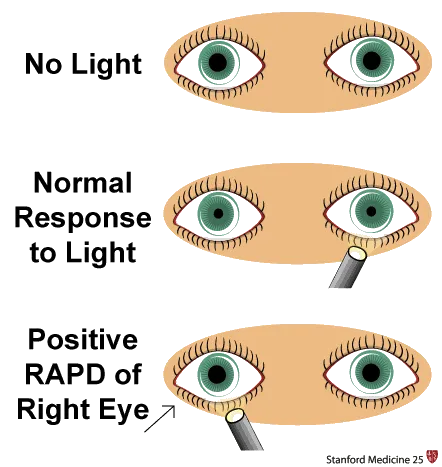
⭐ RAPD implies the lesion is anterior to the optic chiasm.
Efferent Pupillary Defects - Nerve Wreck Revels
Efferent defects disrupt pupil motor pathways (parasympathetic/sympathetic). 📌 Mnemonic: Nerve, Wreck, Revels.
-
CN III (Oculomotor) Palsy ("Nerve")
- Parasympathetic fiber damage → mydriasis.
- Features: Ptosis, "down & out" eye, dilated non-reactive pupil.
- Compressive (e.g., PCOM aneurysm): Painful, pupil involved.
- Microvascular (e.g., DM, HTN): Pupil often spared.
⭐ Painful CN III palsy + Mydriasis = Posterior Communicating Artery (PCOM) aneurysm until proven otherwise.
-
Adie's Tonic Pupil ("Wreck")
- Ciliary ganglion/short ciliary nerve lesion (often idiopathic/post-viral).
- Features: Unilateral mydriasis, poor light reaction, light-near dissociation (better near constriction). Vermiform iris movements.
- Test: Constriction with dilute pilocarpine (0.1% or 0.125%) due to denervation hypersensitivity.
-
Horner's Syndrome ("Revels")
- Sympathetic pathway disruption (oculosympathetic paresis).
- Triad: Miosis (constricted pupil), mild ptosis (~2mm), anhidrosis (variable).
- Tests:
- Cocaine 4%: Fails to dilate Horner's pupil (confirms).
- Apraclonidine 0.5% or 1%: Dilates Horner's pupil (reversal of anisocoria, confirms).

Specific Pupillary Syndromes - Peculiar Peepers Parade
- Adie's Tonic Pupil: Unilateral dilated pupil; light-near dissociation (LND). Young women, ↓ DTRs (Holmes-Adie).
⭐ Shows cholinergic supersensitivity: constricts to dilute (0.125%) pilocarpine.
- Argyll Robertson Pupil (ARP): Bilateral small, irregular pupils; LND. 📌 ARP: Accom. Reflex Present, Pupil. Reflex Absent. Strong neurosyphilis link.
- Marcus Gunn Pupil (RAPD): Optic nerve lesion. Affected eye dilates: swinging flashlight test.
- Hutchinson's Pupil: Unilateral fixed, dilated pupil; CN III compression (uncal herniation).
High‑Yield Points - ⚡ Biggest Takeaways
- Marcus Gunn Pupil (APD) indicates optic nerve disease; paradoxical dilation with swinging flashlight test.
- Argyll Robertson Pupil shows light-near dissociation (accommodates, no light reaction); classic for neurosyphilis.
- Adie's Tonic Pupil: Dilated pupil, poor light reaction, slow near response, often with absent deep tendon reflexes.
- Horner's Syndrome: Triad of miosis, ptosis, and anhidrosis due to sympathetic pathway lesion.
- Third Nerve Palsy: Mydriasis with ptosis and "down and out" gaze suggests compression (e.g., aneurysm).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

