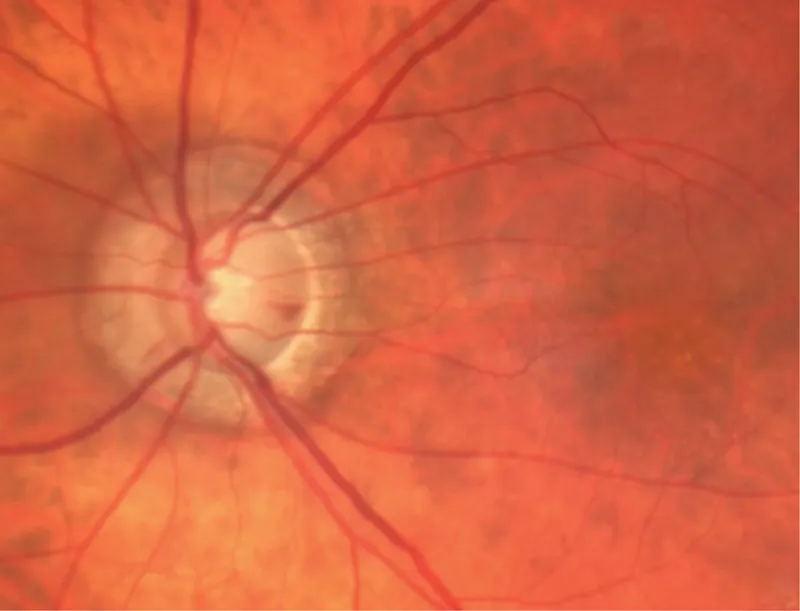
Papilledema - Swollen Disc Genesis
- Definition: Optic disc swelling due to elevated Intracranial Pressure (ICP).
Pathophysiology
- ↑ ICP transmits to optic nerve subarachnoid space.
- Compression of optic nerve fibers.
- Impedes axoplasmic flow (orthograde & retrograde stasis).
- Obstructs retinal venous outflow → venous engorgement, hemorrhages, exudates.
- Results in axonal swelling, intraneuronal ischemia, and optic disc edema.

⭐ Papilledema implies raised intracranial pressure and is typically bilateral, though may be asymmetrical.
Key Features
- Usually bilateral, can be asymmetric.
- Initially, visual acuity often preserved.
- Enlarged blind spot is an early sign.
- Transient visual obscurations may occur.
Papilledema - Eye Spy Swelling
-
Definition: Optic disc swelling due to ↑ Intracranial Pressure (ICP). Usually bilateral.
-
Pathophysiology: ↑ ICP → impaired axoplasmic flow in optic nerve → axonal swelling.
-
Symptoms:
- Headache (worse on waking, Valsalva)
- Nausea, vomiting
- Transient Visual Obscurations (TVOs)
- Pulsatile tinnitus
- Diplopia (CN VI palsy)
- Late: ↓ visual acuity, visual field loss (enlarged blind spot, nasal constriction)
-
Signs:
- Optic disc: blurred margins, elevation, hyperemia
- Venous engorgement, peripapillary hemorrhages, cotton wool spots
- Paton's lines (retinal folds)
- Absence of spontaneous venous pulsation (SVP)
- Late: Optic atrophy, champaign-cork appearance
-
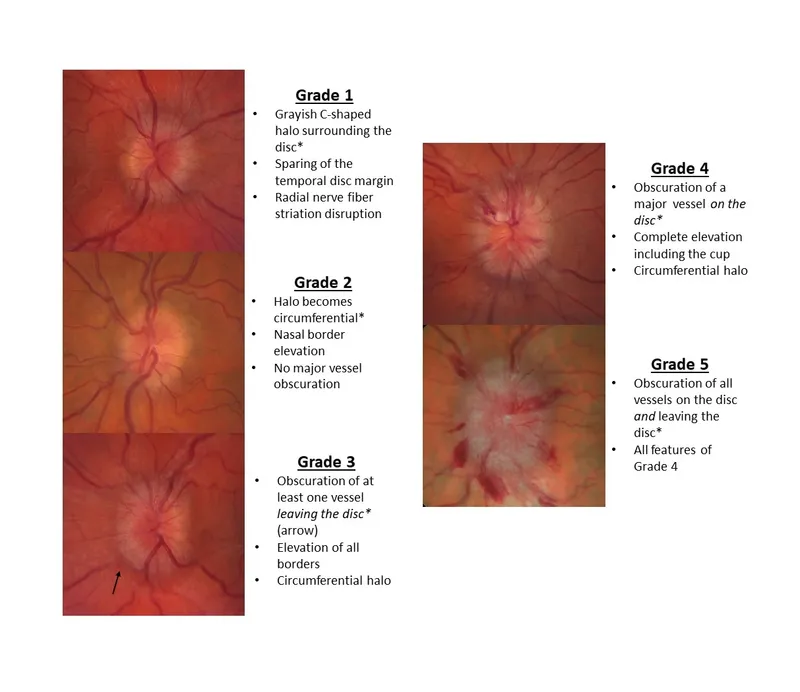
Ophthalmoscopic Stages (Modified Frisen Scale):
- Stage 0: Normal
- Stage 1: Minimal C-shaped halo, blurred nasal border
- Stage 2: Halo obscures vessels
- Stage 3: Obscuration of major vessels
- Stage 4: Total obscuration
- Stage 5: Dome-shaped protrusion
⭐ Transient visual obscurations (TVOs), lasting seconds and often precipitated by postural changes or Valsalva, are a characteristic symptom of papilledema.
Papilledema - Disc Deception Detectives
- Optic disc swelling due to ↑ Intracranial Pressure (ICP); typically bilateral, can be asymmetric.
- Key Signs:
- Blurred disc margins (initially nasal, then circumferential), disc elevation, hyperemia.
- Venous engorgement, peripapillary flame-shaped hemorrhages, cotton wool spots.
- Paton's lines (circumferential retinal folds).
- Enlarged blind spot; later, visual field defects (e.g., arcuate scotoma) & ↓ acuity.
- Symptoms: Headache (worse on waking/straining), nausea, vomiting, transient visual obscurations (TVOs).
- ⚠️ Always rule out intracranial mass lesion (e.g., via CT/MRI) before lumbar puncture.
⭐ Optic disc drusen are a common cause of pseudopapilledema; they may autofluoresce and are best seen with B-scan ultrasonography (showing calcification) or OCT.
Papilledema - Probing & Protecting Vision
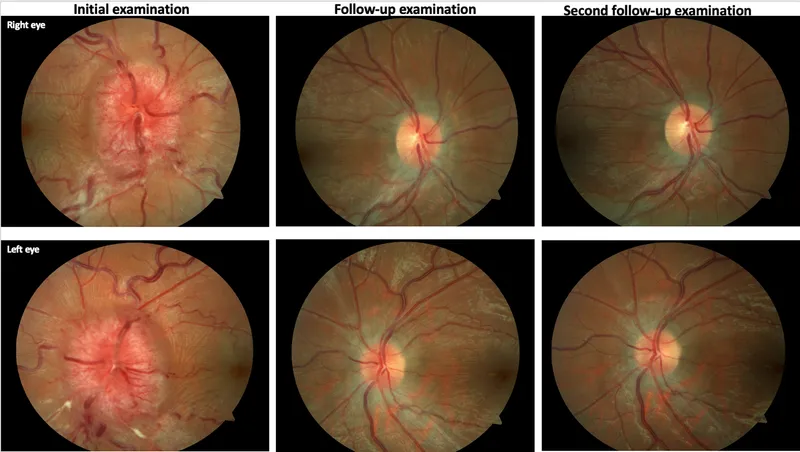
- Definition: Optic disc swelling (bilateral) from ↑ Intracranial Pressure (ICP).
- Causes: Space-Occupying Lesion (SOL), hydrocephalus, Idiopathic Intracranial Hypertension (IIH), meningitis, Cerebral Venous Sinus Thrombosis (CVST).
- Symptoms: Headache, Transient Visual Obscurations (TVOs), pulsatile tinnitus, diplopia (VI N. palsy). Late: ↓Visual Field (VF), ↓Visual Acuity (VA).
- Signs: Hyperemic, edematous disc; blurred margins; venous engorgement; peripapillary hemorrhages; cotton wool spots; Paton's lines. VA often normal initially.
- Workup:
> ⭐ Neuroimaging (MRI of brain and orbits with MRV, or CT if MRI contraindicated) MUST precede lumbar puncture to rule out a mass lesion or structural cause that could lead to herniation.
- LP: Check Opening Pressure (OP >**250** mmH₂O in adults); CSF analysis.
- Management: Treat underlying cause. Medical: Acetazolamide to ↓ICP. Surgical (if vision threatened): Optic Nerve Sheath Fenestration (ONSF), CSF shunting procedures.
High‑Yield Points - ⚡ Biggest Takeaways
- Papilledema: Bilateral optic disc swelling due to ↑ Intracranial Pressure (ICP).
- Visual acuity often preserved early; enlarged blind spot is a key early sign.
- Symptoms of ↑ ICP: headache (worse on waking), nausea/vomiting, transient visual obscurations.
- Absence of pain with eye movements is characteristic.
- Funduscopic signs: blurred disc margins, hyperemia, venous engorgement, hemorrhages.
- Urgent neuroimaging (MRI/CT) is crucial to identify underlying cause.
- Lumbar puncture (after imaging) confirms ↑ opening pressure and can be therapeutic for IIH (Idiopathic Intracranial Hypertension).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more