Nutritional & Toxic Optic Neuropathies - Vision Villains
- 📌 Mnemonic: "TEAM Villains": Tobacco/Alcohol, Ethambutol, Amiodarone, Methanol, Vitamin deficiencies.
| Toxin/Deficiency | Key Features & Visual Field Defect | Management Highlights |
|---|---|---|
| Vit B12/Folate Def. | Painless, progressive bilateral ↓VA; dyschromatopsia. Centrocecal scotoma. | B12/Folate supplementation. |
| Ethambutol | Dose-dependent (>15 mg/kg/day); ↓VA, red-green dyschromatopsia. Centrocecal scotoma. | Discontinue drug; monitor. |
| Methanol | "Snowfield" vision, acidosis, CNS depression. Optic disc hyperemia → atrophy. Centrocecal scotoma. | Fomepizole/Ethanol, supportive, $HCO_3^-$. |
| Amiodarone | Insidious onset, bilateral disc swelling (NAION-like), often mild ↓VA. Various defects. | Discontinue if possible; monitor. |
⭐ Methanol poisoning classically causes optic disc hyperemia initially, followed by optic atrophy, and treatment involves fomepizole or ethanol.
Hereditary Optic Neuropathies - Gene-Sighted Woes
⭐ Leber Hereditary Optic Neuropathy (LHON) is characterized by maternal inheritance due to mitochondrial DNA mutations, typically affecting young males with acute/subacute painless bilateral vision loss.
- Leber Hereditary Optic Neuropathy (LHON)
- 📌 Mnemonic: Lads, Hereditary, Optic Neuropathy, Mothers (Maternal inheritance).
- Inheritance: Maternal (mtDNA mutations, e.g., 11778, 3460, 14484).
- Onset: 15-35 years, acute/subacute painless bilateral vision loss (sequential or simultaneous).
- Clinical: Central/cecocentral scotoma, ↓ color vision. Initially, peripapillary telangiectasia, disc hyperemia; later, optic atrophy.
- Associated: Cardiac arrhythmias (e.g., Wolff-Parkinson-White syndrome), skeletal abnormalities.
- Dominant Optic Atrophy (DOA) - Kjer type
- Inheritance: Autosomal Dominant (OPA1 gene mutation).
- Onset: Insidious, childhood (4-6 years).
- Clinical: Slowly progressive, bilateral, often asymmetric vision loss. Centrocecal scotoma, blue-yellow color defect (tritanopia). Temporal optic disc pallor.
| Feature | LHON | DOA (Kjer type) |
|---|---|---|
| Inheritance | Maternal (mtDNA) | Autosomal Dominant (OPA1) |
| Onset Age | 15-35 yrs (Acute) | 4-6 yrs (Insidious) |
| Vision Loss | Severe, bilateral, painless | Mild-moderate, progressive, bilateral |
| Fundus (Early) | Hyperemia, peripapillary telangiectasia | Normal or temporal pallor |
| Fundus (Late) | Optic atrophy | Optic atrophy (temporal > nasal) |
Compressive & Infiltrative Optic Neuropathies - Pressure Points
- Optic Nerve Glioma:
- Typically children, strong NF1 association.
- Painless proptosis, ↓ vision.
- MRI: Fusiform enlargement of optic nerve.
- Mgmt: Observation, chemotherapy if progressive.
- Optic Nerve Sheath Meningioma (ONSM):
- Primarily middle-aged women.
- MRI: "Tram-track" sign (calcification, enhancement around nerve).
- Mgmt: Observation, radiotherapy, surgery for severe cases.
⭐ Optic nerve sheath meningiomas classically present with the triad of painless progressive vision loss, optic atrophy, and optociliary shunt vessels (though shunt vessels are not always present).
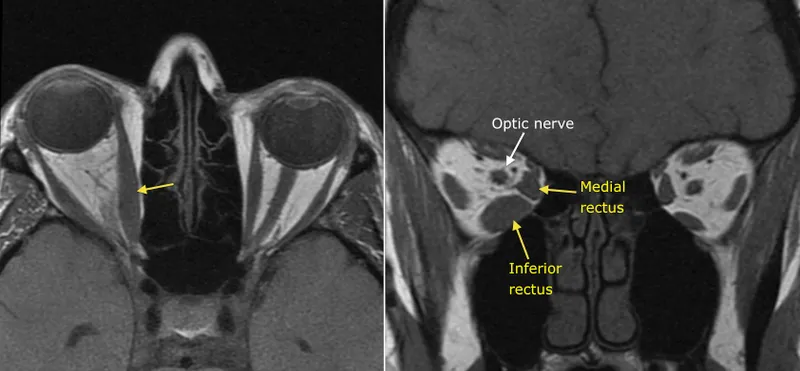
- Thyroid Eye Disease (TED):
- Most common cause of unilateral/bilateral proptosis in adults.
- Diplopia, exposure keratopathy, compressive optic neuropathy.
- CT/MRI: Enlarged extraocular muscles (sparing tendons).
- Mgmt (optic neuropathy): IV methylprednisolone, orbital radiotherapy, surgical decompression.
- Infiltrative Optic Neuropathies (e.g., Sarcoidosis, Lymphoma):
- Sarcoidosis: Optic disc granuloma, uveitis, ↑ACE.
- Lymphoma: Older patients, often bilateral, masquerade syndrome.
- MRI: Optic nerve thickening, enhancement.
- Mgmt: Systemic steroids (sarcoidosis); chemotherapy/radiotherapy (lymphoma).
Traumatic Optic Neuropathy - Impact Insights
-
Classification:
- Direct TON: Penetrating injury, foreign body, direct nerve trauma.
- Indirect TON: More common; blunt head trauma (e.g., frontal impact). Forces transmitted to optic canal.
-
Pathophysiology (Indirect): Shearing forces on nerve fibers, vascular compromise (ischemia), edema within the unyielding optic canal.
-
Clinical Presentation: Acute, often severe, unilateral vision loss; Relative Afferent Pupillary Defect (RAPD) prominent; dyschromatopsia, visual field defects.
-
Immediate Assessment: Visual acuity, pupillary reactions, fundoscopy (may be normal initially), high-resolution CT scan (thin cuts of optic canal for fractures).
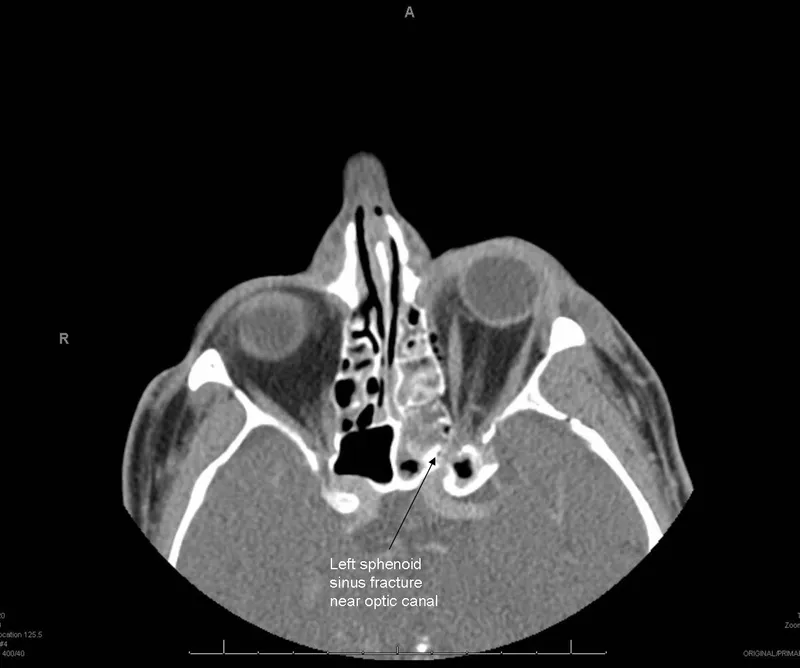
-
Management (Indirect TON): Highly controversial; evidence for any intervention is limited.
-
Options include observation, high-dose corticosteroids, or surgical optic nerve decompression. Decision is individualized.
⭐ The use of high-dose corticosteroids in indirect Traumatic Optic Neuropathy (TON) is controversial and not universally recommended; management decisions are often individualized based on presentation and timing.
High‑Yield Points - ⚡ Biggest Takeaways
- Nutritional/Toxic Optic Neuropathies: Cause bilateral, painless, progressive vision loss with central/cecocentral scotomas.
- Ethambutol toxicity: Dose-dependent, red-green dyschromatopsia.
- Methanol poisoning: Optic disc hyperemia then atrophy; formic acid is toxic.
- LHON: Mitochondrial inheritance, affects young males, acute severe bilateral vision loss.
- DOA: Autosomal dominant (OPA1), childhood onset, temporal pallor, blue-yellow color defect.
- Traumatic Optic Neuropathy: Indirect injury common, acute vision loss post-trauma.
- Amiodarone can cause insidious, bilateral optic neuropathy with prolonged disc swelling.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

