Nystagmus 101 - Decoding Eye Wiggles
- Definition: Involuntary, rhythmic, to-and-fro eye oscillations.
- Types by Waveform:
- Jerk: Slow drift, fast corrective saccade (named by fast phase).
- Pendular: Equal velocity oscillations.
- Planes: Horizontal, vertical, torsional (rotary).

- Characteristics:
- Amplitude: Extent of movement (degrees).
- Frequency: Oscillations per second (Hz).
- Intensity: $Amplitude \times Frequency$.
- Null Point/Zone: Gaze position where nystagmus is minimal/absent. Patients may adopt abnormal head posture.
⭐ Alexander's Law: Jerk nystagmus amplitude ↑ with gaze in the direction of the fast phase.
Nystagmus Types - The Grand Classification
Nystagmus is broadly divided into physiological (normal responses) and pathological (due to disorders).
- Physiological Nystagmus: Benign, induced by stimuli.
- End-point: At extreme lateral gaze; transient.
- Optokinetic: Tracking moving visual fields (e.g., scenery from a train).
- Rotational: During/after head rotation (Vestibulo-Ocular Reflex - VOR).
- Caloric: Thermal stimulation of semicircular canals (VOR test).
- Pathological Nystagmus: Indicates underlying ocular or neurological disease.
- Congenital: Onset at birth or by 3-6 months. Often bilateral, horizontal, pendular. May improve with convergence.
- Acquired: Develops later. Various causes (CNS, vestibular, drugs, toxins). Can be jerk or pendular; type and direction can help localize lesion.
⭐ Congenital nystagmus often has a "null point" or "null zone" where eye movements are minimized, leading patients to adopt an abnormal head posture (AHP) to utilize this zone for improved visual acuity.
Spotlight on Pathological Nystagmus - Key Culprits & Clues
- Peripheral Vestibular Nystagmus:
- Usually horizontal/torsional, unidirectional.
- Suppressed by fixation. Intense vertigo.
- Causes: BPPV (positional), Labyrinthitis/Vestibular Neuronitis (acute, persistent), Meniere's (episodic, auditory symptoms).
- Alexander's Law: Nystagmus ↑ with gaze towards fast phase. 📌 "Alexander looks fast."
- Central Vestibular Nystagmus:
- Often vertical (downbeat, upbeat), torsional, or gaze-evoked (changes direction).
- Not suppressed by fixation. Vertigo mild/absent; neuro signs common.
- Key Types & Localization:
- Downbeat: Craniocervical junction (e.g., Arnold-Chiari).
- Upbeat: Brainstem (pontomedullary), cerebellar vermis.
- Torsional: Medulla, midbrain.
- Gaze-evoked/Rebound: Cerebellar disease.
- See-saw: Parasellar/rostral midbrain.
- PAN (Periodic Alternating Nystagmus): Nodulus/uvula.
- Congenital Nystagmus:
- Bilateral, horizontal, conjugate from birth/early infancy.
- Null point common. ↓ VA, no oscillopsia.
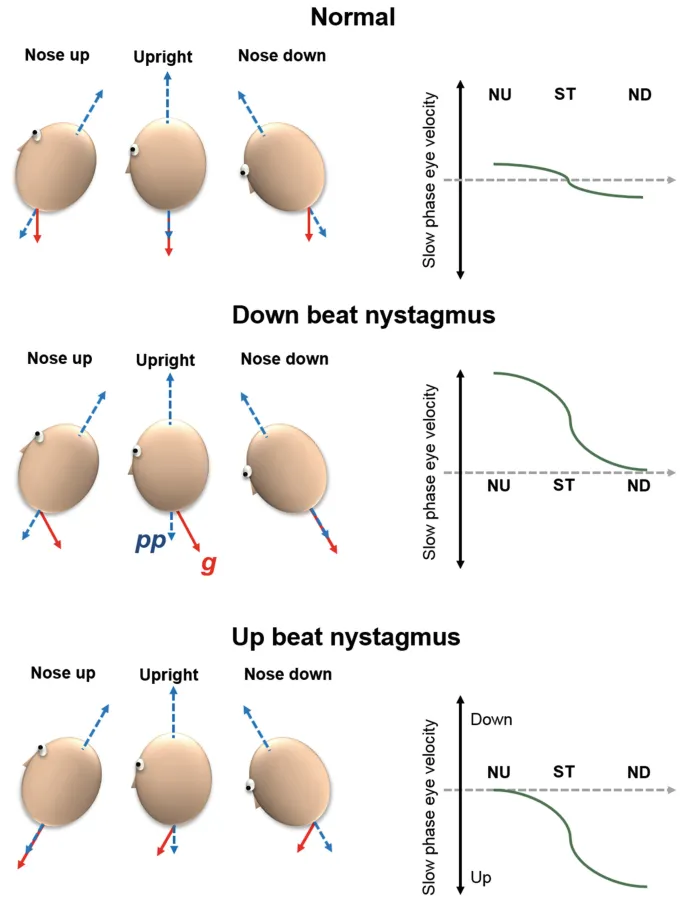
⭐ Downbeat nystagmus often localizes to lesions at the craniocervical junction (e.g., Chiari malformation, cerebellar degeneration).
Central vs. Peripheral Vestibular Nystagmus
| Feature | Peripheral | Central |
|---|---|---|
| Direction | Unidirectional, Horiz-Torsional | Gaze-evoked, Pure Vertical/Torsional |
| Visual Fixation | Suppresses | No suppression / Paradoxical ↑ |
| Vertigo | Severe | Mild / Absent |
| Neurological Signs | Absent (except deafness) | Often present |
| Smooth Pursuit | Normal | Often abnormal |
Clinical Approach - Nystagmus Detective Work
- History: Onset (acute/chronic), oscillopsia, vertigo, triggers (gaze, position), medications (e.g., phenytoin), family Hx.
- Examination:
- Visual Acuity (VA), Dynamic VA (DVA), ocular alignment.
- Nystagmus: Waveform (jerk/pendular), direction (primary & eccentric gaze), effect of fixation.
- Provocative tests: Dix-Hallpike. 📌 HINTS exam (Head Impulse, Nystagmus type, Test of Skew) for central vs. peripheral differentiation.

- Red Flags: New adult onset, associated neurological deficits (e.g., diplopia, ataxia), vertical (downbeat/upbeat) or see-saw nystagmus, HINTS positive for central lesion.
- Key Investigations: Videonystagmography (VNG), MRI Brain (especially if central signs or red flags present).
⭐ Alexander's Law: Jerk nystagmus usually increases in intensity when the eyes are moved in the direction of the fast phase (a key feature of peripheral vestibular nystagmus).
High‑Yield Points - ⚡ Biggest Takeaways
- Nystagmus: Involuntary, rhythmic eye oscillations; differentiate jerk (fast/slow phases) vs. pendular (equal velocity).
- Jerk nystagmus direction: Named by its fast phase; slow phase often localizes pathology.
- Congenital nystagmus: Typically horizontal, improves with convergence, has a null point.
- Acquired nystagmus: Often indicates neurological disease (vestibular, cerebellar, brainstem).
- Downbeat nystagmus: Key sign of craniocervical junction lesions (e.g., Arnold-Chiari).
- Upbeat nystagmus: Suggests brainstem (pontomedullary) lesions; See-saw nystagmus: parasellar lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

