Migraine & Ocular Link - Eye Ache Echoes
- Migraine, a common neurological disorder, frequently manifests with ocular symptoms.
- Visual Aura (most common precursor/accompaniment):
- Scintillating scotomas (flickering blind spots).
- Fortification spectra (teichopsia/zigzag lines).
- Ocular discomfort:
- Photophobia (light sensitivity) is a hallmark.
- Eye ache/pain: often unilateral, retro-orbital, throbbing.
- Pathophysiology: Involves trigeminovascular system activation and cortical spreading depression (CSD).
⭐ Retinal migraine features fully reversible, monocular positive or negative visual phenomena (scintillations, scotoma, or blindness) lasting minutes to <1 hour, differentiating it from typical aura with binocular involvement.
Visual Aura Pathophysiology - Brain's Light Show
- Cortical Spreading Depression (CSD): The primary mechanism.
- Wave of neuronal/glial depolarization.
- Starts in occipital lobe (visual cortex).
- Spreads across cortex at ~3-5 mm/min.
- Followed by prolonged neuronal suppression.
- Neurochemical Events:
- Massive efflux of $K^+$ ions, influx of $Ca^{2+}$.
- Release of glutamate, CGRP, NO.
- Cerebral blood flow: initial brief hyperemia, then sustained oligemia.
- Clinical Correlation:
- CSD in visual cortex → scintillating scotomas, fortification spectra.
- Activates trigeminovascular system → headache.
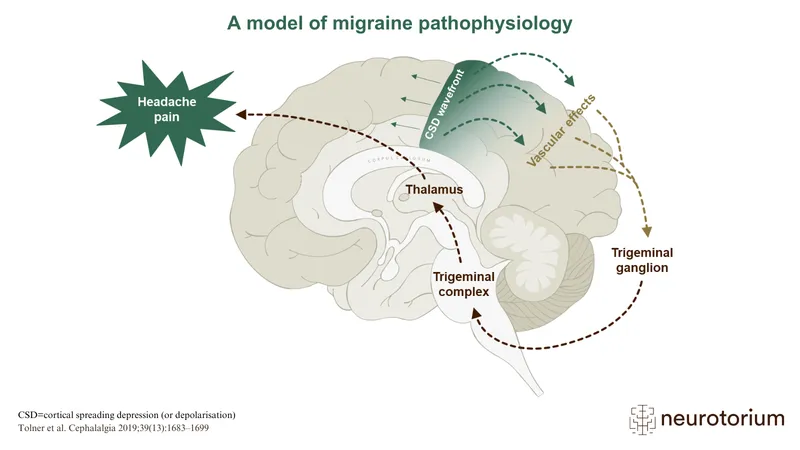
⭐ The slow propagation rate of Cortical Spreading Depression (~3-5 mm/min) across the occipital cortex directly correlates with the gradual build-up and spread of visual aura symptoms.
Key Migraine Eye Syndromes - Vision's Vexing Variants
- Retinal Migraine
- Monocular, reversible visual disturbance (loss, scintillations, scotoma).
- Headache follows/accompanies.
- Diagnosis of exclusion.
- Migraine with Aura (Visual)
- Binocular, homonymous (fortification spectra, scintillating scotoma).
- Develops ≥5 min; lasts 5-60 min.
- Headache usually follows.
- Persistent Visual Aura (PVA)
- Aura >1 week; no infarction.
- Continuous/frequent positive (photopsia) or negative (scotoma) phenomena.
- Recurrent Painful Ophthalmoplegic Neuropathy (RPON)
- (Formerly Ophthalmoplegic Migraine)
- Headache + ipsilateral ocular CN palsy (III most common, IV, VI).
- Childhood onset; MRI essential.
⭐ RPON: CN III palsy can involve pupil, unlike diabetic CN III (pupil-sparing).
- Acephalgic Migraine (Aura without Headache)
- Typical aura (visual, sensory, speech); no headache.
- Commoner in elderly; R/O TIA.
Diagnosis & Mimics - Sorting Sight Signals
- Migraine with Visual Aura:
- IHS Criteria: ≥2 attacks; reversible visual symptoms (scintillating scotoma, photopsia).
- Key features: Gradual spread (≥5 min), duration 5-60 min, headache follows within 60 min.
- Retinal Migraine: Monocular, transient, reversible visual disturbance; headache association.
- Critical Mimics:
- TIA/Stroke: Sudden, negative phenomena, vascular risks.
- Retinal Detachment: Floaters, flashes, curtain.
- Occipital Seizure: Brief, stereotyped, coloured.
- ⚠️ Red Flags: New onset >50 yrs, thunderclap headache, persistent deficit, aura >60 min, papilledema.
⭐ Aura symptoms lasting longer than 60 minutes (persistent aura) or including motor weakness are red flags requiring urgent neuroimaging to exclude stroke.
High‑Yield Points - ⚡ Biggest Takeaways
- Migraine with aura is strongly associated with visual symptoms, often preceding the headache phase.
- Visual auras, like scintillating scotomas or fortification spectra, typically last 5-60 minutes.
- Acephalgic migraine (migraine aura without headache) is a recognized variant.
- Retinal migraine is characterized by monocular visual disturbances, distinct from typical binocular aura.
- Ophthalmoplegic migraine (recurrent painful ophthalmoplegic neuropathy) involves CN palsies; CN III is most common.
- Crucial to differentiate from TIA and other emergent neurological conditions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

