ION Basics - Vision's Vascular Villains
- ION: Optic nerve head (ONH) damage due to ischemia (↓ blood flow).
- Types:
- AAION (Arteritic): Due to Giant Cell Arteritis (GCA). Patients >50 yrs. Urgent!
- NAION (Non-Arteritic): More common. "Optic nerve stroke." Risks: DM, HTN, sleep apnea.
- Pathophysiology: ONH ischemia → axonal swelling → NFL infarct.
⭐ Sudden, painless, and profound vision loss is a hallmark of Ischemic Optic Neuropathy (ION).
AAION (GCA) - Inflamed Artery Attack
- Aka Temporal Arteritis; affects elderly (>50 yrs).
- Systemic vasculitis causing occlusion of short posterior ciliary arteries.
- Symptoms: Sudden, severe, painless vision loss; jaw claudication, headache, scalp tenderness, Polymyalgia Rheumatica (PMR).
- Signs: Chalky-white swollen disc (edema), Afferent Pupillary Defect (APD), often with splinter hemorrhages.
- Diagnosis: Stat ↑ESR (often >50 mm/hr), ↑CRP. Platelets may be ↑.
⭐ Temporal artery biopsy (TAB) showing giant cells and granulomatous inflammation is the gold standard for Giant Cell Arteritis (GCA) diagnosis.
- Treatment: Immediate high-dose IV corticosteroids (e.g., Methylprednisolone 1g/day for 3 days), then oral prednisolone. DO NOT DELAY treatment for biopsy.
- Risk: High risk of bilateral involvement (up to 50% in fellow eye if untreated).

NAION - Ischemia's Silent Strike
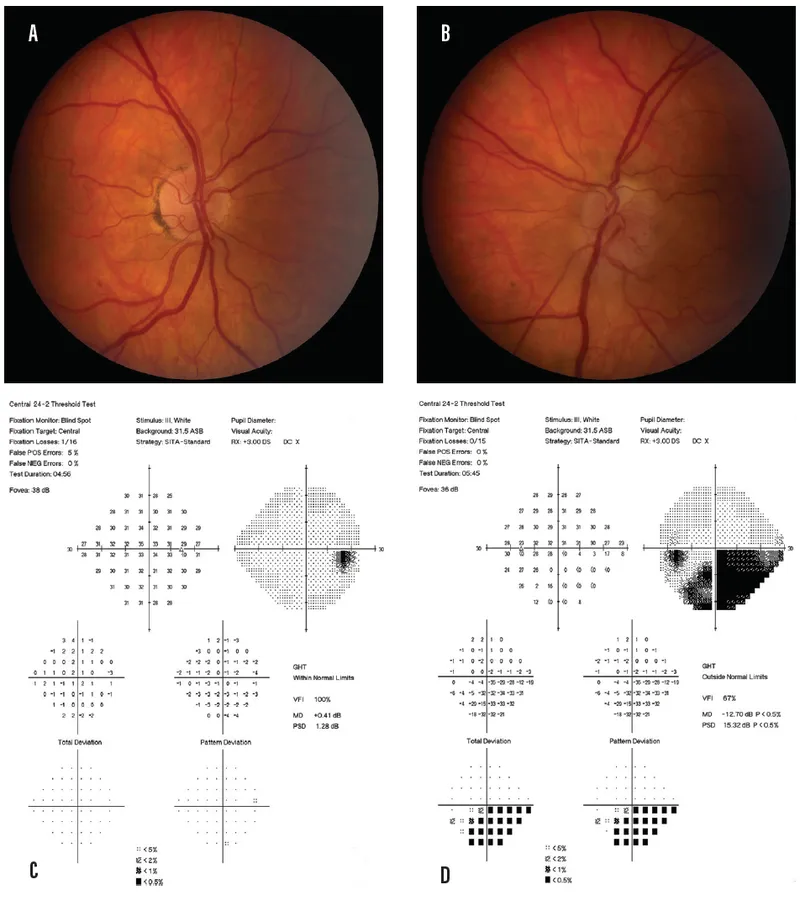
- Pathophysiology: Ischemia of the anterior optic nerve head (ONH) due to transient ↓ perfusion, often via short posterior ciliary arteries.
- Risk Factors: Systemic vascular issues (DM, HTN, HLD, OSA, nocturnal hypotension), phosphodiesterase-5 inhibitors.
- Ocular: Crowded optic disc ('disc at risk').
- Presentation: Sudden, painless, unilateral vision loss, often noticed upon waking.
- Altitudinal (esp. inferior) or arcuate visual field defect.
- Optic disc: Diffuse or sectoral edema (hyperemic or pale), peripapillary hemorrhages.
- Afferent Pupillary Defect (APD) present.
- ESR/CRP: Normal.
⭐ Non-Arteritic AION (NAION) is strongly associated with a 'disc at risk' - a small, crowded optic disc with a small or absent physiologic cup.
ION Workup - Pinpointing the Problem
- History & Exam: Sudden, painless vision loss; relative afferent pupillary defect (RAPD); optic disc swelling (AION) or pallor (PION, late AION).
- Key Investigations:
- ESR, CRP: Crucial for suspected Giant Cell Arteritis (GCA-AION); target ESR > 50 mm/hr.
- Temporal artery biopsy if GCA suspected.
- Visual Fields: Altitudinal defects (inferior > superior) are characteristic.
- **Fluorescein Angiography (FA):
- AION: Delayed choroidal filling, optic disc hyperfluorescence/leakage.
- NAION: Sectoral disc hypoperfusion, late leakage.
- Differentiating from Optic Neuritis (ON):
- ON: Pain with eye movements, typically younger, good steroid response, often retrobulbar initially.
⭐ An altitudinal visual field defect, especially inferiorly, is highly characteristic of Ischemic Optic Neuropathy.
ION Treatment - Vision Rescue Plan
- AAION (Arteritic Anterior Ischemic Optic Neuropathy):
- Immediate high-dose systemic corticosteroids (IV methylprednisolone 1g/day for 3 days, then oral prednisolone).
- Temporal artery biopsy for confirmation.
- Aspirin may be added.
- Prognosis: Vision recovery variable; fellow eye risk ↓ with steroids.
- NAION (Non-Arteritic Anterior Ischemic Optic Neuropathy):
- No proven acute treatment; manage vascular risk factors (HTN, DM, cholesterol).
- Aspirin may be considered.
- Prognosis: Some spontaneous vision improvement in ~40%; fellow eye involvement ~15-20% in 5 years.
⭐ For AAION, immediate administration of high-dose systemic corticosteroids is crucial to prevent further vision loss in the affected eye and involvement of the fellow eye.
High‑Yield Points - ⚡ Biggest Takeaways
- AION is more common; AAION, often due to Giant Cell Arteritis (GCA), requires urgent high-dose steroids.
- NAION is associated with vascular risk factors (e.g., diabetes, hypertension, sleep apnea).
- Characteristic symptom: sudden, painless, monocular vision loss.
- Optic disc swelling (diffuse or sectoral, often pallid) is seen in AION; initially normal disc in PION.
- An Afferent Pupillary Defect (APD) is typically present in unilateral or asymmetric cases.
- Elevated ESR and CRP are critical for suspected GCA in AAION; temporal artery biopsy confirms.
- Management: Steroids for AAION; manage risk factors for NAION; no proven treatment for NAION itself.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

