CN III Palsy - The Droopy Director
- Causes:
- Microvascular (DM, HTN): Pupil often spared.
- Compressive (PCOM aneurysm, tumor): Pupil often involved. ⚠️
- Trauma.
- Signs:
- Ptosis (droopy eyelid).
- Eye "down and out".
- Mydriasis (dilated pupil; if parasympathetic fibers hit).
- Diplopia.
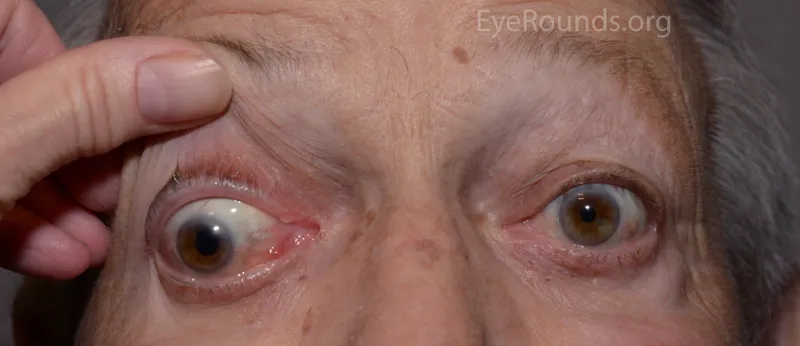
- Pupil:
- Sparing: Ischemia likely.
- Involved: Urgent imaging (aneurysm?).
⭐ A pupil-involving CN III palsy suggests a compressive lesion like a PCOM aneurysm.
CN IV Palsy - The Tilted Viewer
- Etiology: Trauma (most common), congenital, vascular (DM, HTN), tumor, idiopathic.
- Clinical Features:
- Vertical/torsional diplopia: worse on downgaze & contralateral gaze (e.g., reading, descending stairs).
- Compensatory head tilt to the shoulder opposite the lesion.
- Examination:
- Parks-Bielschowsky 3-step test to isolate paretic Superior Oblique (SO).
- Affected eye shows hypertropia, worsening on adduction & ipsilateral head tilt.
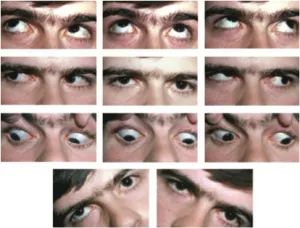
⭐ Patients characteristically tilt their head AWAY from the side of the lesion (towards the contralateral shoulder) to minimize diplopia_._
CN VI Palsy - The Sideways Straggler
- Nerve: Abducens (CN VI). Muscle: Lateral Rectus (LR). Action: Abduction (outward eye movement).
- Symptoms:
- Horizontal, uncrossed diplopia; worse on ipsilateral gaze & for distance.
- Esotropia (eye turns inward), more pronounced on attempted abduction.
- Compensatory head turn towards the side of palsy to maintain binocular vision.
- Common Causes:
- Microvascular (diabetes, hypertension) in older adults (>50 yrs).
- Trauma.
- ↑ Intracranial Pressure (ICP).
- Tumors (e.g., pontine glioma, nasopharyngeal carcinoma), inflammation.
⭐ Sixth nerve palsy can be a "false localizing sign," indicating raised intracranial pressure (ICP) due to its long, vulnerable intracranial course over the petrous apex, rather than a direct lesion of the nerve nucleus or fascicle at that specific ICP-related site of injury (e.g., Dorello's canal).
Combined Palsies - The Cranial Crowd
- Multiple CN palsies localize lesion.
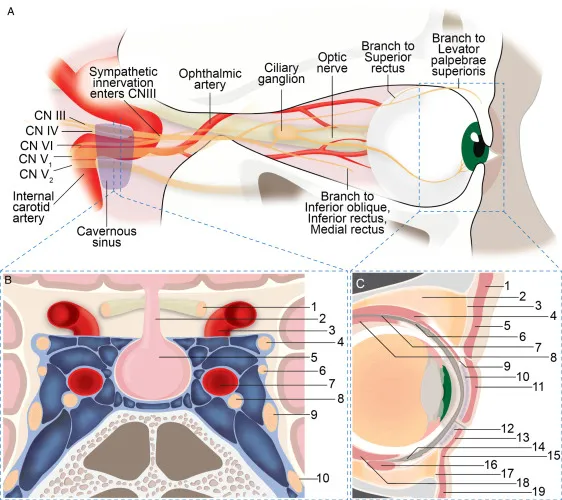
- Cavernous Sinus Syndrome:
- III, IV, V1, V2, VI, sympathetics.
- Proptosis, ophthalmoplegia, facial sensory loss (V1/V2).
- Causes: Tumor, fistula, inflammation.
- Superior Orbital Fissure (SOF) Syndrome:
- III, IV, V1, VI. (V2 spared vs. Cavernous Sinus)
- Orbital Apex Syndrome:
- SOF nerves + II (optic neuropathy → ↓vision).
- E.g., Tolosa-Hunt (painful ophthalmoplegia, steroid-responsive).
- Gradenigo's Syndrome:
- VI palsy, V pain (V1/V2), petrous apicitis.
- VI palsy, V pain (V1/V2), petrous apicitis.
⭐ Tolosa-Hunt syndrome: painful ophthalmoplegia from granulomatous inflammation (cavernous sinus/SOF), responds to steroids.
Cranial Nerve Palsy Workup - The Neuro-Op Toolkit
- History: Onset (sudden/gradual), progression, trauma, pain, diplopia, ptosis, associated neurological/systemic symptoms.
- Examination:
- Visual Acuity, Visual Fields, Pupils (RAPD, size, reactivity).
- Ocular Motility (versions, ductions), Cover tests, Lid position.
- Fundoscopy (optic disc), Exophthalmometry.
- Complete neurological & relevant systemic exam.
- Investigations (Clinical-Guided):
- Bloods: CBC, ESR/CRP, Glucose/HbA1c, TFTs, AChR-Ab.
- Imaging: MRI (brain/orbits) ± MRA/MRV; CT (trauma).
- LP (infection/inflammation).
- Tensilon/Ice pack test (Myasthenia).
⭐ In an isolated CN III palsy, pupillary involvement (mydriasis) is a red flag for a compressive lesion (e.g., PCOM aneurysm) until proven otherwise; pupillary sparing often points to microvascular ischemia (e.g., diabetes, hypertension).
High‑Yield Points - ⚡ Biggest Takeaways
- CN III palsy: Ptosis, mydriasis, "down and out" eye. Pupil involved = compressive (aneurysm); pupil spared = ischemic.
- CN IV palsy: Vertical diplopia, worse on contralateral gaze & ipsilateral head tilt. Head tilt away from lesion.
- CN VI palsy: Horizontal diplopia, worse on ipsilateral gaze (abduction failure). Vulnerable to ↑ICP.
- Painful ophthalmoplegia: Suspect PCOM aneurysm, Tolosa-Hunt, or GCA.
- Aberrant regeneration CN III: Lid-gaze dyskinesis after compressive injury, not ischemic.
- Multiple palsies: Think cavernous sinus, orbital apex, or brainstem.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

