Definitions & Goals - Seeing the Challenge
- Low Vision (as per NPCB, India):
- Visual Acuity (VA): >3/60 up to 6/18 (better eye, best correction).
- Visual Field (VF): <40° to >10° around central fixation.
- Blindness (as per NPCB, India):
- VA: ≤3/60 (better eye, best correction).
- VF: ≤10° around central fixation.
- Goals of LVA & Rehabilitation:
- Maximize use of residual vision.
- Enhance functional ability, independence.
- Improve Quality of Life (QoL).
⭐ For NEET PG, remember NPCB (India) criteria: Blindness includes VA ≤3/60 or VF ≤10°.
Patient History - Uncovering Needs
- Goal: Uncover patient's specific needs, functional limitations, and clear rehabilitation goals.
- Key Areas (📌 Mnemonic: FOCUS):
- Functional Impact: ADL/IADL difficulties (e.g., reading, mobility, self-care), work, hobbies.
- Ocular Details: Diagnosis, onset, duration, progression of vision loss; key symptoms (blur, scotoma, glare); LVAs used & effectiveness.
- Chief Complaint & Goals: Patient's primary concerns; specific, desired activities post-rehab.
- Understanding & Expectations: Patient's knowledge of their condition; psychosocial impact; realistic rehab goals.
- Systemic Health & Social Context: Relevant co-morbidities (DM, HTN); medications; social support, living situation, occupation.
⭐ Eliciting patient-specific, realistic goals is crucial for tailoring rehabilitation and ensuring patient motivation and satisfaction.
Visual Function Tests I - Quantifying Sight
- Visual Acuity (VA): Measures detail. Distances: 6m (Snellen), 4m (ETDRS).
- LogMAR: For low vision. $LogMAR = Log_{10}(MAR)$. 1.0 = 6/60.
| Feature | Snellen Chart | ETDRS/LogMAR Chart |
|---|---|---|
| Letters/Line | Variable | 5 (Sloan optotypes) |
| Size Progression | Irregular | Logarithmic (0.1 LogMAR steps) |
| Scoring | Line-based (e.g., 6/60) | Letter-by-letter (LogMAR score) |
| Distance | 6m | 4m, 2m, 1m (adaptable) |
| Low Vision Use | Less accurate | Gold standard |
⭐ LogMAR Advantage: ETDRS charts: superior accuracy in low vision via uniform letters, consistent spacing, log progression; crucial for monitoring.
- Beyond Charts: Counting Fingers (CF), Hand Movements (HM), Light Perception (LP).
Visual Function Tests II - Beyond Acuity
- Visual Field Assessment:
- Confrontation Test: Gross peripheral field screening.
- Amsler Grid: Central 10-20° (macula); detects scotomas, metamorphopsia.
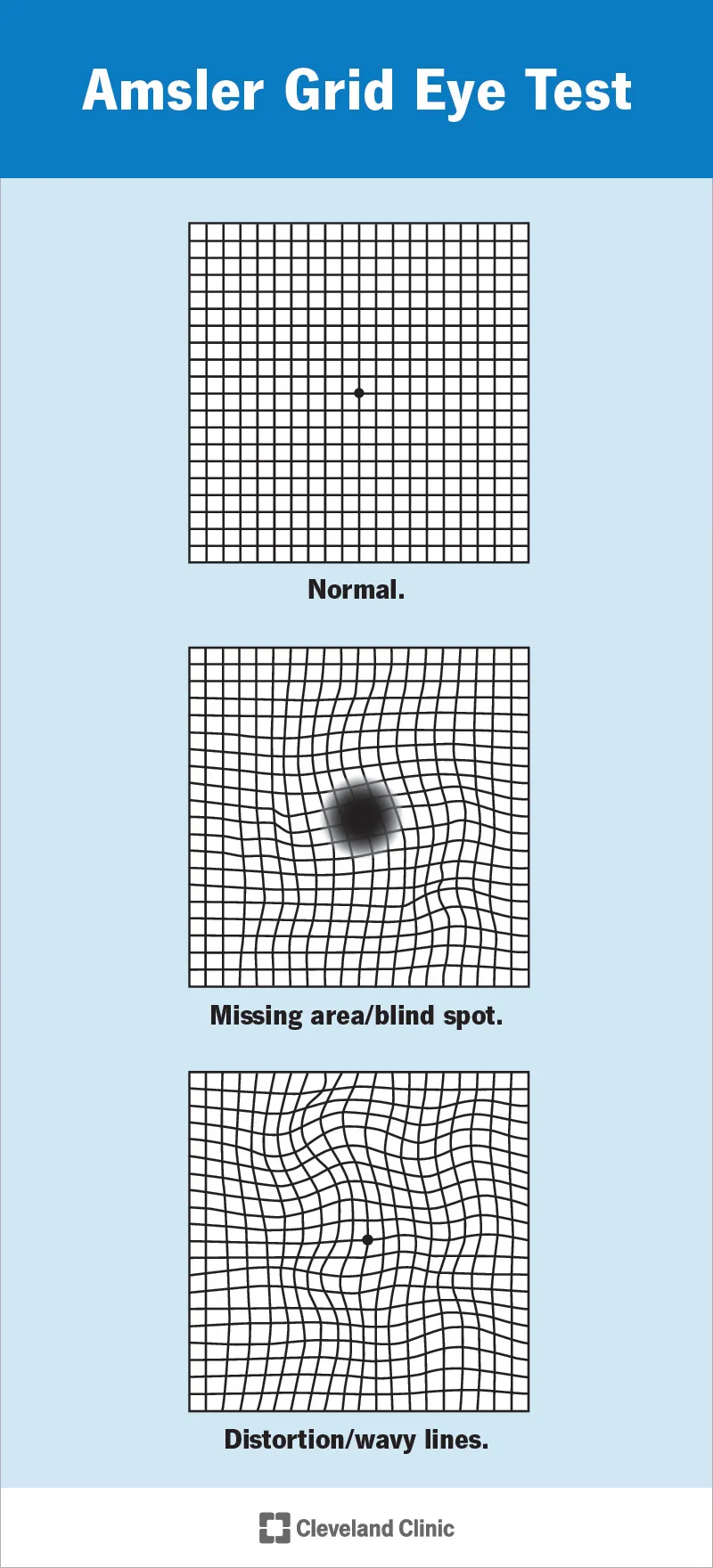
- Perimetry (Humphrey, Goldmann): Detailed mapping for glaucoma, neuro-lesions, and monitoring progression.
- Contrast Sensitivity:
- Pelli-Robson, Mars charts: Quantifies ability to discern subtle shade differences.
- Reduced in cataract, glaucoma, diabetic retinopathy; impacts daily tasks like night driving, reading, recognizing faces.
- Color Vision:
- Ishihara Plates: Rapid screening for congenital red-green deficiencies.
- Farnsworth D-15: Arranges colored caps; classifies defect type/severity (e.g., protan, deutan, tritan).
- Glare Testing & Disability Glare:
- Brightness Acuity Tester (BAT): Measures acuity reduction under glare conditions (e.g., posterior subcapsular cataracts).
- Dark Adaptation:
- Evaluates rod function; prolonged in retinitis pigmentosa, Vitamin A deficiency, or other photoreceptor dystrophies.
⭐ The Amsler grid is a simple, effective tool for patients to self-monitor central visual field changes at home, crucial for early detection or monitoring progression of macular diseases like Age-related Macular Degeneration (AMD).
High-Yield Points - ⚡ Biggest Takeaways
- Low Vision: BCVA <6/18 to >3/60 or visual field <20° (better eye).
- Assessment: History, VA (distance/near), contrast, fields, refraction, functional vision.
- Distance VA: LogMAR charts (ETDRS, Bailey-Lovie) preferred over Snellen.
- Near Vision: Assessed with MNREAD charts for acuity and reading speed.
- Functional Vision: Evaluated using questionnaires (VFQ-25) and observation of ADLs.
- Contrast Sensitivity: Tested with Pelli-Robson or Mars charts; vital for mobility.
- Goal Setting: Patient-centered goals are paramount for successful rehabilitation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

