Visual Field Testing in Glaucoma - VFT Basics: Unveiling Loss
- Visual Field (VF): Area visible to one eye with fixed gaze; "Hill of Vision" concept.
- Glaucoma causes progressive, irreversible VF loss due to optic nerve damage.
- VFT detects defects early, often before symptoms, and monitors progression.
- Sensitivity measured in decibels (dB); higher dB = better light sensitivity. Normal peak ~35 dB.
- Defects: Nasal step, paracentral scotoma, arcuate (Bjerrum's) scotoma.
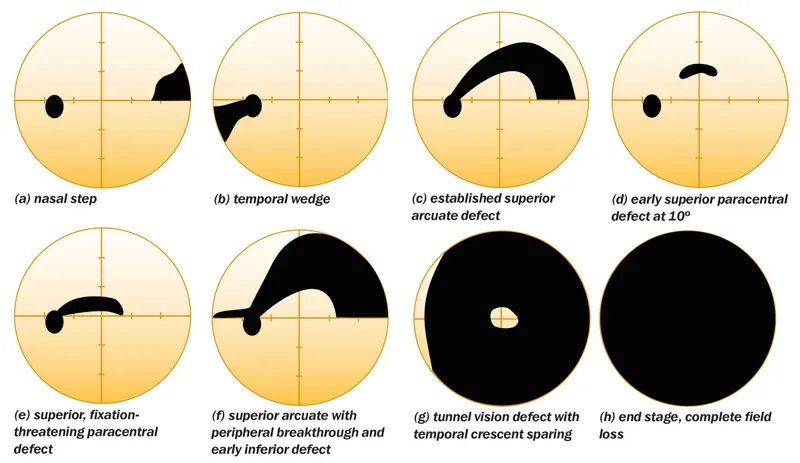
⭐ Bjerrum's (arcuate) scotoma, arching from blind spot, is a hallmark of early glaucoma.
Visual Field Testing in Glaucoma - Perimetry Types: Test Tactics
- Standard Automated Perimetry (SAP): Gold standard (e.g., Humphrey, Octopus).
- Stimulus: White, Size III. Background: White.
- Test Strategies:
- Threshold: SITA (Standard, Fast, Faster) - common, efficient. Full Threshold - longest, most data.
- Suprathreshold: Rapid screening; less detail.
- Frequency Doubling Technology (FDT): Targets magnocellular (M-cell) pathway; rapid screening.
- Short Wavelength Automated Perimetry (SWAP): Blue stimulus (Size V) on yellow background; detects early blue-yellow defects. Higher variability.
- Reliability Indices (SAP):
- Fixation Losses: < 20%
- False Positives: < 15%
- False Negatives: < 15%
⭐ SITA strategies significantly reduce test duration compared to Full Threshold, enhancing patient cooperation and test reliability.
Visual Field Testing in Glaucoma - Defect Patterns: Glaucoma's Footprints
- Early Defects (Reflect RNFL Damage):
- Paracentral scotoma: In Bjerrum's area (10-20° from fixation).
- Nasal step (Rønne's): Respects horizontal meridian.
- Seidel's scotoma: Sickle-shaped extension from blind spot.
- Temporal wedge defect: Less common.
- Progressive Defects:
- Arcuate scotoma (Bjerrum scotoma): Arch-shaped, from blind spot to nasal field; coalescence of smaller scotomas.
- Ring scotoma (Double arcuate): Encircles fixation.
- Advanced Defects:
- Central and/or temporal island of vision.
- End Stage:
- Minimal remaining vision or No Light Perception (NLP).
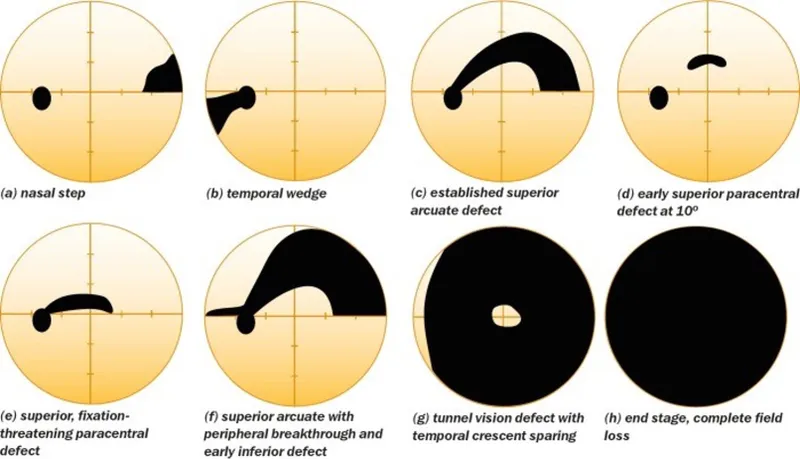
⭐ The nasal step is a classic early glaucomatous defect, often appearing before significant changes in visual acuity.
Visual Field Testing in Glaucoma - Report Analysis: Decoding Dots
- Reliability Check (Key for valid interpretation):
- Fixation Losses (FL): < 20%
- False Positives (FP): < 15%
- False Negatives (FN): < 15%
- Interpreting Dots & Global Indices:
- Dots: Represent retinal sensitivity in decibels (dB). Lower dB = ↓ sensitivity.
- Mean Deviation (MD): Overall field depression. More negative = worse. ↓ in glaucoma.
- Pattern Standard Deviation (PSD): Localized loss. ↑ in glaucoma.
- Visual Field Index (VFI): 0-100%; estimates percentage of remaining vision.
- Key Plots: Grayscale, Total Deviation, Pattern Deviation (highlights focal defects), Glaucoma Hemifield Test (GHT) (compares hemifields).
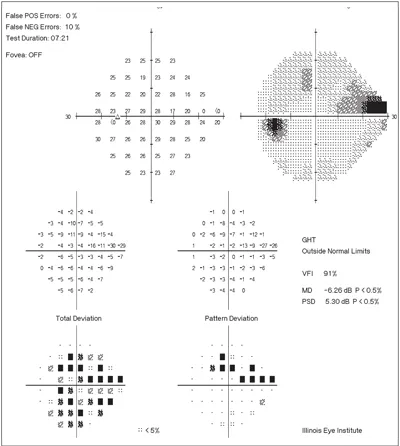
⭐ Visual Field Index (VFI) is a key staging parameter, expressed as a percentage (0-100%), and correlates well with retinal ganglion cell (RGC) count, reflecting structural damage an_function_call_response
High‑Yield Points - ⚡ Biggest Takeaways
- SAP (Standard Automated Perimetry) is the gold standard for assessing glaucomatous field loss.
- Early defects: Paracentral scotoma, nasal step (Rønne's), Bjerrum's scotoma (arcuate).
- Seidel's scotoma: Sickle-shaped extension of the blind spot, an early sign.
- Progression patterns: Arcuate scotoma can enlarge to a ring scotoma or nasal breakthrough.
- Advanced loss: Only a central island and temporal island of vision remain.
- Key HFA indices: VFI (Visual Field Index) for staging/progression, GHT (Glaucoma Hemifield Test) for classification of results based on normative data.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

