Secondary Angle-Closure Glaucomas - Angle Antagonists
- Definition: Trabecular meshwork (TM) obstruction; angle directly compromised by identifiable factors.
- Mechanisms:
- Anterior Pulling (Membranes):
- Neovascular Glaucoma (NVG): Fibrovascular membrane (FVM) contracts, zippering angle. Causes: PDR, CRVO, OIS.
- ICE Syndromes: Corneal endothelium membrane over angle.
- Peripheral Anterior Synechiae (PAS): Chronic uveitis, post-op.
- Posterior Pushing (Direct Obstruction):
- Ciliary Body Swelling/Rotation: Topiramate, uveal effusion.
- Phacomorphic Glaucoma: Large lens crowds angle.
- Tumors/Cysts: Iris/ciliary body masses obstruct.
- Anterior Pulling (Membranes):
⭐ NVG: Rubeosis iridis precedes angle neovascularization. 90-day glaucoma classic post-CRVO.
Secondary Angle-Closure Glaucomas - Behind The Scenes Push
- Posterior segment pathology or lens changes displace iris-lens diaphragm anteriorly, narrowing/closing the angle.
- Key Mechanisms & Causes (Posterior Push):
- Lens-induced (Phacomorphic):
- Intumescent cataract (swollen lens).
- Subluxated/dislocated lens.
- Ciliary Body Swelling/Anterior Rotation:
- Uveitis (e.g., Vogt-Koyanagi-Harada, posterior scleritis).
- Drugs (e.g., topiramate, sulfonamides 📌 SulfaTop).
- Choroidal effusion/hemorrhage.
- Tumors (ciliary body/choroidal).
- Aqueous Misdirection (Malignant Glaucoma):
- Posterior aqueous diversion; often post-op.
- Post-Retinal Surgery:
- Scleral buckle, intravitreal gas/oil.
- Nanophthalmos: Anatomical predisposition.
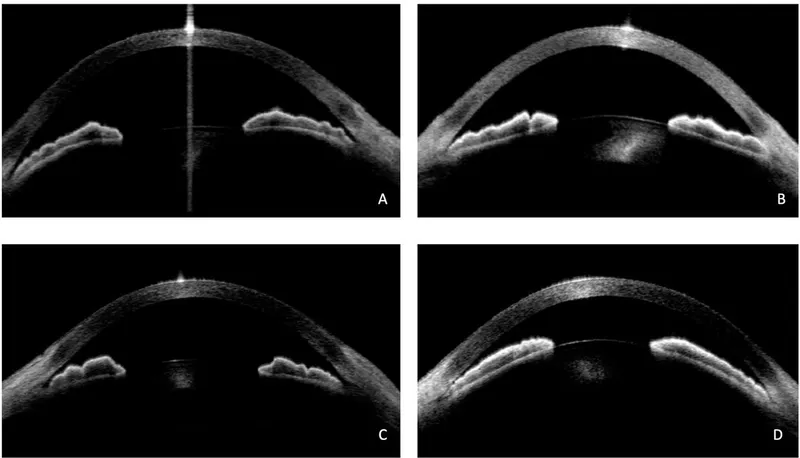
- Lens-induced (Phacomorphic):
⭐ Aqueous misdirection classically presents with a uniformly shallow anterior chamber and high IOP, often post-trabeculectomy.
Secondary Angle-Closure Glaucomas - Frontal Assault & Blockade
- Anterior Pulling (No Pupillary Block): Iris pulled into TM, closing angle.
- Neovascular Glaucoma (NVG): Membrane contraction (rubeosis iridis).
- ICE Syndrome: Endothelial membrane contracts iris.
- Epithelial/Fibrous downgrowth: Post-trauma/surgery.
- PAS: Post-inflammation/trauma.
- Pupillary Block: Aqueous flow obstructed at pupil.
- Phacomorphic: Swollen lens (intumescent cataract).
- Ectopia Lentis: Subluxated/dislocated lens.
- Aphakic/Pseudophakic block: Vitreous/IOL.
- Seclusio Pupillae: 360° posterior synechiae (uveitis).
- Silicone oil.

⭐ NVG: rubeosis iridis & angle neovessels are key; linked to retinal ischemia (PDR, CRVO).
Secondary Angle-Closure Glaucomas - Spotting The Closure
- Clinical Clues:
- Symptoms: Acute pain, blurred vision, halos, N/V (if IOP ↑↑).
- Signs: Corneal edema, shallow AC, mid-dilated pupil, ↑IOP.
- Diagnostic Steps:
- Gonioscopy: Essential to see Peripheral Anterior Synechiae (PAS) & angle status.
- Indentation gonioscopy: Differentiates appositional vs. synechial closure.
- Ultrasound Biomicroscopy (UBM): Visualizes angle structures if cornea hazy; ciliary body assessment.
- Slit-lamp exam: Detailed anterior segment evaluation.
- Gonioscopy: Essential to see Peripheral Anterior Synechiae (PAS) & angle status.
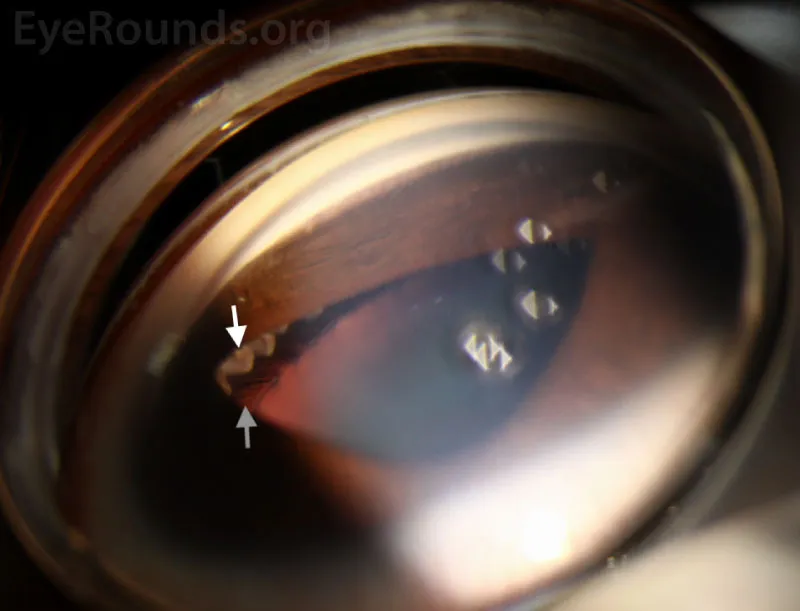
⭐ Gonioscopy is indispensable for diagnosing angle closure, revealing Peripheral Anterior Synechiae (PAS) which confirm synechial closure.
Secondary Angle-Closure Glaucomas - Unblocking The Path
- Causes: Uveitis, neovascular (NVG), lens-induced (phacomorphic, phacolytic), trauma, tumors, drugs (e.g., topiramate).
- Mechanisms:
- Anterior pulling (e.g., peripheral anterior synechiae (PAS), membranes).
- Posterior pushing (e.g., swollen lens, ciliary body edema/rotation).
- Treatment Focus:
- Crucially, treat the primary underlying pathology first.
- Aggressively ↓IOP: Medical (aqueous suppressants; ⚠️ avoid miotics in pupillary block/phacomorphic), Laser (LPI if pupillary block present), Surgery (filtration, GDDs).
⭐ Neovascular glaucoma (NVG), often due to Proliferative Diabetic Retinopathy (PDR) or Central Retinal Vein Occlusion (CRVO), is a common, aggressive SACG.
High‑Yield Points - ⚡ Biggest Takeaways
- Neovascular glaucoma (NVG): severe SACG, often from PDR/CRVO.
- Uveitic glaucoma: inflammation causes synechiae (PAS/PS) or pupillary block.
- Lens-induced: Phacomorphic (swollen lens), phacolytic (leaking proteins), lens subluxation/dislocation.
- Aqueous misdirection (malignant glaucoma): posterior aqueous diversion, shallow AC.
- ICE syndromes: progressive angle closure by abnormal corneal endothelium.
- Epithelial/Fibrous downgrowth: post-surgery/trauma, obstructs angle.
- Management: Treat underlying cause and aggressively lower IOP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

