PACG Basics - Eye Under Pressure
Error generating content for this concept group: No object generated: the tool was not called.
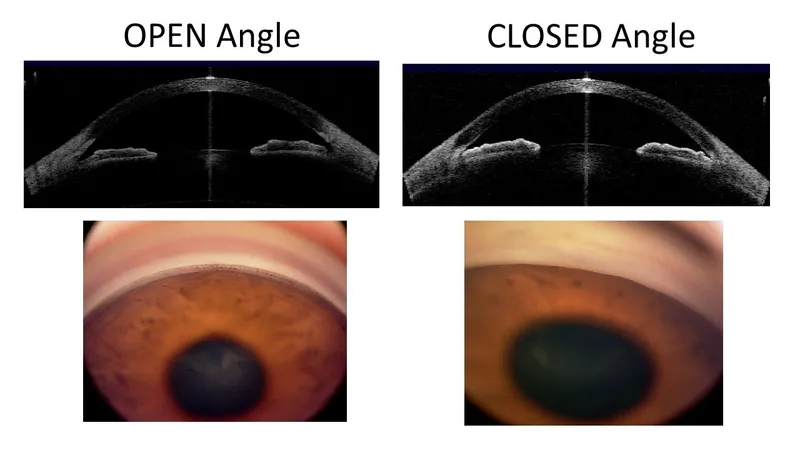
Mechanisms & Stages - The Closure Story
- Mechanisms:
- Pupillary Block (>90%): Relative (lens-iris apposition) or absolute (posterior synechiae) → iris bombé → iridotrabecular contact (ITC).
- Plateau Iris: Anterior ciliary processes push peripheral iris into angle. "Double hump sign".
- Lens-induced: Phacomorphic, subluxation.
- Malignant Glaucoma: Posterior aqueous misdirection.
- Stages (ISGEO Classification):
- PACS: ≥180° ITC; normal IOP, no PAS, no optic disc damage.
- PAC: PACS criteria + (PAS or ↑IOP); no glaucomatous optic neuropathy (GON).
⭐ Pupillary block is the predominant mechanism in over 90% of Primary Angle Closure cases.
- PACG: PAC criteria + GON.
- Acute Angle Closure Crisis (AACG): Sudden, severe IOP ↑; pain, blurred vision (corneal edema), halos, nausea.
Symptoms & Signs - Spotting the Attack
- Acute Angle-Closure Crisis (Ophthalmic Emergency):
- Symptoms:
- Sudden, severe unilateral ocular pain, may radiate.
- Blurred vision ("steamy"), halos around lights.
- Nausea, vomiting (oculocardiac reflex).
- Headache, photophobia.
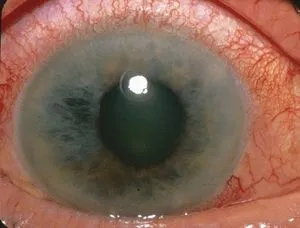
- Signs:
- IOP markedly ↑ (often > 40-50 mmHg).
- Ciliary flush (circumcorneal injection).
- Corneal edema (hazy cornea).
- Shallow anterior chamber (AC).
- Pupil: mid-dilated, fixed or sluggishly reactive, often vertically oval.
- Gonioscopy: Confirms closed angle (e.g., Shaffer Grade 0).
- Symptoms:
- Intermittent (Subacute) Angle Closure:
- Transient blurred vision, halos (e.g., in dim light, movies).
- Mild eye ache or frontal headache.
- Symptoms resolve spontaneously (e.g., sleep, bright light).
⭐ The classic triad of acute angle-closure crisis includes severe ocular pain, blurred vision with halos around lights, and nausea/vomiting.
Diagnosis & Management - Opening the Gates
-
Diagnosis:
- Gonioscopy: Gold standard (ITC, PAS).
- UBM/AS-OCT: Angle/ciliary body imaging.
-
Management Goal: ↓IOP, open angle, prevent ON damage.
-
Acute Attack:
- Medical:
- Topical: Timolol 0.5%, Apraclonidine 1%, Pilocarpine 2% (post-IOP drop).
- Systemic: Acetazolamide 500mg, Mannitol 1-2 g/kg IV.
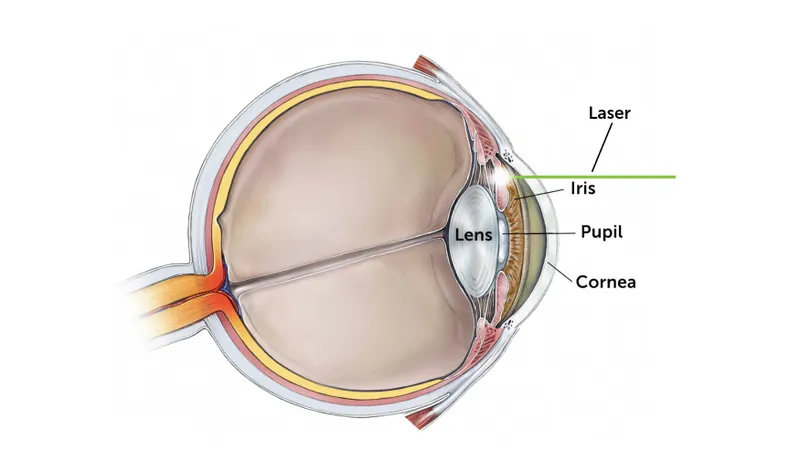
- Laser:
⭐ Laser Peripheral Iridotomy (LPI) is the definitive first-line treatment for eyes with pupillary block mechanism in PAC Suspect, PAC, and PACG.
- Acute Management Steps:
- Medical:
-
Chronic/Post-LPI:
- Topical IOP-lowering meds.
- ALPI (plateau iris).
- Lens extraction/Trabeculectomy (if needed).
High‑Yield Points - ⚡ Biggest Takeaways
- Pupillary block is the most common mechanism in PACG.
- Risk factors: hypermetropia, female, older age, Asian ethnicity.
- Acute attack: sudden painful red eye, halos, nausea, mid-dilated fixed pupil, ↑↑IOP.
- Gonioscopy confirms occludable angles, essential for diagnosis.
- Acute treatment: Medical (IV mannitol, acetazolamide, pilocarpine) then Laser Peripheral Iridotomy (LPI).
- LPI is the definitive treatment for pupillary block PACG.
- Chronic PACG is often asymptomatic with progressive optic nerve damage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

