Laser Principles & Types - Beam Me Up!
- Core Principle: Selective absorption of laser energy by target tissue.
- Photocoagulation: Thermal effect (e.g., Argon laser for ALT, Diode for cyclophotocoagulation).
- Photodisruption: Optical breakdown (e.g., Nd:YAG for iridotomy, capsulotomy).
- Selective Photothermolysis: Targets pigmented cells with minimal collateral damage (e.g., SLT).
- Common Lasers in Glaucoma:
- Argon Laser (thermal)
- Nd:YAG Laser (photodisruptive)
- Selective Laser Trabeculoplasty (SLT) Laser (selective photothermolysis)
- Diode Laser (thermal, transscleral cyclophotocoagulation - TCPC)
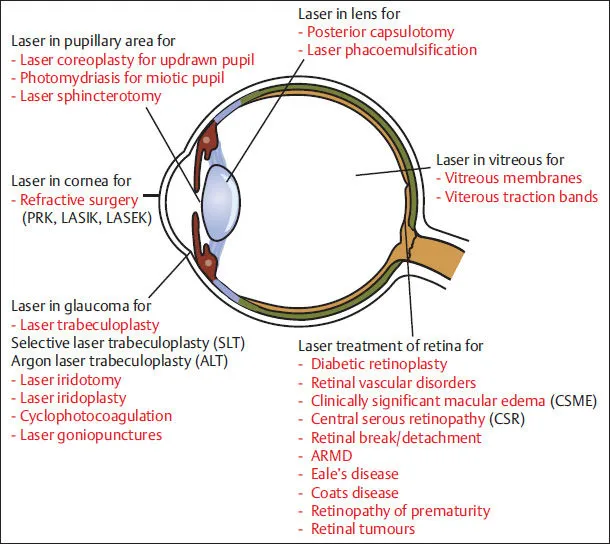
⭐ Nd:YAG laser creates a shockwave and plasma formation for tissue disruption, crucial for peripheral iridotomy in angle-closure glaucoma to create an alternative aqueous outflow pathway. Its wavelength is typically 1064 nm (infrared).
Laser Trabeculoplasty - Drain Game Changer
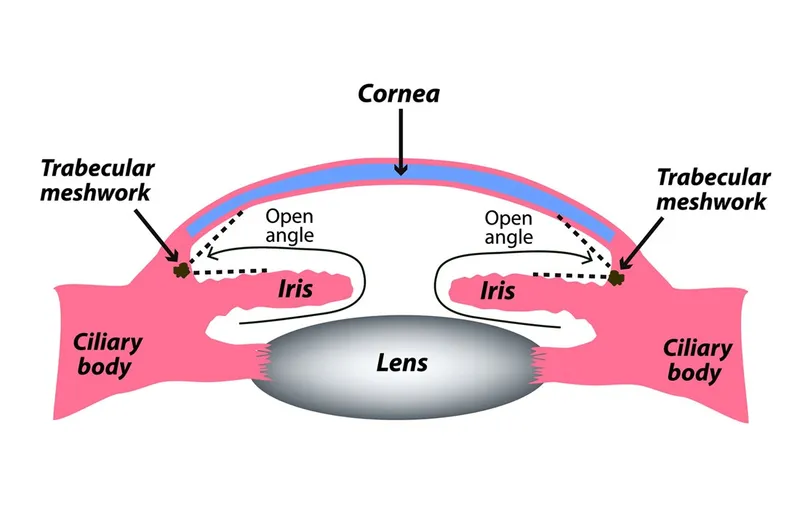
- Enhances aqueous outflow via trabecular meshwork (TM); lowers Intraocular Pressure (IOP).
- Argon Laser Trabeculoplasty (ALT):
- Thermal effect (Argon laser); coagulative burns → mechanical TM stretching.
- Spot size: 50 µm; Duration: 0.1 sec; Power: 300-1000 mW.
- Typically ~50 spots applied over 180°; can treat up to 360°.
- Risks: Transient IOP spike, peripheral anterior synechiae (PAS); scarring limits repeatability.
- Selective Laser Trabeculoplasty (SLT):
- Q-switched, frequency-doubled Nd:YAG laser (532 nm).
- Selectively targets pigmented TM cells (photothermolysis) with minimal thermal spread.
- Spot size: 400 µm (fixed); Duration: 3 ns; Energy: 0.4-1.2 mJ.
- Typically ~100-120 non-overlapping spots over 360°.
- Mechanism: Induces biological response (cytokine release, macrophage recruitment) → TM remodeling.
- Repeatable; less inflammation and structural damage than ALT.
- Indications: Primary open-angle glaucoma (POAG), normal-tension glaucoma (NTG), pigmentary glaucoma, pseudoexfoliation glaucoma. Can be primary or adjunctive therapy.
⭐ SLT is often considered a first-line laser option for open-angle glaucoma due to its favorable safety profile, non-destructive nature, and repeatability compared to ALT.
 Mnemonic: "SLT is Selective & Safe & Superiorly repeatable."
Mnemonic: "SLT is Selective & Safe & Superiorly repeatable."
Laser Iridotomy & Iridoplasty - Angle Attackers
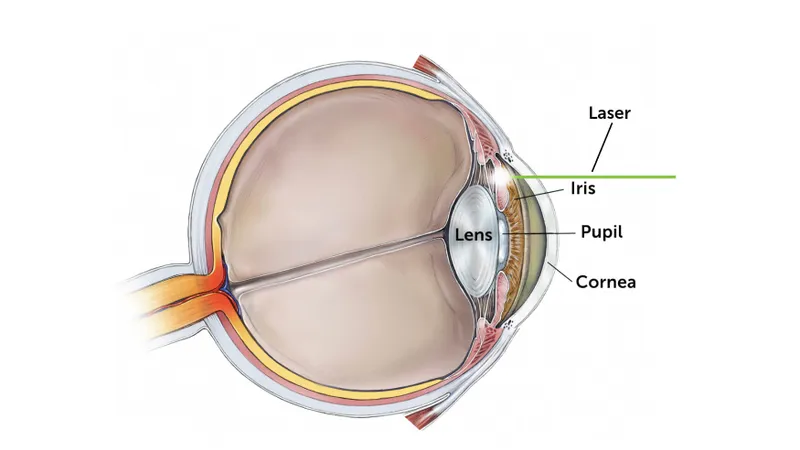
- Laser Iridotomy (LI): Full-thickness iris opening.
- Mechanism: Relieves pupillary block, equalizing pressure between anterior & posterior chambers.
- Indications: Primary Angle Closure Glaucoma (PACG), Primary Angle Closure (PAC), high-risk Primary Angle Closure Suspect (PACS), secondary pupillary block.
- Laser: Nd:YAG. Site: Superior (e.g., 11/1 o'clock), mid-peripheral iris, often at a crypt.
- Key: Patentcy vital. Target size ~150-200 µm.
- Complications: IOP spike (commonest), hyphema, iritis, dysphotopsia, corneal burn.
- Laser Peripheral Iridoplasty (LPI / ALPI): Contracts peripheral iris stroma.
- Mechanism: Mechanically pulls peripheral iris from Trabecular Meshwork (TM); for non-pupillary block mechanisms (e.g., Plateau Iris).
- Indications: Plateau Iris Syndrome/Configuration, persistent appositional closure post-patent LI.
- Laser: Argon.
- Complications: Iris atrophy, pigment dispersion, transient IOP ↑, iritis.
⭐ Prophylactic LI in the fellow eye of a patient experiencing acute angle closure glaucoma (AACG) dramatically reduces the risk of an AACG attack in that fellow eye by over 90% within 5 years compared to no treatment.
Cyclodestructive Lasers - Ciliary Crushers
- Principle: Ablate ciliary body epithelium → ↓ aqueous humor production.
- Indications:
- Refractory glaucoma (failed medical/surgical treatments).
- Painful blind eye (e.g., neovascular glaucoma, absolute glaucoma).
- Glaucoma with poor visual prognosis.
- Types & Techniques:
- Transscleral Cyclophotocoagulation (TSCPC):
- External application (Diode, Nd:YAG laser).
- Targets ciliary body through sclera.
- Common: Diode laser (810 nm).
- Risks: Hypotony, Inflammation, Pain, Phthisis bulbi, Sympathetic ophthalmia (rare) (📌 HIPPS).
- Endoscopic Cyclophotocoagulation (ECP):
- Internal approach via endoscope (Diode laser).
- Direct visualization & treatment of ciliary processes.
- Often combined with phacoemulsification.
- More targeted, potentially less collateral damage.
- Transscleral Cyclophotocoagulation (TSCPC):
- Primary Goal: Significant IOP ↓.
⭐ ECP allows direct visualization of ciliary processes, offering more precise ablation compared to the "blind" approach of TSCPC.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- ALT and SLT improve trabecular outflow in OAG; SLT is selective, repeatable, and often preferred.
- Laser Peripheral Iridotomy (LPI) is crucial for angle-closure glaucoma (ACG), bypassing pupillary block.
- Cyclophotocoagulation (CPC), including TSCPC and ECP, reduces aqueous production in refractory glaucoma.
- A transient IOP spike is a common early complication after trabeculoplasty (ALT/SLT).
- LPI is first-line for acute angle-closure crisis and prophylactic in narrow angles (occludable angles).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

