Overview & Classification - Eye Development Drama
- Developmental glaucomas: Group of disorders with ↑IOP from birth/early childhood due to abnormal aqueous outflow pathway development (trabeculodysgenesis).
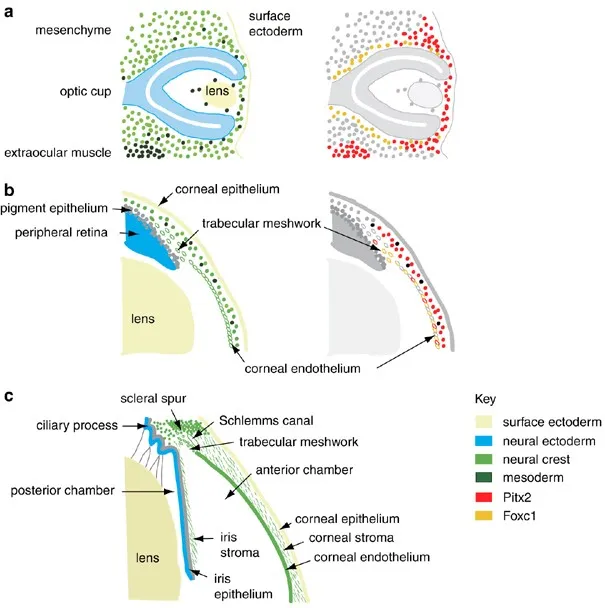
- Embryology: Primarily due to maldevelopment of neural crest cells, which form the trabecular meshwork (TM) and Schlemm's canal.
- Classification:
- Primary Congenital Glaucoma (PCG): Isolated trabeculodysgenesis.
- Glaucomas with Ocular/Systemic Anomalies: e.g., Axenfeld-Rieger, Peters anomaly.
- Secondary Developmental Glaucomas: e.g., due to phakomatoses, inflammation, trauma, tumors.
⭐ Congenital glaucomas result from developmental abnormalities of the anterior chamber angle (trabeculodysgenesis).
PCG: Features & Diagnosis - The Buphthalmos Burden
- Etiology: Trabeculodysgenesis (maldevelopment of trabecular meshwork).
- Genetics: Most commonly associated with CYP1B1 gene mutations.
- Clinical Triad (📌 Mnemonic: BLEP):
- Blepharospasm
- Lacrimation (Epiphora)
- Photophobia
- Key Signs:
- Corneal edema (hazy cornea).
- Haab's striae (breaks in Descemet's membrane).
- Increased corneal diameter: >12mm at 1 year, >13mm anytime.
- Buphthalmos (enlarged globe, "ox eye").
- Deep anterior chamber (AC).
- Intraocular Pressure (IOP) >21 mmHg.
- Optic Disc: Cupping, initially reversible.
- Investigations:
- Examination Under Anesthesia (EUA).
- Tonometry (IOP measurement).
- Corneal diameter measurement.
- Gonioscopy (visualize angle structures).
- Ophthalmoscopy (optic disc assessment).

⭐ Haab's striae, pathognomonic for congenital glaucoma, are horizontal or circumferential breaks in Descemet's membrane due to corneal stretching.
PCG: Management - Angle Attack Plan
- Goals: ↓IOP to safe levels, preserve vision, prevent amblyopia.
- Medical (Bridge to Surgery):
- Topical: β-blockers (e.g., timolol), CAIs (e.g., dorzolamide).
- PGAs generally less effective. Avoid miotics (may ↑IOP).
- Systemic: Acetazolamide (short-term, pre-op).
- Surgical (Definitive):
* If initial surgery fails or for older children: Combined Trabeculotomy-Trabeculectomy (CTT), Trabeculectomy + MMC/5-FU.
* Refractory cases: Glaucoma Drainage Devices (GDDs).
* Last resort: Cyclodestructive procedures.
> ⭐ Goniotomy and trabeculotomy are the primary surgical interventions for PCG, directly addressing the underlying trabeculodysgenesis.
- Prognosis: Better with early diagnosis and surgery; lifelong monitoring essential.
Syndromic & Secondary Glaucomas - Glaucoma's Entourage
- Axenfeld-Rieger Syndrome: PITX2/FOXC1 genes. Key signs: posterior embryotoxon, iris hypoplasia, corectopia. Glaucoma risk: ~50%.
- Peters Anomaly: Central corneal opacity (leukoma), iridocorneal & lenticulocorneal adhesions. Glaucoma risk: ~50-70%.
- Aniridia: PAX6 gene. Iris aplasia/hypoplasia, foveal hypoplasia, nystagmus. Glaucoma risk: ~50-75%.

- Sturge-Weber Syndrome: GNAQ gene. Facial port-wine stain (nevus flammeus).
⭐ In Sturge-Weber syndrome, glaucoma is typically ipsilateral to the facial port-wine stain and can be caused by elevated episcleral venous pressure or an anomalous angle.
- Neurofibromatosis Type 1 (NF1): Lisch nodules (iris hamartomas), developmental angle anomaly causing glaucoma.
- Lowe Syndrome (Oculocerebrorenal): X-linked. Congenital cataracts, renal tubular dysfunction. Glaucoma risk: ~50%.
- Briefly: Marfan, Weill-Marchesani, Rubella_._
Juvenile OAG - Teen Tension Trouble
- Onset: 4-35 years (Open-Angle Glaucoma).
- Presentation: Often asymptomatic; leads to advanced optic disc cupping.
- Management: Similar to adult POAG; more aggressive course, often needs early surgery.
⭐ Juvenile Open-Angle Glaucoma (JOAG) is strongly associated with mutations in the MYOC (myocilin) gene (Autosomal Dominant) and often presents with very high intraocular pressures.
High‑Yield Points - ⚡ Biggest Takeaways
- PCG often bilateral; presents with Haab's striae, buphthalmos, classic triad (photophobia, epiphora, blepharospasm).
- Most PCG: autosomal recessive, CYP1B1 gene.
- Goniotomy/trabeculotomy are key PCG surgeries.
- Axenfeld-Rieger syndrome: posterior embryotoxon, iris changes, glaucoma (50%); PITX2/FOXC1 genes.
- Peters anomaly: central corneal opacity, irido/lenticulocorneal adhesions; glaucoma (50-70%).
- Aniridia (PAX6 mutation): high glaucoma risk (50-75%), often later onset.
- Sturge-Weber syndrome: glaucoma via ↑ episcleral venous pressure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

