Angle Anatomy & Gonioscopy Basics - Peeking & Probing
-
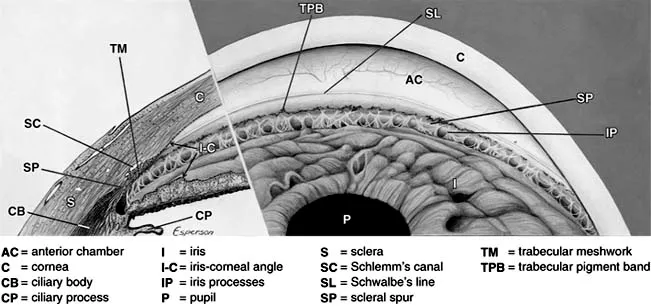
Angle Structures (Anterior to Posterior): 📌 S-L-T-C
- Schwalbe's Line (SL): Termination of Descemet's membrane; anterior-most structure.
- Trabecular Meshwork (TM): Pigmented (functional) & non-pigmented parts; main site of aqueous outflow.
- Scleral Spur (SS): Whitish band; ciliary body attachment. Key landmark for TM identification.
- Ciliary Body Band (CBB): Grey/brown band; anterior aspect of ciliary body. Most posterior structure.
-
Gonioscopy Principles:
- Visualizes the iridocorneal angle, overcoming total internal reflection at the air-cornea interface.
- Direct Gonioscopy: (e.g., Koeppe lens)
- Patient supine; provides a panoramic, erect view of the angle.
- Indirect Gonioscopy: (e.g., Goldmann, Zeiss lenses)
- Uses mirrors at the slit lamp; provides an inverted, virtual image.
- Goldmann: Single mirror (routine, 62° inclination), 3-mirror.
- Zeiss: 4 mirrors (good for indentation, 64° inclination).
- Indentation Gonioscopy: (Dynamic)
- Differentiates appositional (angle opens) vs. synechial (angle remains closed) angle closure.
⭐ The Scleral Spur (SS) is the most crucial and consistent landmark in gonioscopy, essential for identifying the Trabecular Meshwork (TM) located just anterior to it.
Gonioscopic Techniques & Grading - Sizing Up the Space
-
Types of Gonioscopy:
- Direct: Koeppe lens (patient supine; diagnostic/surgical).
- Indirect: Goldmann (3-mirror), Zeiss/Posner/Sussman (4-mirror) (patient at slit-lamp).
- Indentation Gonioscopy (Forbes Test): Differentiates appositional (angle opens with pressure) vs. synechial (angle remains closed/fixed) closure. Crucial for Primary Angle Closure Glaucoma (PACG) assessment.
-
Angle Structures (Posterior to Anterior): 📌 "Can't See Till Sunrise"
- Ciliary Body Band (CBB): Darkest, grey-brown band.
- Scleral Spur (SS): Whitish, prominent line; attachment for ciliary muscle.
- Trabecular Meshwork (TM): Pigmented (posterior, functional) & non-pigmented (anterior). Site of aqueous outflow.
- Schwalbe's Line (SL): Anterior limit of angle; termination of Descemet's membrane.
-
Shaffer Grading (Angle Width):
- Grade 4 (35-45°): CBB visible; Widest, safest.
- Grade 3 (25-35°): SS visible; Open, no closure risk.
- Grade 2 (20°): TM visible; Narrow, closure possible.
- Grade 1 (≤10°): Only SL/part of TM visible; Very narrow, high risk of closure.
- Grade 0 (0°): Closed; Iris in contact with cornea, no structures visible.
-
Spaeth System: More detailed: Records Iris insertion (A-E), Angular width (degrees), Peripheral Iris Contour (f-flat, c-concave, p-plateau, s-steep, b-bowed).
⭐ In Shaffer's grading, an angle of Grade 2 (20°) or less is considered critically narrow (occludable angle) and indicates a significant risk for acute angle closure glaucoma.
Advanced Imaging & Clinical Signs - Tech View & Tell-Tales
- Ultrasound Biomicroscopy (UBM)
- High resolution (25-50 µm); contact procedure.
- Visualizes ciliary body, sulcus, posterior chamber (PC).
- Key for: Plateau iris, cysts, tumors, cyclodialysis clefts, sulcus pathology.
- Anterior Segment OCT (AS-OCT)
- Non-contact, rapid; light-based imaging.
- Types: SD-OCT, SS-OCT (deeper penetration, wider field).
- Measures: Angle Opening Distance (AOD), Trabecular-Iris Space Area (TISA), ACA.
- Details TM, Schwalbe's line, iris profile; quantifies angle.
- Scheimpflug Imaging (e.g., Pentacam)
- Non-contact, rotating camera; 3D anterior segment analysis.
- Measures ACD, ACV, lens parameters. Less angle structure detail.
- Key Clinical Signs (Tell-Tales)
- PAS (Peripheral Anterior Synechiae): Iris adherent to TM/cornea; chronic angle closure.
- Sampaolesi's Line: Pigment line anterior to Schwalbe's (PEX, PDS).
- Blood in Schlemm's Canal: Due to ↑EVP or ocular hypotony.
- NVA (Angle Neovascularization): Pathognomonic for neovascular glaucoma (NVG).
⭐ UBM remains unparalleled for visualizing structures posterior to the iris, such as the ciliary body, crucial for diagnosing conditions like plateau iris syndrome.
High‑Yield Points - ⚡ Biggest Takeaways
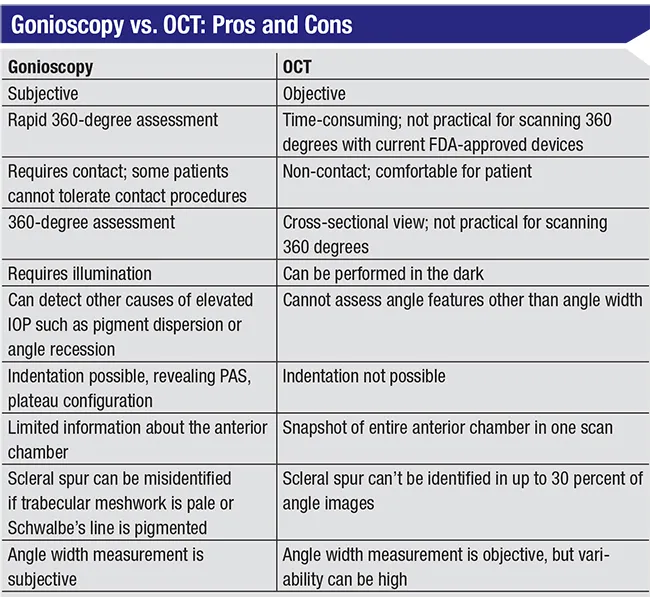
- Gonioscopy remains the gold standard for direct iridocorneal angle visualization.
- Shaffer's grading (Grade 0-closed to 4-widest) is a key clinical classification.
- Angle structures (posterior to anterior): Ciliary Body Band, Scleral Spur, Trabecular Meshwork, Schwalbe's Line.
- Indentation gonioscopy is crucial to differentiate appositional from synechial angle closure.
- Van Herick technique: Slit-lamp estimation; peripheral ACD ≤1/4 corneal thickness suggests occludable angle.
- UBM and AS-OCT offer objective imaging, especially with opaque media or for detailed structure analysis; AS-OCT is non-contact.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

