Scleral Trauma - Wall Woes
- Scleral injury: Blunt (rupture) or sharp (laceration, penetration, perforation).
- Causes: Trauma (sports, RTA, assault), iatrogenic.
- Rupture: Globe gives way at weakest points.
- Common sites: Limbus, behind rectus muscle insertions, prior surgical scars.
- Signs: ↓IOP (often < 5 mmHg), deep/shallow AC, uveal prolapse, hemorrhagic chemosis, bullous subconjunctival hemorrhage (360°), positive Seidel's test.
- Laceration: Sharp object cuts sclera.
- Partial or full thickness.
- Diagnosis: Clinical exam, B-scan USG (if view obscured), CT scan (for IOFB).
- Management: Surgical exploration & repair (primary closure), rule out/remove IOFB, systemic antibiotics.
⭐ Thinnest Sclera: 0.3 mm just posterior to rectus muscle insertions, making it a common site for traumatic rupture.
📌 Mnemonic (Rupture Sites): "Limp Really Slow" - Limbus, Rectus insertions, Scars.
Open Globe Injuries - Globe Gone Wild
Full-thickness scleral/corneal wound. Guarded prognosis.
BETT Classification (OGI):
| Feature | Description |
|---|---|
| Type | A: Rupture; B: Penetrating; C: IOFB; D: Perforating; E: Mixed |
| Grade (VA) | 1: ≥20/40; 2: 20/50-20/100; 3: 19/100-5/200; 4: 4/200-LP; 5: NLP |
| Pupil | P: +ve RAPD; N: -ve RAPD |
| Zone | I: Cornea/limbus; II: Limbus to 5mm post. sclera; III: >5mm post. limbus |
Features & Management:
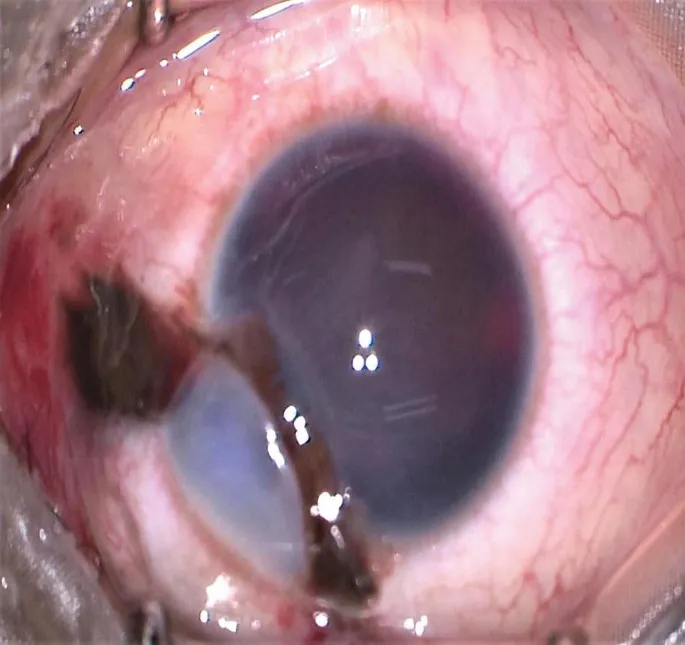
- Signs: Peaked pupil, uveal prolapse, ↓IOP, +ve Seidel test, hemorrhagic chemosis.
- Imaging: CT scan (NO MRI if metallic IOFB suspected).
- Rx: Shield eye (NO patch). IV antibiotics. Tetanus toxoid. Antiemetics. Surgical repair ASAP.
⭐ Common scleral rupture sites (blunt trauma): Limbal (especially superonasal), under rectus muscle insertions, posterior (near optic nerve), and at sites of prior ocular surgery.
Clinical Clues & Imaging - Trauma Telltales
- Symptoms: Severe pain, ↓ vision, photophobia.
- Signs (Ocular Exam):
- Marked conjunctival injection, chemosis, 360° subconjunctival hemorrhage.
- Peaked pupil, uveal prolapse (dark knuckle).
- Shallow/flat anterior chamber (AC).
- IOP: Often low (< 5 mmHg), can be normal/high.
- Positive Seidel's test (fluorescein stream).
- Relative Afferent Pupillary Defect (RAPD).
- Imaging:
- B-scan USG: Essential for opaque media. Detects rupture, vitreous/retinal/choroidal detachment, IOFB.
- CT Scan (Orbit): For IOFB (metallic), fractures. "Flat tire" sign.
- UBM: Details anterior scleral/ciliary body injury.
⭐ Seidel's test (fluorescein streaming) confirms aqueous leak, pathognomonic for open globe. RAPD indicates significant optic nerve/retinal damage, poor prognosis.
Scleral Repair & Recovery - Suture & Soothe
- Surgical Repair Principles:
- Goal: Watertight, anatomical closure.
- Timing: Urgent, ideally within 24 hours.
- Sutures: 8-0 to 10-0 Nylon (non-absorbable), interrupted.
- Technique: Meticulous apposition, avoid uveal incarceration, explore thoroughly.
- Post-operative Management ("Soothe"):
- Topical: Broad-spectrum antibiotics (e.g., Moxifloxacin), potent steroids (e.g., Prednisolone).
- Systemic: Antibiotics for penetrating injuries or intraocular foreign body (IOFB) cases.
- Cycloplegics (e.g., Atropine) for comfort, prevent synechiae.
- Protective eye shield.
- Key Complications:
- Endophthalmitis, sympathetic ophthalmia, retinal detachment, phthisis bulbi.
⭐ Principles of scleral wound repair: Achieve watertight closure with meticulous apposition of wound edges, remove foreign bodies/necrotic tissue, and avoid incarceration of uveal tissue. Consider evisceration/enucleation for no light perception (NLP) with extensive damage or uncontrollable pain in a blind eye.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Scleral rupture is a full-thickness scleral defect, often occult; maintain high suspicion post-trauma.
- Common rupture sites: Limbus, under rectus muscle insertions, and the posterior pole.
- Key signs: ↓VA, uveal/retinal prolapse, hemorrhagic chemosis, low IOP (can be variable).
- Seidel's test (fluorescein streaming) confirms an active aqueous leak.
- B-scan ultrasonography (USG) is vital for diagnosis, especially with opaque media or suspected posterior rupture.
- Immediate surgical exploration and primary scleral repair are mandatory for open globe injuries.
- Poor prognostic signs include Relative Afferent Pupillary Defect (RAPD), initial VA < Perception of Light (PL), and a large wound (>10mm).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

