Sclera: Anatomy & Physiology - Eye's White Coat
- Tough, opaque, fibrous protective outer layer; forms posterior 5/6th of the eyeball. "White of the eye".
- Composition: Primarily dense Type I collagen bundles, some elastic fibers. Largely avascular.
- Thickness: Variable:
- Posterior pole: 1.0 mm
- Equator: 0.4-0.6 mm
- Under EOM insertions: 0.3 mm (thinnest part)
- Layers (Outer to Inner): Episclera (vascular loose connective tissue), Sclera proper (dense avascular stroma), Lamina fusca (innermost, pigmented).
- Apertures:
- Optic nerve (via Lamina cribrosa - weakest structural point).
- Vortex veins.
- Long & short ciliary arteries & nerves.
- Functions: Maintains globe shape, protects intraocular structures, provides EOM attachment.
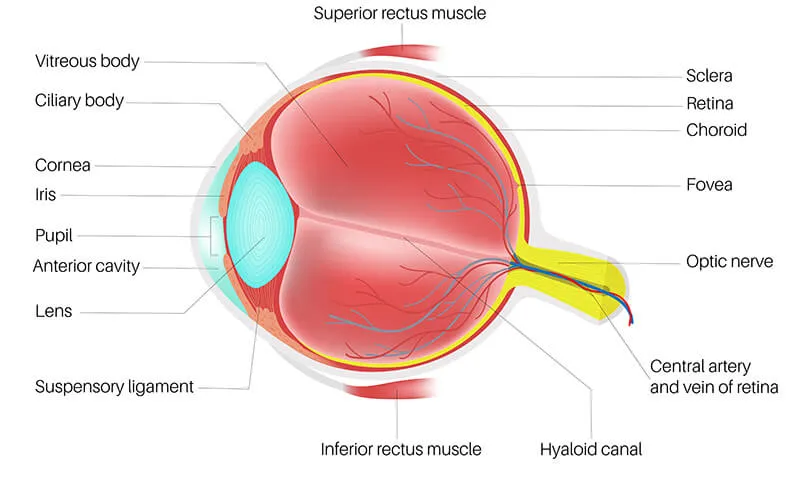
⭐ The sclera is thinnest (0.3 mm) at the site of insertion of the rectus muscles, a clinically significant point for potential globe rupture during trauma or surgery.
Sclera: Anatomy & Physiology - Tough Outer Shell

- Function: Tough, opaque, fibrous outer protective layer of the eyeball; maintains globe shape.
- Layers:
- Episclera: Outer, vascularized loose connective tissue.
- Scleral Stroma: Dense, avascular collagenous tissue (Type I collagen); irregular arrangement causes opacity.
- Lamina Fusca: Innermost, pigmented layer, blends with choroid.
- Thickness:
- Posteriorly (around optic nerve): 1.0-1.35mm
- Anteriorly (at limbus): 0.8mm
- Equator: 0.4-0.6mm
- Under rectus muscle insertions: 0.3mm (thinnest, prone to rupture).
- Openings (Foramina):
- Anterior: Scleral spur, trabecular meshwork.
- Posterior: Lamina cribrosa (optic nerve fibres pass).
- Middle: Vortex veins (4-7), long/short posterior ciliary arteries & nerves.
- Attachments: Extraocular muscles (EOMs).
- Blood Supply: Largely avascular stroma; supplied by episcleral & choroidal vessels.
- Nerve Supply: Branches of ciliary nerves.
⭐ The sclera is thinnest (0.3mm) beneath the insertions of the rectus muscles, making it a site of potential rupture from trauma.
- Composition: Collagen (mainly Type I), elastin, proteoglycans. Hydration level (68%) critical for opacity. 📌 Strong Collagen Layers Ensure Rigid Architecture (SCLERA).
Sclera: Anatomy & Physiology - Microscopic Might

- Core Matrix: Dense, irregular connective tissue.
- Collagen Type I: Predominant (~90%); fibers vary in diameter (25-230 nm) and spacing. Irregular arrangement scatters light, causing opacity.
- Fibroblasts (Sclerocytes): Synthesize and maintain extracellular matrix (ECM).
- Proteoglycans: (e.g., decorin) Regulate hydration, influence collagen fibril assembly and spacing.
- Elastic Fibers: Fewer than collagen; provide some elasticity.
- Avascularity: Lacks intrinsic blood vessels.
- Nourished by diffusion from episclera and choroid.
- Scleral foramina allow passage for nerves/vessels (optic nerve, ciliary vessels).
⭐ The sclera's avascularity and dense collagen make it relatively inert metabolically, contributing to its white appearance and slow healing after injury or surgery.
Sclera: Anatomy & Physiology - Shape & Strength
- Forms posterior 5/6th of eye's fibrous tunic; opaque, white.
- Shape Maintenance: Provides rigid framework, maintains globe shape against Intraocular Pressure (IOP) & Extraocular Muscle (EOM) forces.
- Strength & Rigidity: Derived from dense, irregular Type I collagen fibers & elastin.
- Collagen fibrils (25-230 nm diameter) arranged in lamellae parallel to scleral surface.
- Interweaving bundles provide high tensile strength.
- IOP Resistance: Critical for resisting normal IOP (typically 10-21 mmHg) & transient spikes, preventing globe expansion.
- Viscoelasticity: Exhibits time-dependent stress-strain behavior, allowing deformation under load & subsequent recovery.
- Thickness varies: 1.0 mm at posterior pole, 0.3 mm under rectus muscle insertions (thinnest point), 0.6 mm at equator, 0.8 mm at limbus.
⭐ The sclera is thinnest (0.3 mm) just posterior to the insertions of the extraocular rectus muscles, making these sites vulnerable to globe rupture from blunt trauma.
High‑Yield Points - ⚡ Biggest Takeaways
- Avascular structure, receives nutrition from episclera and choroid.
- Composed of dense Type I collagen fibers, providing strength and shape to the eyeball.
- Thinnest at the rectus muscle insertions (0.3 mm), thickest at the posterior pole (1.0 mm).
- Lamina fusca: innermost, pigmented layer, adjacent to choroid.
- Blue sclera indicates thinness, seen in conditions like osteogenesis imperfecta or Marfan syndrome.
- Nerve supply from long and short ciliary nerves.
- Weakest points: lamina cribrosa and scleral canals for vortex veins.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

