Definition, Anatomy & Types - Retina's Rip Roar
- Definition: Separation of neurosensory retina (NSR) from retinal pigment epithelium (RPE).
- Anatomy:
- NSR: Inner 9 layers; RPE: Outermost layer.
- Ora serrata: Anterior termination of retina.
- Potential space between NSR & RPE.
- Types:
- Rhegmatogenous (RRD): Retinal break (hole/tear) → vitreous fluid ingress. 📌 Rhegma = Rent/Break.
- Tractional (TRD): Vitreoretinal membranes pull NSR (e.g., Proliferative Diabetic Retinopathy, Retinopathy of Prematurity).
- Exudative/Serous (ERD): Subretinal fluid (no break) from RPE/choroid pathology (e.g., tumors, inflammation).
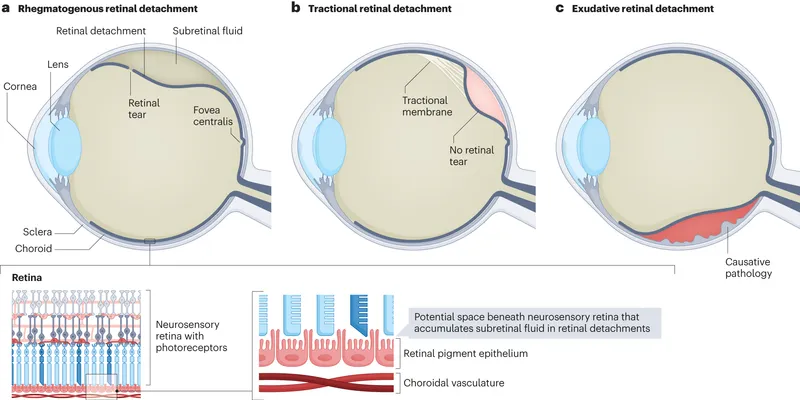
⭐ Rhegmatogenous RD (RRD) is the most common type of retinal detachment, accounting for the majority of cases.
Etiology & Risk Factors - The Unsticking Story
- Rhegmatogenous (RRD): Most common type. Retinal break → fluid entry.
- Risks: Posterior Vitreous Detachment (PVD) (most common precursor), myopia (> -6D), trauma, aphakia/pseudophakia, lattice degeneration, family history.
- Tractional (TRD): Vitreoretinal membranes contract & pull retina.
- Risks: Proliferative Diabetic Retinopathy (PDR - commonest cause), Retinopathy of Prematurity (ROP), sickle cell retinopathy, trauma.
- Exudative (ERD): Subretinal fluid from damaged RPE/choroid; no retinal break.
- Risks: Choroidal tumors (e.g., melanoma), inflammation (e.g., Vogt-Koyanagi-Harada [VKH] syndrome), Coats' disease, severe hypertension.
⭐ Posterior Vitreous Detachment (PVD) is the most common precursor to Rhegmatogenous Retinal Detachment (RRD).
Clinical Features & Diagnosis - Shadow Signs & Scans
- Symptoms:
- Photopsia (flashes of light), new-onset floaters (cobwebs, shower of black dots).
- Painless, progressive peripheral visual field loss (often described as a "curtain" or "shadow" spreading across vision).
- Sudden decrease in visual acuity if macula becomes involved.
- Signs:
- Relative Afferent Pupillary Defect (RAPD) if RD is extensive.
- Shafer's sign: Pigment cells ("tobacco dust") in the anterior vitreous; pathognomonic for a retinal break.
- Weiss ring: Annular opacity in vitreous anterior to optic disc, indicates Posterior Vitreous Detachment (PVD).
- ↓ Intraocular pressure (IOP) is common, though IOP can be normal or ↑.
- Investigations:
- Indirect Ophthalmoscopy (with scleral indentation): Gold standard. Shows detached retina (greyish, undulating, opaque membrane), retinal breaks (e.g., horseshoe tear, round hole).
⭐ Shafer's sign ("tobacco dust" in anterior vitreous) is highly suggestive of a retinal break.
- B-scan Ultrasonography: Essential if media are opaque (e.g., dense cataract, vitreous hemorrhage) preventing clear fundus view.

Management Principles - Patching the Peel-off
Aims: Close retinal breaks, relieve traction, create chorioretinal adhesion.
- Creating Adhesion:
- Laser photocoagulation: Seals breaks/demarcates subclinical RD.
- Cryopexy: Induces adhesion via freezing.
- Surgical Interventions:
- Pneumatic Retinopexy: Intravitreal gas (e.g., $SF_6$, $C_3F_8$) + retinopexy. For uncomplicated superior RDs. 📌 Gas Up High!
- Scleral Buckle: External support for breaks. Ideal for young, phakic, peripheral breaks.
- Pars Plana Vitrectomy (PPV): Vitreous removal, internal tamponade (gas/oil), endolaser. For complex RDs (PVR, giant tears, posterior breaks).

⭐ > Silicone oil is preferred over gas for long-term tamponade in complex RDs (severe PVR) or if post-op positioning is challenging.
Complications & Prognosis - Aftermath & Outlook
- Complications:
- Early: Endophthalmitis, ↑IOP, choroidal detachment.
- Late: Proliferative Vitreoretinopathy (PVR) (most common failure cause), cataract, macular pucker, hypotony, refractive errors.
- Prognosis Factors:
- Macular status (on/off) - key determinant.
⭐ Macula-off RD > 7-10 days = poorer visual outcome.
- Duration, extent of RD, PVR presence.
- Pre-op VA.
- Macular status (on/off) - key determinant.
- Success Rates: Anatomical ~80-90% (1 surgery); functional varies.
High‑Yield Points - ⚡ Biggest Takeaways
- Rhegmatogenous RD (RRD): most common, from retinal breaks. Tractional: membranes (PDR). Exudative: subretinal fluid, no break.
- Symptoms: sudden floaters, photopsia, painless vision loss, "curtain" defect.
- RRD risks: high myopia, aphakia/pseudophakia, trauma, lattice degeneration.
- Shafer's sign (tobacco dust) in anterior vitreous indicates retinal break.
- Macula-on RRD is an emergency. Surgery (pneumatic retinopexy, buckle, vitrectomy) aims to save vision.
- Lincoff's rules help locate the primary retinal break.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

