Retinal Layers - Ten Tiers Deep

From outermost to innermost:
- RPE (Retinal Pigment Epithelium): Outer blood-retina barrier.
- Photoreceptors: Rods (night), Cones (day, color).
- OLM (Outer Limiting Membrane): Müller cell junctions.
- ONL (Outer Nuclear Layer): Photoreceptor nuclei.
- OPL (Outer Plexiform Layer): 1st synapse (P-B-H); Henle's layer (macula).
- INL (Inner Nuclear Layer): Bipolar, Horizontal, Amacrine, Müller nuclei.
- IPL (Inner Plexiform Layer): 2nd synapse (B-A-G).
- GCL (Ganglion Cell Layer): Ganglion cell nuclei.
- NFL (Nerve Fiber Layer): Ganglion cell axons (to optic nerve).
- ILM (Inner Limiting Membrane): Müller cell footplates; inner boundary.
📌 Mnemonic (Outermost to Innermost): Rich People Often Order Oranges, Including Imported Grapefruit, Nectarines, Instead.
⭐ OPL is a key watershed zone, with dual blood supply from choroid and central retinal artery (CRA).
Retinal Vasculature - Lifeblood Lines
- Dual supply: Central Retinal Artery (CRA) & Choroid.
- CRA: Inner 2/3 retina (NFL to INL). Branch of ophthalmic artery. End-artery. Forms inner Blood-Retinal Barrier (BRB).
- Choroid: Outer 1/3 retina (OPL to RPE, photoreceptors). Fenestrated. Forms outer BRB with RPE.
- Foveal Avascular Zone (FAZ): Central 0.5mm, relies on choroid.
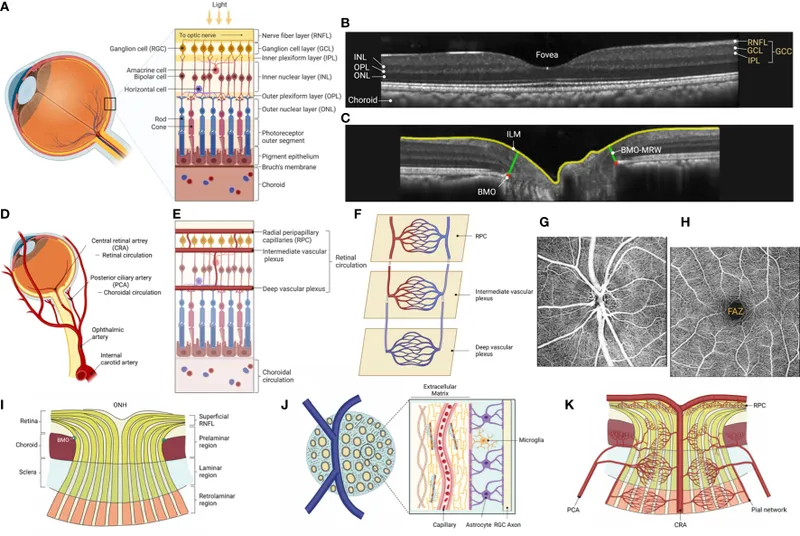
⭐ CRA occlusion leads to a "cherry-red spot" due to visible choroidal circulation through the thin, ischemic inner retina at the fovea, contrasting with the pale, infarcted surrounding retina.
Photoreceptors and Macula - Vision's VIPs
- Photoreceptors: Convert light (photons) to electrical signals.
- Rods (Scotopic Vision):
- ~120 million; high light sensitivity (night vision).
- Rhodopsin pigment. Peripheral retina; low acuity; achromatic.
- Cones (Photopic Vision):
- ~6-7 million; low light sensitivity (day vision).
- Iodopsin (3 types). Central retina (fovea); high acuity; color vision.
- 📌 Mnemonic: Cones = Color & Central.
- Mechanism: Light → ↓ cGMP → Na+ channels close → Hyperpolarization.
- Rods (Scotopic Vision):
- Macula Lutea (~5.5 mm):
- Oval, yellowish (lutein, zeaxanthin); central, high-resolution vision.
- Fovea Centralis (~1.5 mm):
- Highest cone density; peak visual acuity.
- Avascular (Foveal Avascular Zone - FAZ). Inner retinal layers displaced.
- Foveola (~0.35 mm): Center of fovea; thinnest retina; only cones.
⭐ The fovea centralis, containing only cone photoreceptors and being avascular, provides the sharpest visual acuity (VA > 6/6).

Phototransduction Pathway - Light to Sight Cascade
- Dark State: Rods/cones are depolarized. cGMP is high, keeping cGMP-gated Na+ channels open. Glutamate is continuously released.
- Resting membrane potential: -40mV.
- Light Activation:
- Light hits Rhodopsin (Rods) / Photopsin (Cones).
- Retinal changes from 11-cis to all-trans form.
- Activates Transducin (G-protein).
- Transducin activates cGMP Phosphodiesterase (PDE).
- PDE hydrolyzes cGMP to GMP, ↓cGMP levels.
- Na+ channels close → Hyperpolarization.
- ↓Glutamate release → Signal to bipolar cells.
⭐ Inactivation: Rhodopsin kinase phosphorylates activated rhodopsin. Arrestin binds, preventing transducin activation, aiding recovery to dark state. This is crucial for rapid adaptation to changing light levels.
- 📌 Light → Less cGMP → Less Glutamate release (Hyperpolarization).
Retinal Pigment Epithelium (RPE) - Retina's Support Crew
- Single layer of hexagonal, pigmented cells between Bruch's membrane & photoreceptors.
- Functions:
- Phagocytosis of photoreceptor outer segments.
- Vitamin A metabolism (retinoid cycle).
- Blood-retinal barrier (outer).
- Nutrient/waste transport.
- Light absorption, reducing scatter.
- Secretion of growth factors (e.g., PEDF).

⭐ Drusen (lipofuscin deposits) accumulate between RPE & Bruch's membrane, a hallmark of Age-related Macular Degeneration (AMD).
High‑Yield Points - ⚡ Biggest Takeaways
- Retina from neuroectoderm; ora serrata is anterior end.
- Fovea centralis (macula) for sharpest vision (max cones).
- Rods: scotopic (dim light); Cones: photopic (bright light) & color.
- RPE: phagocytosis, Vitamin A cycle, outer blood-retinal barrier.
- Optic disc (blind spot): ganglion cell axons exit, form optic nerve.
- Blood: Inner retina by central retinal artery; outer by choriocapillaris.
- Müller cells: main retinal glia, provide structural/metabolic support.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

