Foundations & Agents - Drug Delivery Drama
- Intravitreal (IVT) Route:
- Direct drug delivery to vitreous.
- Bypasses blood-retinal barrier (BRB).
- Achieves high local drug concentration.
- Minimizes systemic side effects.
- Key Risks:
- Endophthalmitis
- Retinal detachment (RD)
- ↑Intraocular Pressure (IOP)
- Cataract (with steroids)

Common IVT Agents:
| Agent Class | MOA Highlights | Examples (Dose) | Key Uses | Major Risks |
|---|---|---|---|---|
| Anti-VEGF | Binds VEGF-A; ↓neovasc, ↓permeability | Ranibizumab (0.5 mg), Aflibercept (2 mg), Bevacizumab (1.25 mg), Brolucizumab (6 mg) | nAMD, DME, RVO, CNVM | Endophthalmitis, inflammation, ↑IOP, RD |
| Corticosteroids | Anti-inflammatory, ↓permeability, anti-angiogenic | Triamcinolone (4 mg), Dexamethasone implant (0.7 mg), Fluocinolone implant (0.19 mg) | DME, RVO, Uveitis | ↑IOP (glaucoma), cataract, endophthalmitis |
| Antibiotics | Anti-bacterial | Vancomycin, Ceftazidime | Bacterial endophthalmitis | Retinal toxicity (dose), local irritation |
Key Indications - Retina's Rescue Remedies
- Wet AMD (wAMD):
- Patho: CNV (VEGF-driven).
- Drugs: Anti-VEGF (Ranibizumab, Aflibercept, Bevacizumab, Brolucizumab).
- Diabetic Macular Edema (DME):
- Patho: ↑VEGF, inflammation → ↑permeability.
- Drugs: Anti-VEGF; Corticosteroids (Dexamethasone, Fluocinolone implants).
- Retinal Vein Occlusion (RVO) Macular Edema:
- Patho: Ischemia → ↑VEGF → edema.
- Drugs: Anti-VEGF; Corticosteroids.
- Myopic CNV (mCNV):
- Patho: CNV in pathologic myopia (VEGF).
- Drugs: Anti-VEGF.
- Non-infectious Posterior Uveitis:
- Patho: Inflammation → macular edema/vitritis.
- Drugs: Corticosteroids.
- Infectious Endophthalmitis:
- Patho: Intraocular infection.
- Drugs: Antibiotics (Vancomycin+Ceftazidime); Antifungals (Amphotericin B, Voriconazole).
⭐ Wet Age-Related Macular Degeneration (wAMD) and Diabetic Macular Edema (DME) are the most frequent indications for intravitreal anti-VEGF injections.
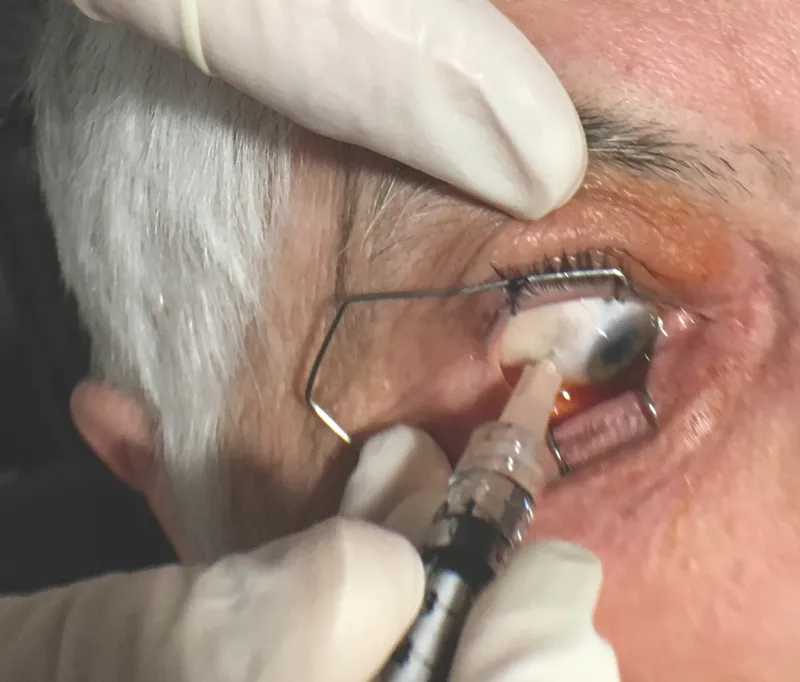
The Injection Journey - Precision Pokes
- Goal: Deliver drug to vitreous, minimize complications.
- Key Prep:
- Anesthesia (topical/subconjunctival).
- Antisepsis: Povidone-iodine 5% or 10% (crucial!).
- The Poke:
- Needle: 30G or 32G.
- Site: 📌 SIT (SuperoTemporal preferred, also InferoTemporal).
- Distance from limbus: Phakic 3.5-4 mm; Pseudophakic/Aphakic 3-3.5 mm.
- Angle: Perpendicular to sclera.

⭐ Strict aseptic technique, including topical povidone-iodine application, is paramount to minimize the risk of post-injection endophthalmitis.
Risks & Roadblocks - Cautionary Tales
-
Common/Mild (Usually Self-Limiting):
- Subconjunctival hemorrhage
- Transient ocular pain, foreign body sensation
- Floaters (e.g., air bubble)
- Transient IOP ↑ (monitor if >21 mmHg)
- Corneal abrasion
-
Serious/Vision-Threatening:
- Endophthalmitis: Incidence ~0.05% per injection. ⚠️ Most feared!
- Key signs: 📌 RSVP (Redness, Severe pain, ↓Vision, Pus/hypopyon)
- Retinal Detachment (RD): Incidence ~0.01-0.7%
- Vitreous Hemorrhage
- Lens Damage / Cataract (esp. phakic eyes)
- Sustained IOP ↑ / Glaucoma
- Sterile Uveitis / Intraocular Inflammation
- Systemic (rare): e.g., thromboembolic events (anti-VEGF)
- Endophthalmitis: Incidence ~0.05% per injection. ⚠️ Most feared!
⭐ Post-injection endophthalmitis, though rare (~0.05%), is the most devastating complication, typically presenting with pain, vision loss, and hypopyon within days.
High‑Yield Points - ⚡ Biggest Takeaways
- Anti-VEGF agents (Ranibizumab, Bevacizumab, Aflibercept) are primary for wet AMD, DME, and RVO.
- Ranibizumab is an antibody fragment; Bevacizumab is a full antibody (used off-label).
- Aflibercept is a potent VEGF trap binding VEGF-A, VEGF-B, and PlGF.
- Intravitreal steroids (Triamcinolone, Dexamethasone implant) treat inflammatory conditions like uveitis, DME, RVO.
- Key risks: endophthalmitis, retinal detachment, increased IOP (↑IOP), and cataract.
- Ozurdex (Dexamethasone implant) is biodegradable; Iluvien (Fluocinolone implant) is non-biodegradable.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

