Posterior Uveitis & Basics - Eye's Inner Turmoil
- Inflammation of posterior segment: choroid (choroiditis), retina (retinitis), or both (chorioretinitis); may involve retinal vessels (vasculitis).
- Key Symptoms: Floaters, ↓ vision, photophobia; pain less common than anterior uveitis.
- Cardinal Signs:
- Vitritis (vitreous cells/haze) - hallmark.
- Chorioretinal inflammatory lesions (yellowish/white patches, fuzzy borders).
- Retinal vasculitis (sheathing, occlusion).
- Broad Etiology:
- Infectious (e.g., Toxoplasma, TB, CMV, Syphilis).
- Non-infectious/Autoimmune (e.g., Sarcoidosis, Behçet's, VKH, Birdshot).
- Diagnosis: Clinical; supported by FFA, ICG, OCT, lab investigations.
⭐ Vitritis, appearing as hazy vision and cells/flare in the vitreous, is a cardinal sign of posterior uveitis.
Infectious Retinal Disease - Microbial Mayhem
- Bacterial Retinitis/Endophthalmitis
- Etiology: Post-op (e.g., cataract surgery), post-trauma, endogenous spread.
- Signs: Rapid vision ↓, pain, hypopyon, severe vitritis.
- Tx: Prompt intravitreal antibiotics (e.g., Vancomycin + Ceftazidime).
- Viral Retinitis
- CMV Retinitis:
- Setting: Immunocompromised (AIDS, CD4 < 50 cells/$\text{µL}$).
- Appearance: Indolent; "pizza pie" / "cottage cheese & ketchup" (hemorrhages, exudates).
- Tx: Ganciclovir (systemic/intravitreal), Foscarnet.
- Acute Retinal Necrosis (ARN):
- Etiology: HSV, VZV; often in immunocompetent individuals.
- Features: Rapidly progressive peripheral necrotizing retinitis, occlusive vasculitis, prominent vitritis. "Brushfire" border.
- Tx: IV Acyclovir, systemic steroids (after antivirals initiated).
- Progressive Outer Retinal Necrosis (PORN):
- Etiology: VZV; severe immunocompromise (e.g., AIDS).
- Features: Rapid, widespread necrosis; minimal vitritis; poor prognosis.
- Tx: Aggressive combination antivirals.
- CMV Retinitis:
- Fungal Retinitis/Endophthalmitis
- Etiology: Candida (common in IV drug users, indwelling catheters), Aspergillus.
- Appearance: Fluffy white chorioretinal lesions; Candida may show "string of pearls" in vitreous.
- Tx: Systemic & intravitreal antifungals (e.g., Amphotericin B, Voriconazole).
- Parasitic Retinochoroiditis
- Toxoplasmosis: Most common cause of infectious posterior uveitis.
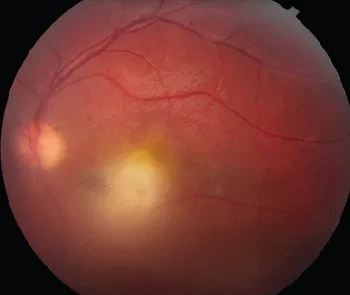
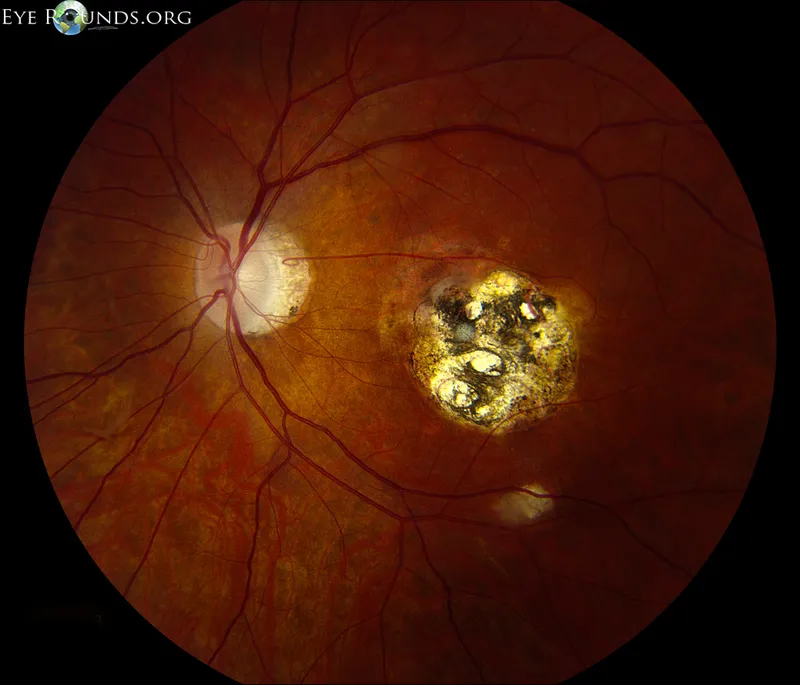
⭐ Toxoplasmic retinochoroiditis classically presents as a 'headlight in the fog' appearance due to focal necrotizing retinitis adjacent to an old pigmented scar, with overlying vitritis.
- Tx: Triple therapy (Pyrimethamine, Sulfadiazine, Corticosteroids). 📌 Mnemonic: "PSC" for treatment.
- Toxocariasis (Ocular Larva Migrans - OLM):
- Population: Typically children (exposure to soil contaminated with dog/cat feces).
- Presentation: Unilateral vision ↓, strabismus; posterior pole granuloma, peripheral granuloma, or chronic endophthalmitis.
- Tx: Corticosteroids; antihelminthics (e.g., Albendazole) for active larva.
- Toxoplasmosis: Most common cause of infectious posterior uveitis.
Non-Infectious Retinal Disease - Immune Overdrive
- Autoimmune/autoinflammatory processes targeting retina/uvea; often bilateral with systemic links. Management: corticosteroids, immunosuppressants.
- Behçet's Disease:
- Systemic vasculitis (recurrent oral/genital ulcers, skin lesions).
- Ocular: Severe panuveitis, hypopyon, occlusive retinal vasculitis (arteritis > phlebitis), retinal hemorrhages, neovascularization, optic atrophy.
- HLA-B51 association.
⭐ Bilateral, occlusive retinal vasculitis is a hallmark of Behçet's disease and can lead to severe vision loss.
- Sarcoidosis:
- Multisystem granulomatous disorder.
- Ocular: Uveitis (any part), "candle-wax drippings" periphlebitis (venous sheathing), choroidal/optic nerve granulomas, CME.
- ↑ Serum ACE, lysozyme; CXR for hilar lymphadenopathy.
- Vogt-Koyanagi-Harada (VKH) Syndrome:
- Targets melanocytes; HLA-DR4.
- Phases: Prodromal (flu-like, meningism) → Ophthalmic (bilateral granulomatous panuveitis, multifocal serous RD, disc hyperemia) → Convalescent (sunset glow fundus, vitiligo, poliosis).
- Sympathetic Ophthalmia:
- Rare bilateral granulomatous panuveitis after penetrating trauma/surgery to one eye (exciting eye).
- Dalen-Fuchs nodules (epithelioid cells over RPE).
- Birdshot Chorioretinopathy:
- Chronic, bilateral posterior uveitis; strong HLA-A29 association (>90%).
- Creamy, ovoid "birdshot" lesions deep, radiating from optic disc; vitritis, vasculitis, CME.
High‑Yield Points - ⚡ Biggest Takeaways
- Toxoplasmosis: Most common infectious posterior uveitis; classic "headlights in fog" appearance.
- CMV retinitis: Affects AIDS patients (CD4 < 50); "pizza pie" or "cottage cheese & ketchup" fundus.
- ARN: Caused by herpes viruses (VZV/HSV); presents with peripheral necrosis, vasculitis, and vitritis.
- Sarcoidosis: Features retinal periphlebitis ("candle wax drippings") and choroidal granulomas.
- Behcet's disease: Associated with HLA-B51; causes occlusive retinal vasculitis and hypopyon.
- Ocular Toxocariasis: Unilateral in children; posterior pole granuloma or peripheral inflammatory mass.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

