Intro & Pathophysiology - Sweet Retinal Damage
- Diabetic Retinopathy (DR): Most common microvascular complication of Diabetes Mellitus (DM). A leading cause of preventable blindness in working-age adults globally.
- Pathophysiology: Driven by chronic hyperglycemia.
- Key mechanisms:
- Polyol pathway: Aldose reductase converts glucose to sorbitol → osmotic stress, cellular damage.
- Advanced Glycation End-products (AGEs): Accumulate, causing vascular dysfunction, ↑permeability.
- Protein Kinase C (PKC) activation: Stimulates VEGF, promoting angiogenesis and leakage.
- Key mechanisms:
⭐ Pericyte loss is the earliest detectable histological change in diabetic retinopathy.
- Consequences: Breakdown of Blood-Retinal Barrier (BRB), capillary non-perfusion, retinal ischemia/hypoxia, leading to VEGF upregulation.
Classification & Features - Retina's Red Alerts
- Non-Proliferative DR (NPDR): No neovascularization.
- Mild: ≥1 Microaneurysm (MA).
- Moderate: MAs, dot/blot hemorrhages (H), hard exudates (HE), Cotton Wool Spots (CWS). Not severe NPDR.
- Severe (4-2-1 Rule): Any 1 of:
- Severe H/MA in 4 quadrants.
- Venous beading (VB) in ≥2 quadrants.
- IRMA (Intraretinal Microvascular Abnormalities) in ≥1 quadrant.
- Very Severe: ≥2 criteria for severe NPDR.
- Proliferative DR (PDR): Neovascularization (NV) present.
- NVD (NV of Disc) / NVE (NV Elsewhere).
- Complications: Vitreous hemorrhage, Tractional Retinal Detachment (TRD).
- Diabetic Macular Edema (DME): Macular thickening/exudates. Commonest cause of vision loss. Can occur at any stage.
⭐ Neovascularization (NVD/NVE) is the hallmark of Proliferative Diabetic Retinopathy (PDR).
 oka
oka
Diagnosis & Investigations - Eye Detective Tools
- Dilated Fundoscopy: Essential first step. Identifies microaneurysms, hemorrhages, hard exudates, cotton wool spots, IRMA, NVD, NVE.
- Key Imaging Modalities:
- Fundus Photography: Baseline documentation; monitors progression.
- Optical Coherence Tomography (OCT): Gold standard for DME detection & quantification; measures central macular thickness.
- Fluorescein Angiography (FFA): Visualizes retinal circulation; detects leakage, macular ischemia, neovascularization. Critical for PDR.
- OCT Angiography (OCT-A): Non-invasive; details microvasculature; alternative to FFA.
- Systemic Evaluation: Crucial for management: HbA1c, blood pressure, lipid profile, renal function.

⭐ Fluorescein Angiography (FFA) is crucial for detecting neovascularization and macular ischemia.
Management - Sight-Saving Tactics
- Core Aim: Prevent vision loss; stabilize/improve sight.
- Systemic Control: Essential foundation.
- Glycemic (HbA1c < 7%), BP (< 140/90 mmHg), Lipid optimization.
- Ocular Therapies: Tailored to severity.
- Laser Photocoagulation:
- PRP (Pan-Retinal): For PDR, severe NPDR. Reduces neovessels.
- Focal/Grid: For specific DME (less common).
- Anti-VEGF Injections: (Ranibizumab, Aflibercept)
- First-line for center-involving DME. Reduces permeability.
- Adjunct for PDR.
- Intravitreal Steroids: (Dexamethasone implant) Refractory DME; pseudophakic.
- Pars Plana Vitrectomy (PPV):
- Non-clearing vitreous hemorrhage.
- Tractional RD involving macula.
- Laser Photocoagulation:
⭐ Pan-Retinal Photocoagulation (PRP) is the gold standard treatment for high-risk PDR.
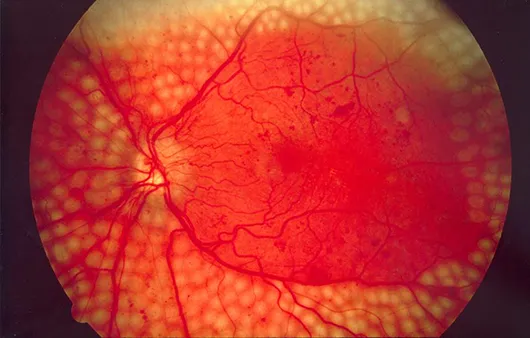
Screening & Prevention - Vision Vigilance Now
- Regular dilated fundus examination is paramount.
⭐ Annual dilated eye exam recommended for all diabetics: at diagnosis for Type 2 DM, and 5 years after diagnosis for Type 1 DM.
- Primary Prevention Pillars:
- Intensive glycemic control (Target HbA1c < 7%).
- Optimal blood pressure management (Target < 140/90 mmHg).
- Dyslipidemia correction.
- Counsel on early symptom recognition and treatment adherence.
High‑Yield Points - ⚡ Biggest Takeaways
- Diabetic Retinopathy (DR): leading cause of new blindness in working-age individuals.
- Duration of diabetes: most significant risk factor for DR development.
- Microaneurysms are the earliest sign of NPDR; also see hemorrhages, exudates, CWS.
- PDR is marked by neovascularization (NVD/NVE), risking vitreous hemorrhage and TRD.
- Macular Edema (CSME): can occur at any stage, primary cause of visual impairment.
- Pan-Retinal Photocoagulation (PRP): standard treatment for high-risk PDR.
- Anti-VEGF injections: vital for macular edema and adjunctive in PDR.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

