Traumatic Cataract: Etiology & Mechanisms - Eye's Impact Story
Traumatic cataract: lens opacification due to direct/indirect ocular injury.
- Etiology & Mechanisms:
-
Blunt Trauma: Most frequent.
- Mechanism: Coup-contrecoup, equatorial stretch (capsular/zonular tears), shock waves damaging fibers.
- Forms: Vossius ring (iris pigment on ant. capsule), Rosette/Stellate (classic, ant/post), localized subepithelial opacities.
-
Penetrating Trauma: Direct capsule perforation.
- Mechanism: Rapid lens fiber hydration & opacification.
- Often with Intraocular Foreign Body (IOFB). Focal cortical changes.
-
Other Causes:
- Electric shock: True ant. capsule exfoliation, diffuse punctate opacities.
- Radiation: Infrared (glassblower's - ant. capsular), Ionizing (PSC).
- Chemical injury (alkali more severe than acid).
-
⭐ Blunt trauma is a more common cause of traumatic cataract than penetrating trauma, often leading to characteristic Vossius ring or rosette cataracts.
Traumatic Cataract: Pathophysiology & Morphology - Lens Under Fire
-
Pathophysiology:
- Blunt Trauma (Concussion): Most common. Shock waves → lens fiber disruption, capsular micro-tears. Aqueous influx → fiber hydration, swelling → protein denaturation → opacification.
- Penetrating Trauma: Direct capsular breach → rapid hydration, opacification. Often associated with infection/foreign body.
- Other Causes: Electric shock, radiation, chemical injury.
-
Morphology:
- Concussion Cataract:
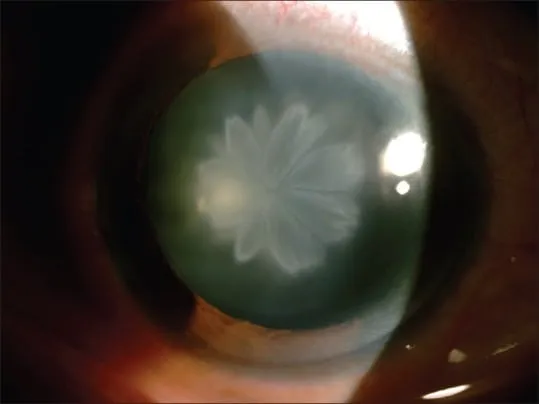
- Rosette/Stellate Cataract: Pathognomonic. Anterior/posterior subcapsular. Forms hours to days.
⭐ A classic rosette-shaped or stellate cataract is highly characteristic of concussional trauma and typically forms within hours to days post-injury.
- Vossius Ring: Iris pigment imprint on anterior capsule (not true cataract).
- Penetrating Cataract: Localized opacity at rupture; may rapidly mature.
- Electric Shock Cataract: Anterior subcapsular opacities, true capsular exfoliation.
- Radiation Cataract: Posterior subcapsular, delayed onset.
- Concussion Cataract:
Traumatic Cataract: Clinical Evaluation - Damage Assessment
- History: Mechanism: blunt, penetrating, chemical, radiation.
- Visual Acuity: Document Best Corrected Visual Acuity (BCVA).
- Slit-lamp Exam:
- Cornea: Wound, edema, foreign body (FB).
- Anterior Chamber: Depth, cells, flare, hyphema.
- Iris: Sphincter tears, iridodialysis, iridodonesis.
- Lens: Type (e.g., rosette, Vossius ring); capsular integrity (rupture); subluxation/dislocation (phacodonesis).
- Vitreous: Prolapse, hemorrhage.
- Intraocular Pressure (IOP): Check for glaucoma/hypotony.
- Fundoscopy (Dilated): Retina, choroid, optic nerve status.
⭐ A thorough ocular examination in traumatic cataract must include gonioscopy to detect angle recession, a risk factor for late-onset glaucoma.
- Investigations:
- B-scan: If poor posterior segment view.
- X-ray/CT: For suspected Intraocular Foreign Body (IOFB).

Traumatic Cataract: Management & Complications - Rescue & Repair
⭐ Early surgical intervention for traumatic cataract is indicated in cases of phacolytic glaucoma, phacomorphic glaucoma, or severe lens-induced uveitis.
-
Management Principles:
- Conservative: For small, non-progressive peripheral opacities. Includes observation, topical corticosteroids (inflammation control), cycloplegics (ciliary spasm, synechiae prevention).
- Surgical: For visually significant cataracts, lens-induced glaucoma (phacolytic/phacomorphic), severe uveitis, intumescent lens, phacoanaphylaxis.
- Techniques: Lens aspiration (children/young adults), phacoemulsification & IOL (primary/secondary). Pars plana lensectomy/vitrectomy for PCR/vitreous issues.
-
Management Flow:
- Potential Complications:
- Early: Persistent uveitis, secondary glaucoma (angle recession, pupillary block), hyphema, wound leak, endophthalmitis.
- Late: Posterior capsular opacification (PCO), IOL malposition, chronic uveitis, cystoid macular edema (CME), retinal detachment.
High‑Yield Points - ⚡ Biggest Takeaways
- Rosette-shaped cataract is a hallmark of blunt ocular trauma.
- Vossius ring (iris pigment on anterior capsule) signifies significant contusion injury.
- Etiologies include penetrating trauma, concussion, electric shock, and radiation.
- Surgical extraction with IOL implantation is the mainstay for visually significant cataracts.
- Crucial to assess for associated ocular injuries (e.g., angle recession, retinal detachment).
- Leaking lens proteins can induce phacolytic glaucoma, requiring prompt management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

