Introduction & Pathophysiology - Cloudy Comeback
- Posterior Capsular Opacification (PCO): Opacification of the posterior lens capsule post-cataract surgery.
- Commonly called "secondary cataract" or "after-cataract".
- Pathophysiology: Driven by residual Lens Epithelial Cells (LECs).
- 📌 Mnemonic: 'LECs PMM to cause PCO' (Proliferate, Migrate, Metaplase).
- LECs undergo:
- Proliferation: Increase in cell numbers.
- Migration: Movement from anterior capsule/equator to the posterior capsule.
- Metaplasia: Transformation of LECs.
- Fibrous metaplasia: LECs become myofibroblasts, depositing collagen, leading to capsular fibrosis.
- Key Types:
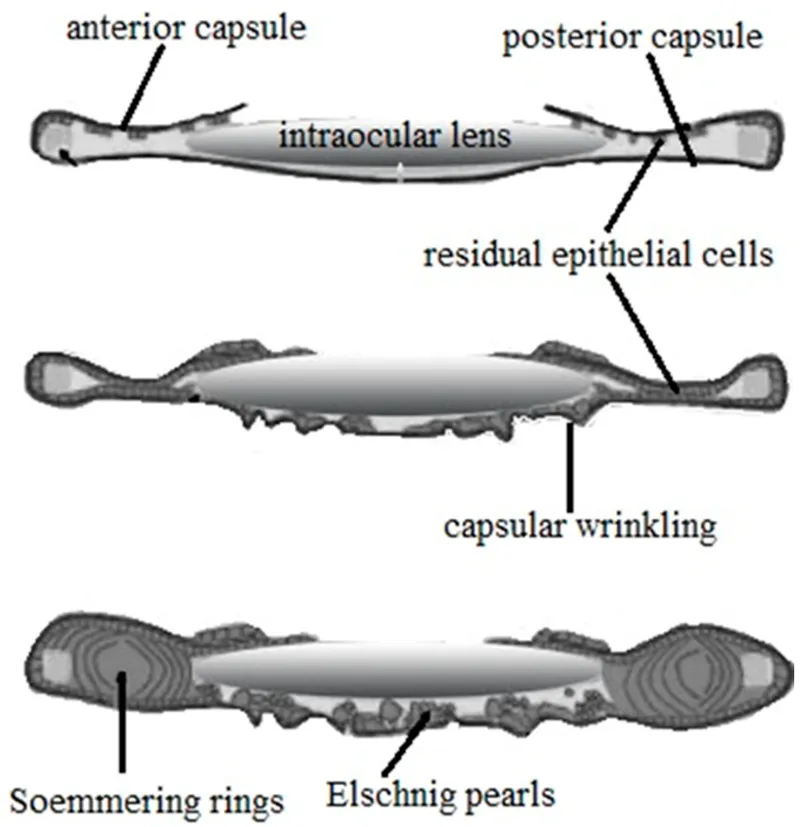
- Elschnig pearls: Proliferative type; clusters of swollen, vacuolated LECs.
- Capsular fibrosis: Fibrous type; due to myofibroblastic activity and collagen deposition, causing wrinkling/opacification.
⭐ PCO is the most common long-term complication of modern cataract surgery.
Clinical Features & Diagnosis - Hazy View Clues
Symptoms:
- Gradual, painless vision blurring.
- Glare/halos, esp. with night driving.
- ↓ Contrast sensitivity (difficulty in dim light).
- Monocular diplopia (ghost image).
Signs:
- ↓ Visual acuity (variable).
- Elschnig pearls: Grape-like clusters of swollen LECs on posterior capsule.
- Soemmering's ring: Peripheral doughnut opacity (retained cortex/LECs).
- Capsular fibrosis/wrinkles: Opacification/folds on posterior capsule.

Diagnosis:
- Slit-lamp exam: Key for diagnosis.
- Direct illumination: Shows opacities.
- Retroillumination: Best for pearls, fibrosis, wrinkles against red reflex.
⭐ Elschnig pearls, appearing as grape-like clusters of swollen LECs, are a characteristic sign of proliferative PCO.
Risk Factors & Prevention - Dodging the Fog
Risk Factors:
- Patient Factors:
- Younger age
- Ocular conditions: Uveitis, Diabetes, Pseudoexfoliation, Retinitis Pigmentosa
- Surgical & IOL Factors:
- Retained lens cortex
- Surgical trauma
- IOL characteristics (see table below)
IOL & PCO Risk:
| Feature | Higher PCO Risk | Lower PCO Risk |
|---|---|---|
| Material | PMMA, Silicone | Hydrophobic Acrylic |
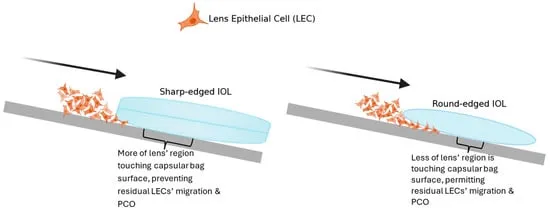
| Edge Design | Round | Sharp, Square |
- Surgical Technique:
- Meticulous cortical cleanup
- Complete hydrodissection (facilitates cleanup)
- In-the-bag IOL fixation (maintains barrier)
- Capsular polishing (removes more LECs)
- IOL Choice:
- Prefer Hydrophobic Acrylic material (biocompatible, less LEC adhesion)
- Ensure Sharp, Square-edged optic design (barrier effect)
⭐ A sharp, square-edged IOL optic design is the most crucial factor in preventing PCO by creating a mechanical barrier to Lens Epithelial Cell (LEC) migration.
Management - Laser Sharp Fix
Nd:YAG laser posterior capsulotomy is the standard treatment.
- Indications:
- Visually significant PCO (↓VA, glare).
- Impaired view of the fundus.
- Procedure:
- Energy levels: 0.8-1.5 mJ.
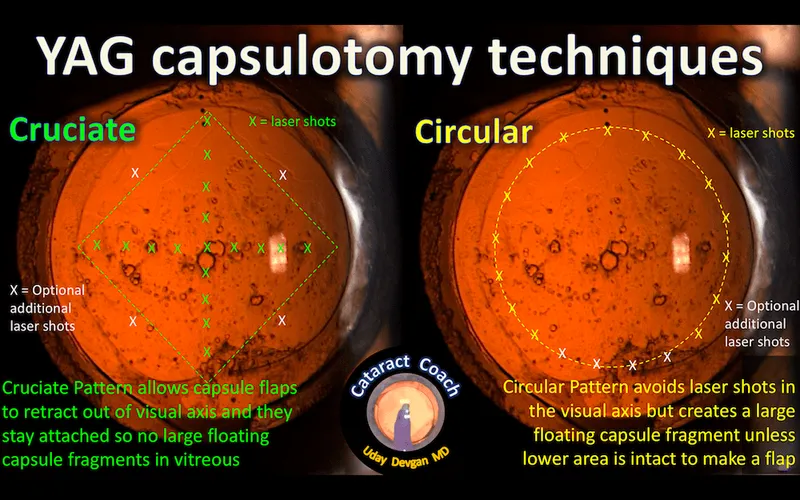
- Capsulotomy size: 3-4 mm (cruciate or circular pattern).
- Peri-operative Care:
- Pre-op: Apraclonidine or brimonidine (to ↓ risk of IOP spike).
- Post-op: Topical steroids and/or NSAIDs.
- Complications: 📌 Mnemonic: 'I-RACE My Lens'
- IOP spike (most common).
- Retinal detachment.
- Acute uveitis.
- Cystoid Macular Edema (CME).
- Endothelial damage/Corneal edema.
- My (IOL) Lens pitting/damage.
⭐ A transient rise in intraocular pressure is the most common complication immediately following Nd:YAG laser capsulotomy.
High‑Yield Points - ⚡ Biggest Takeaways
- Posterior Capsular Opacification (PCO) is the most common late complication of cataract surgery.
- Caused by proliferation and migration of residual lens epithelial cells (LECs).
- Key signs include Elschnig pearls (fish-egg appearance) and Soemmering's ring.
- Presents with gradual, painless blurring of vision, glare, and ↓contrast sensitivity, months to years post-op.
- Nd:YAG laser capsulotomy is the definitive treatment.
- Complications of YAG capsulotomy: ↑IOP, IOL pitting, cystoid macular edema (CME), and retinal detachment.
- Prevention strategies include square-edge design IOLs and meticulous cortical clean-up during surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

