IOL Basics & Materials - Lens Lowdown
- Function: Replaces natural lens; corrects aphakia, high refractive errors.
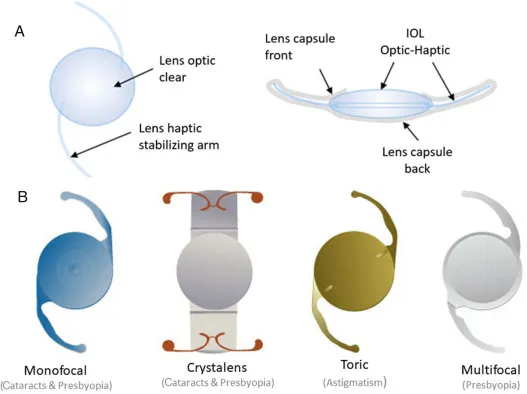
- Structure:
- Optic: Central refractive element.
- Haptics: Arms for fixation & centration within eye.
- Placement: Typically posterior chamber (in capsular bag).
IOL Materials Comparison:
| Material | Type | Key Features | Incision Size |
|---|---|---|---|
| PMMA | Rigid | Historical, excellent optics, biocompatible | ~5.5-7mm |
| Silicone | Foldable | Elastic, hydrophobic, potential for deposits | ~2.8-3.2mm |
| Hydrophilic Acrylic | Foldable | ↑Water (18-38%), good biocompatibility, risk of calcification | ~1.8-2.8mm |
| Hydrophobic Acrylic | Foldable | ↓Water (<1%), most used, ↓PCO, controlled unfolding | ~1.8-2.8mm |
IOL Types & Designs - Focus Features
- Monofocal: Single fixed focus (usually distance). Clear vision at one point; requires glasses for other distances.
- Multifocal (MFIOL): Multiple distinct foci (distance, intermediate, near). Aims for ↑ spectacle independence.
- Refractive: Zonal power variations.
- Diffractive: Light splitting design.
⭐ Diffractive multifocal IOLs commonly cause photic phenomena like glare and halos due to simultaneous focusing of light at multiple points.
- Extended Depth of Focus (EDOF): Creates an elongated focal range. Good intermediate vision; generally ↓ glare/halos vs. MFIOLs.
- Toric: Corrects corneal astigmatism. Available with monofocal, multifocal, or EDOF optics. Precise orientation vital.
- Accommodating: Attempts dynamic focus change, mimicking eye's natural lens. Limited, variable clinical results.
- Aspheric Design: Reduces spherical aberrations for improved contrast sensitivity. Common in modern IOLs.

IOL Power Calculation - Sizing Specs
- Biometry: Measures key eye parameters for IOL power.
- Axial Length (AL): Most critical for accuracy.
- Keratometry (K): Corneal power (average K).
- Anterior Chamber Depth (ACD): Effective lens position.
- SRK Formula (Basic): $P = A - 2.5L - 0.9K$
- $P$: IOL power (Diopters)
- $A$: A-constant (IOL model specific)
- $L$: Axial length (mm)
- $K$: Average keratometry (Diopters)
- A-constant: Manufacturer-provided; surgeon factor optimization improves accuracy.
⭐ A 1 mm error in axial length measurement typically results in approximately 2.5-3.0 Diopters of postoperative refractive surprise.
- Formula Selection by Axial Length (AL):
| AL Range (mm) | Recommended Formulas |
|---|---|
| < 22.0 | Hoffer Q, Holladay 2 |
| 22.0 - 24.5 | SRK/T, Holladay 1, Hoffer Q |
| > 24.5 - 26.0 | SRK/T, Holladay 1 |
| > 26.0 | SRK/T (Haigis preferred) |
IOL Complications - Glitch Gallery

- Early Complications:
- Toxic Anterior Segment Syndrome (TASS)
- Endophthalmitis (acute)
- IOL decentration/dislocation
- Corneal edema
- Wound leak
- ↑ Intraocular pressure (IOP)
- Cystoid Macular Edema (CME) (Irvine-Gass syndrome)
- Late Complications:
- Posterior Capsular Opacification (PCO) - most common
- IOL decentration/dislocation (late)
- UGH Syndrome (Uveitis-Glaucoma-Hyphema)
- Pseudophakic bullous keratopathy
- Chronic endophthalmitis
- Refractive surprise
⭐ Posterior Capsular Opacification (PCO), often called 'secondary cataract', is the most common late complication following cataract surgery with IOL implantation, treatable with Nd:YAG laser capsulotomy.
- Management: Varies by complication; e.g., Nd:YAG for PCO, IOL repositioning/exchange, topical steroids for inflammation, antibiotics for infection.
High‑Yield Points - ⚡ Biggest Takeaways
- PMMA is the standard material for non-foldable IOLs; foldable IOLs (acrylic, silicone) enable small incision surgery.
- The A-constant is a crucial lens-specific value for accurate IOL power calculation (e.g., SRK/T formula).
- Posterior Capsule Opacification (PCO) is the most common long-term complication after cataract surgery, treated with Nd:YAG laser capsulotomy.
- Multifocal IOLs offer a degree of spectacle independence but can be associated with visual phenomena like glare and halos.
- Toric IOLs are designed to correct pre-existing corneal astigmatism during cataract surgery.
- Anterior Chamber IOLs (ACIOLs) are utilized when there is insufficient capsular support for a posterior chamber lens implant.
- Biometry (axial length, keratometry) is essential for precise IOL power selection before surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

