ARC: Intro & Risks - Lens Clouding Culprits
- Age-Related Cataract (ARC): Gradual, progressive opacification (clouding) of the eye's crystalline lens.
- Leading cause of treatable blindness and ↓ vision in adults >60 years.
⭐ Age-related cataract is the leading cause of blindness worldwide and the most common cause of treatable blindness in India.
- Major Risk Factors:
- Age: Primary, non-modifiable factor.
- UV Radiation: Chronic exposure (especially UVB).
- Smoking: Oxidative stress.
- Diabetes Mellitus: Osmotic stress, earlier onset.
- Corticosteroids: Long-term systemic/topical use.
- Ocular Trauma.
- Genetics/Family History.
- Poor Nutrition: Low antioxidant intake.
- Excessive Alcohol.
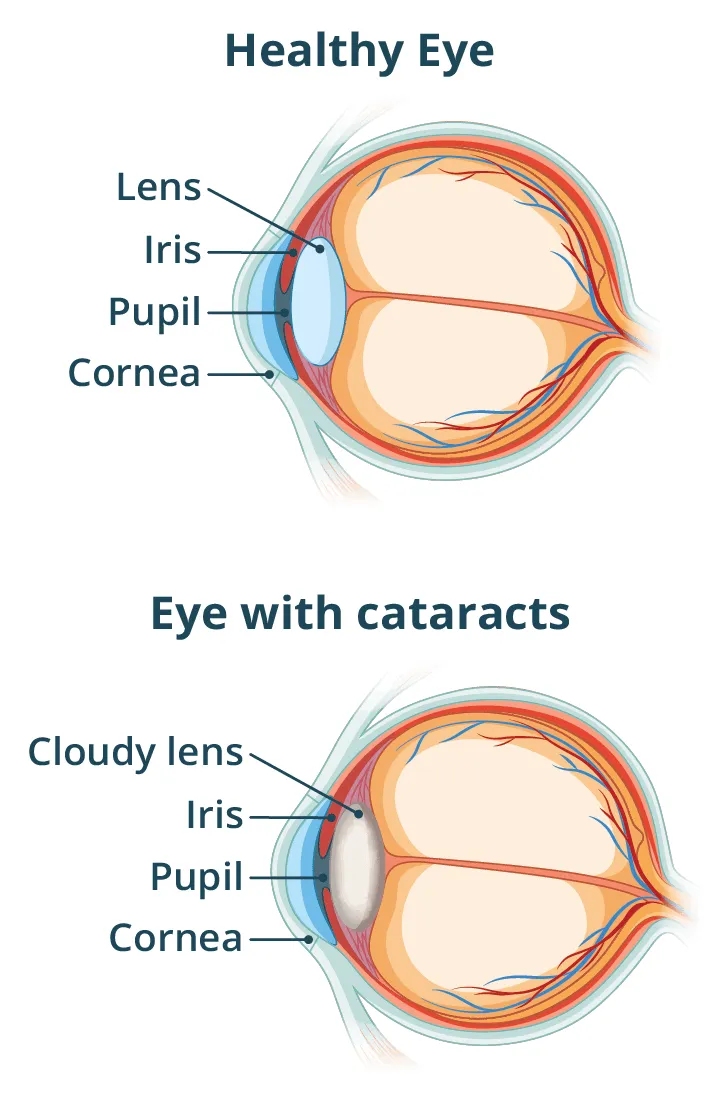
ARC: Pathophys & Types - Opacity Unveiled
Pathophysiology:
- Protein denaturation & aggregation (crystallins → insoluble albuminoids).
- Oxidative stress: ↑ Reactive Oxygen Species (ROS), ↓ glutathione.
- Electrolyte imbalance: ↑ Na⁺, Ca²⁺; ↓ K⁺.
- Non-enzymatic glycosylation.
Morphological Types:
- Nuclear Sclerosis (NS):
- Central, yellowish/brown opacity.
- Myopic shift ("second sight").
- Slow progression.
- Cortical Cataract (CC):
- Peripheral, radial spoke-like/cuneiform opacities.
- Glare.
- Stages: Incipient → Intumescent → Mature → Hypermature (Morgagnian).
- Posterior Subcapsular Cataract (PSC):
- Granular/plaque-like opacity on posterior capsule.
- Near vision ↓, glare ↑.
- Rapid progression.
⭐ Posterior Subcapsular Cataracts (PSC) cause disproportionate glare and difficulty with near vision, often progressing faster than other types.
- Christmas Tree Cataract: Polychromatic needle-like crystals.
ARC: Clinical & Diagnosis - Unmasking the Haze
- Symptoms:
- Painless, progressive ↓ vision (most common)
- Glare & halos (e.g., night driving difficulties)
- Difficulty reading fine print; needs ↑ illumination
- Altered color perception (blues appear faded/yellowish)
- Frequent changes in spectacle prescription
- Monocular diplopia (less common)
- Signs (Ocular Examination):
- ↓ Visual acuity (Snellen chart)
- Lens opacities visible on slit-lamp biomicroscopy & direct ophthalmoscopy
- Leukocoria (white pupillary reflex) in advanced/mature cataracts
- Diminished or altered red reflex (e.g., "oil droplet" sign in nuclear sclerosis)
- Diagnostic Workup:
- Comprehensive history taking
- Visual acuity assessment (distant & near)
- Slit-lamp examination (essential for type & grading)
- Ophthalmoscopy (direct & indirect) to view fundus
- Retinoscopy (may reveal "scissoring reflex")
⭐ The phenomenon of 'second sight' (myopic shift improving near vision temporarily due to increased refractive index of the lens nucleus) is characteristic of nuclear sclerosis.

ARC: Management & Complications - Restoring Sight Safely
- Management:
- Non-Surgical: Spectacles, improved lighting. Mydriatics (rarely).
- Surgical (Definitive):
- Indications: ↓VA (daily activities), phacolytic/morphic glaucoma, anisometropia.
- Pre-op: Biometry (IOL power calculation), B-scan (if opaque media).
- Techniques:
- Phacoemulsification + Foldable IOL: Preferred.
- Manual SICS + PMMA/Foldable IOL: For mature cataracts, high volume.
- ECCE: Largely historical.
- Surgical Steps Overview:
- Complications:
- Intraoperative: Posterior Capsular Rupture (PCR), dropped nucleus/IOL.
- Early Postoperative:
- Corneal edema, uveitis (TASS vs Endophthalmitis ⚠️).
- ↑IOP, wound leak.
- Late Postoperative:
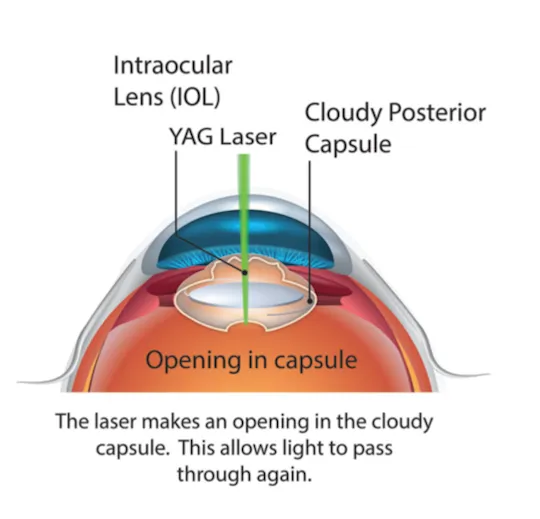
⭐ Posterior Capsular Opacification (PCO), also known as 'after-cataract', is the most common long-term complication following cataract surgery, treatable with YAG laser capsulotomy.
- Cystoid Macular Edema (CME - Irvine-Gass syndrome).
- IOL subluxation/dislocation, bullous keratopathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Age-related cataract: most common cause of reversible blindness worldwide.
- Presents with painless, progressive blurring of vision.
- Nuclear sclerosis (commonest) causes myopic shift ("second sight").
- Cortical cataracts cause glare and haloes, especially with night driving.
- Posterior subcapsular (PSC) affects near vision most, progresses rapidly.
- Major risk factors: age, diabetes, UV exposure, smoking, steroids.
- Treatment: phacoemulsification with IOL implantation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

