Introduction to Corneal Trauma - Eye's Shield Under Siege
The cornea, the eye's transparent "shield," is vital for vision and protection. Trauma to this structure is common and potentially sight-threatening.
-
Types of Corneal Injuries:
- Mechanical:
- Abrasions: Superficial epithelial defect.
- Lacerations: Partial/full-thickness (penetrating/perforating).
- Foreign Bodies: Superficial or intraocular.
- Blunt Trauma: Contusion, globe rupture.
- Non-Mechanical:
- Chemical Burns: Acid/Alkali (⚠️ Alkali more severe).
- Radiation Keratitis: e.g., UV exposure.
- Mechanical:
-
Common Patient Presentation:
- Severe pain, foreign body sensation.
- Photophobia, lacrimation.
- Blurred vision.
- Redness (circumciliary injection).
- History of trauma.
⭐ Alkali chemical burns penetrate deeper into ocular tissues via saponification, causing more extensive damage than acid burns.

Mechanical Corneal Injuries - When Things Go Bump (or Sharp!)
- Common Types:
- Corneal Abrasion: Superficial epithelial defect; intense pain.
- Foreign Body (FB): Superficial/embedded; rust ring if metallic.
- Laceration: Partial/full-thickness (penetrating/perforating).
- Key Symptoms: Sudden pain, photophobia, lacrimation, FB sensation, ↓vision.
- Essential Signs:
- Fluorescein staining: Highlights epithelial defects (abrasions, entry sites).
- Visible FB: On cornea or under lids (evert lids!).
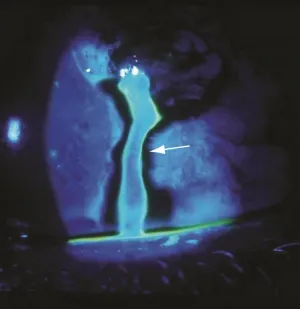
- Seidel's Test: Positive in perforation (aqueous leak dilutes fluorescein - "waterfall" sign).
- Other: Conjunctival injection, AC reaction, hyphema, irregular pupil.
- Management Principles:
- Abrasion: Topical antibiotics, cycloplegic, analgesia. Patching controversial.
- FB: Removal (needle/spud), rust ring removal (burr), antibiotics.
- Laceration: Shield eye (NO patch), urgent surgical repair.

⭐ A peaked pupil often points towards the site of a corneal perforation.
Chemical Corneal Burns - The Alkali-Acid Agony
- Alkali Burns (More Severe):
- Agents: Lime ($Ca(OH)_2$), $NaOH$, $NH_3$.
- Mechanism: Saponification, ↑penetration. Liquefactive necrosis.
- Prognosis: Worse. 📌 ALKALI is AWFUL.
- Acid Burns (Less Severe):
- Agents: $H_2SO_4$, $HCl$.
- Mechanism: Protein coagulation, ↓penetration. Coagulative necrosis.
- Exception: Hydrofluoric acid ($HF$) - acts like alkali.
- Clinical: Pain, ↓vision, corneal opacity, limbal ischemia (key prognostic factor).
- Grading (Roper-Hall): I-IV based on corneal clarity & limbal ischemia.
- Grade IV: Opaque cornea, >50% limbal ischemia.
- Management:
- Immediate: Copious irrigation (>30 mins with saline/water).
- Medical: Ascorbate, citrate, doxycycline, steroids (cautiously).
- Surgical: Amniotic Membrane Transplant (AMT), Limbal Stem Cell Transplant (LSCT).

⭐ Alkali burns cause liquefactive necrosis, leading to deeper penetration and more severe, progressive damage compared to the coagulative necrosis of most acid burns which tends to be self-limiting.
Diagnosis, Management & Complications - Patching Up the Pane
-
Diagnosis:
- History: Mechanism of injury (blunt, sharp, chemical, radiation).
- Slit-lamp examination: Vital for assessing depth, extent, foreign bodies.
- Fluorescein staining: Highlights epithelial defects (abrasions, ulcers).
- Seidel’s test: Detects aqueous leak (globe perforation).
- Imaging: B-scan (posterior segment), CT scan (intraocular foreign body, orbital fracture).
-
Management Principles:
- Remove foreign bodies.
- Topical antibiotics: Prophylaxis/treatment (e.g., Moxifloxacin).
- Cycloplegics: (e.g., Homatropine, Cyclopentolate) for pain relief, prevent synechiae.
- Pressure patching/Bandage contact lens: For large abrasions.
- Tetanus prophylaxis.
- Surgical repair: For full-thickness lacerations.
- Chemical burns: Copious irrigation (📌 LITMUS test first! Saline/Ringer's lactate).
- Complications:
- Infection (corneal ulcer, endophthalmitis).
- Corneal scarring, opacification.
- Irregular astigmatism.
- Traumatic cataract, glaucoma.
- Sympathetic ophthalmia (rare).
⭐ Seidel’s test is crucial for identifying full-thickness corneal lacerations by observing fluorescein dye dilution from leaking aqueous humor under cobalt blue light.
High‑Yield Points - ⚡ Biggest Takeaways
- Corneal abrasions: fluorescein stain positive; treat with topical antibiotics, cycloplegics.
- Seidel's test (streaming fluorescein) confirms corneal perforation.
- Penetrating injuries: rigid shield (no patch), systemic antibiotics, urgent referral.
- Chemical burns: copious, prolonged irrigation crucial; alkali burns more severe.
- Corneal foreign bodies: prompt removal, antibiotic cover; check for rust ring.
- Hyphema (blood in AC) often indicates significant blunt trauma.
- Suspect intraocular foreign body (IOFB) with high-velocity or penetrating trauma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

