Corneal Degenerations - Age & Wear Unveiled
Corneal degenerations are acquired, progressive, non-familial corneal changes, often age-related or secondary to local/systemic factors.
-
Key Differences: Degenerations vs. Dystrophies
Feature Corneal Degenerations Corneal Dystrophies Onset Later life (Age-related) Early life Laterality Often Unilateral/Asymmetric Usually Bilateral, Symmetric Inheritance Sporadic (Non-familial) Often Hereditary Inflammation May be present Usually Absent Vascularization Often Present Usually Absent Progression Variable Slow, Relentless -
Common Etiological Factors:
- Age (Senile changes)
- Chronic inflammation (e.g., keratitis, uveitis)
- Trauma (mechanical, chemical)
- Systemic diseases (e.g., gout, hypercalcemia)
- UV exposure
⭐ Corneal degenerations are typically acquired, often unilateral or asymmetric, and may be associated with vascularization, unlike most dystrophies.
Peripheral Problems - Thinning & Rings
-
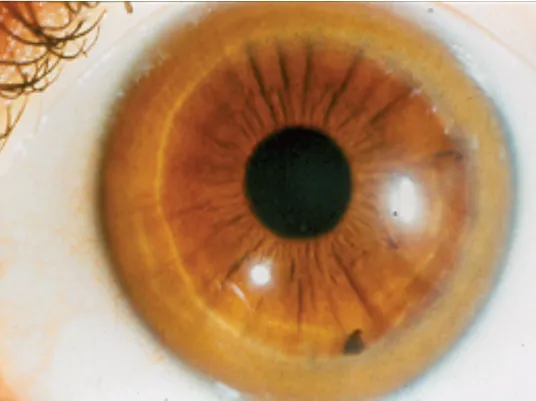
Arcus Senilis
-
Description: Common, bilateral, yellowish-white lipid deposition in peripheral corneal stroma, separated from limbus by a clear "lucid interval of Vogt".
-
Etiology: Usually age-related (>50 yrs). If present in individuals <40 yrs (Arcus Juvenilis), indicates likely hyperlipidemia.
-
Clinical Significance: Benign in elderly.
⭐ Arcus senilis in individuals <40 years (arcus juvenilis) warrants investigation for hyperlipidemia.
-
-
Terrien Marginal Degeneration (TMD)
- Description: Rare, idiopathic, painless, slowly progressive, non-inflammatory thinning of peripheral cornea. Typically bilateral, asymmetric, starting superonasally. 📌 Terrien = Thinning, Top (superiorly).

- Features: Intact epithelium over thinned area, lipid deposition at leading edge of thinning, superficial vascularization, characteristic against-the-rule astigmatism.
- Complications: Risk of spontaneous or traumatic globe perforation.
- Description: Rare, idiopathic, painless, slowly progressive, non-inflammatory thinning of peripheral cornea. Typically bilateral, asymmetric, starting superonasally. 📌 Terrien = Thinning, Top (superiorly).
Central & Surface Changes - Calcium & Nodules
-
Band Keratopathy: 📌 Bad Calcium.
-
Desc: Calcium deposition in Bowman's layer, typically in the interpalpebral fissure. Presents with a 'Swiss cheese' appearance (lucent holes within the band).
-
Etiol:
- Chronic ocular disease: Uveitis, phthisis bulbi.
- Systemic: Hypercalcemia, gout, sarcoidosis.
- Other: Intraocular silicone oil.
-
Sx: ↓ Vision, foreign body sensation (FBS), irritation.
-
Tx: Chelation with Ethylenediaminetetraacetic acid (EDTA).
⭐ Band keratopathy typically starts peripherally in the interpalpebral fissure and progresses centrally, with lucent holes within the band.
-
-
Salzmann Nodular Degeneration:
- Desc: Smooth, opaque, elevated bluish-white nodules, typically in the mid-periphery or periphery.
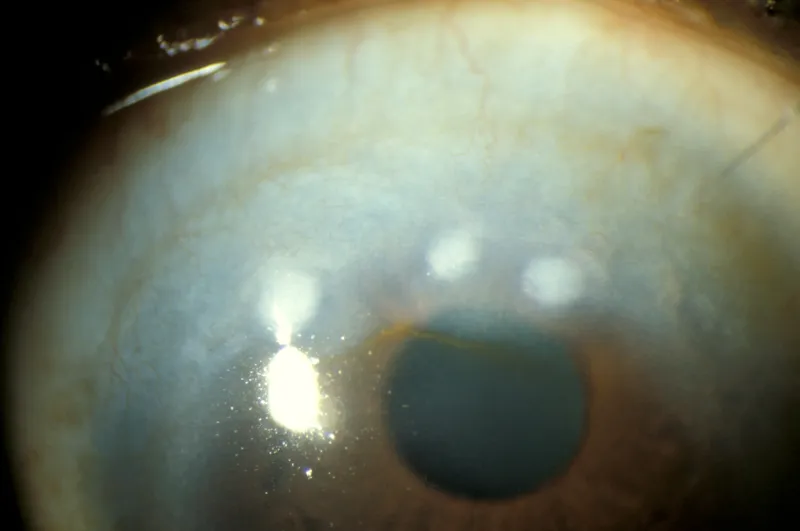
- Histo: Hyaline degeneration, disorganized lamellar collagen.
- Assoc: Chronic keratitis (e.g., phlyctenular, trachoma), trauma, prolonged contact lens wear. Strong female predilection.
- Desc: Smooth, opaque, elevated bluish-white nodules, typically in the mid-periphery or periphery.
-
Lipid Keratopathy:
- Desc: Dense, yellow-white, refractile lipid deposits within the corneal stroma.
- Types:
- Primary (idiopathic): Rare; occurs without prior corneal vascularization.
- Secondary: Common; develops following corneal vascularization from chronic irritation, injury, or herpetic keratitis.
High‑Yield Points - ⚡ Biggest Takeaways
- Arcus senilis: Commonest stromal lipid deposition, clear limbal zone; check lipids if < 40 yrs.
- Band Keratopathy: Interpalpebral calcium in Bowman's; linked to chronic uveitis, hypercalcemia.
- Salzmann's Nodular: Bluish-white hyaline nodules (post-chronic keratitis).
- Terrien's Marginal: Painless peripheral thinning, vascularized; risk of atraumatic perforation.
- Pellucid Marginal: Inferior crescentic thinning, "crab-claw" topo; high ATR astigmatism.
- Spheroidal Degeneration: Amber granules in stroma; linked to UV exposure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

