Corneal Layers & Structure - The Eye's Windshield
- Avascular, transparent; main refractive power.
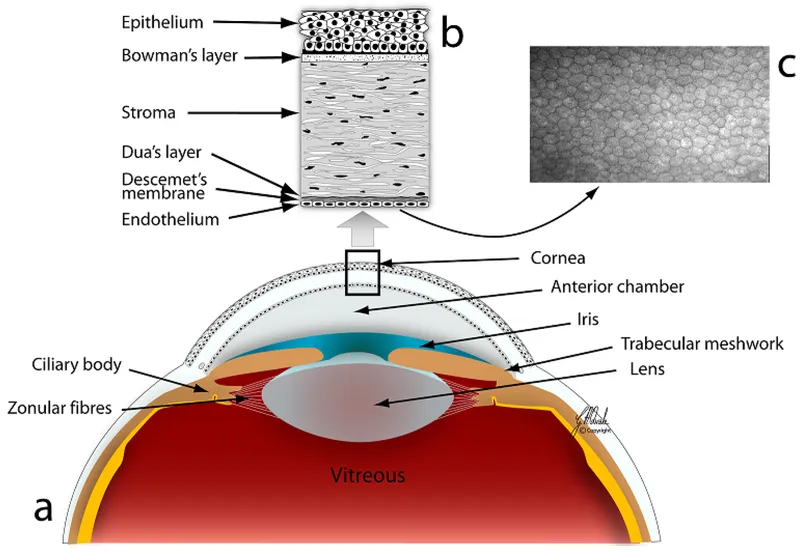
- Layers (Anterior → Posterior): 📌 Mnemonic: Every Brave Surgeon Discovers Deep Endothelium (Epithelium, Bowman's, Stroma, Dua's, Descemet's, Endothelium)
- Epithelium: Stratified squamous, non-keratinized. Regenerative. Barrier. (5-7 cells thick)
- Bowman's Layer: Acellular, Type I collagen. Resists injury. Non-regenerative (scars). (8-14 µm)
- Stroma: Type I collagen lamellae. Keratocytes. GAGs. Transparency. (~90% thickness, ~500 µm)
- Dua's Layer: Strong, acellular collagenous layer. (10-15 µm)
- Descemet's Membrane: Endothelial BM (Type IV collagen). Regenerates. Ends at Schwalbe's line. (3 µm → 10-12 µm with age)
- Endothelium: Single layer, hexagonal cells. Na+/K+ pump (deturgescence). Non-regenerative.
⭐ Endothelial density: ~2500 cells/mm² (adult). Min. for clarity: ~500-700 cells/mm².
 oka
oka
Corneal Histology & Cells - Cellular Scaffolding
- Epithelium: Stratified squamous cells (5-7 layers).
- Basal cells: Columnar, mitotic; anchored to basement membrane.
- Superficial cells: Flattened; tight junctions (zonula occludens) form protective barrier. Turnover: 7-14 days.
- Bowman's Layer: Acellular, dense connective tissue; primarily Type I collagen fibrils.
- Stroma (Cornea Proper): ~90% of corneal thickness.
- Keratocytes: Modified fibroblasts; synthesize collagen (Types I, V, VI), proteoglycans (PGs).
- Extracellular Matrix (ECM): Precisely arranged collagen lamellae & PGs (keratan sulfate, dermatan sulfate) maintain transparency.
- Descemet's Membrane: Posterior basement membrane of endothelium; primarily Type IV collagen.
- Endothelium: Single layer of hexagonal cells.
- Abundant Na+/K+ ATPase pumps maintain corneal deturgescence (relative dehydration).
- Limited regenerative capacity; cell density ↓ with age.
⭐ Normal adult endothelial cell density is 2500-3000 cells/mm²; corneal decompensation risk ↑ if < 500-700 cells/mm².
Corneal Transparency & Nutrition - Clearly Nourished
- Transparency Factors:
- Avascularity: Essential for optical clarity.
- Collagen: Regular fibril lattice (Maurice's theory); diameter
30 nm, spacing < wavelength of light (60 nm). Uniform refractive index. - Relative Dehydration (~78% water): Actively maintained by endothelial Na+/K+ ATPase pump (primary for deturgescence) & epithelial barrier (prevents tear influx).
- Smooth optical surface (precorneal tear film).
- Absence of myelinated nerves.
- Nutrition Sources:
- Aqueous Humor: Glucose, amino acids (main posterior supply).
- Tear Film: Oxygen (anteriorly; atmospheric O2 when eyes open, palpebral conjunctival vessels when closed), minor glucose.
- Limbal Capillaries: Peripheral cornea.
⭐ The corneal endothelium's Na+/K+ ATPase pumps drive its high metabolic activity, vital for transparency.
Corneal Innervation, Hydration & Metabolism - Wired & Water-Wise
- Innervation: Sensory via CN V1 (Ophthalmic div.) → Nasociliary n. → Long ciliary nerves. Rich, mostly unmyelinated. 📌 V1 for Vision's sensation.
- Hydration (Deturgescence): Maintains corneal clarity & 78% water content.
- Endothelial $Na^+/K^+$ ATPase pump (primary driver). Critical density: >500-700 cells/mm² to prevent edema.
- Epithelial barrier (tight junctions).
- Stromal GAGs: Imbibition pressure (draws water in, countered by pump).
- Metabolism: Avascular; relies on diffusion.
- Glucose (from aqueous, tears): Aerobic glycolysis (epithelium, endothelium); Anaerobic glycolysis (stroma, esp. under hypoxia e.g., contact lens wear).
- Pentose Phosphate Pathway (PPP): Produces NADPH for biosynthesis & protection against oxidative stress.
- O₂ Source: Atmosphere (open eye); Palpebral conjunctival vessels & aqueous humor (closed eye).
⭐ The endothelial $Na^+/K^+$ ATPase pump is the most critical component for maintaining corneal deturgescence and transparency.

High‑Yield Points - ⚡ Biggest Takeaways
- Cornea is avascular; nourished by aqueous, limbal vessels, and tear film.
- Five key layers: Epithelium, Bowman's layer, Stroma (90% thickness), Descemet's membrane, Endothelium.
- Sensory innervation via CN V1 (nasociliary branch); highly sensitive.
- Corneal transparency maintained by avascularity, regular stromal collagen, and endothelial pump (deturgescence).
- Primary refractive component of the eye (approx. +43 Diopters).
- Corneal endothelium (single layer) crucial for deturgescence; does not regenerate.
- Bowman's layer is acellular, non-regenerative, and scars upon injury.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

