Subconjunctival Hemorrhage - Bloody Eye Basics
Blood accumulation between conjunctiva and sclera. Anatomically limited posteriorly by Tenon's capsule fusion at limbus; does not cross the limbus.
- Etiology:
- Spontaneous (most common)
- Valsalva maneuver (coughing, sneezing, straining, vomiting)
- Trauma (direct ocular, head injury, barotrauma)
- Hypertension (sudden BP ↑)
- Bleeding disorders/Coagulopathy (e.g., hemophilia, liver disease, vitamin K deficiency)
- Anticoagulant/Antiplatelet medications (e.g., warfarin, aspirin, clopidogrel)
- Infections (viral conjunctivitis e.g., Adenovirus; Enterovirus 70 - Acute Hemorrhagic Conjunctivitis (AHC))
- Idiopathic
- 📌 Mnemonic - SCH CAUSES:
- S: Spontaneous/Strain
- C: Clotting issues/Coumadin
- H: Hypertension/Head trauma
⭐ Subconjunctival hemorrhage, though visually dramatic, is typically painless and does not affect vision.
Clinical Picture - Seeing Red Clearly
-
Symptoms: Often none!
- Patient notices red spot or told by others.
- Mild foreign body sensation or fullness possible.
- Crucially: NO pain, NO photophobia, NO vision loss, NO discharge (unless co-existing conjunctivitis).
-
Signs:
- Bright, flat, homogenous red area on sclera; sharply defined.
- Posterior edge usually visible (unless massive).
- Conjunctiva mobile over hemorrhage.
- Cornea: Clear.
- Pupil: Normal, reactive.
- Anterior Chamber: Quiet.
- Visual Acuity (VA): Normal.
- Intraocular Pressure (IOP): Normal.
⭐ The absence of pain and unchanged visual acuity are hallmark features distinguishing subconjunctival hemorrhage from more serious causes of acute red eye.
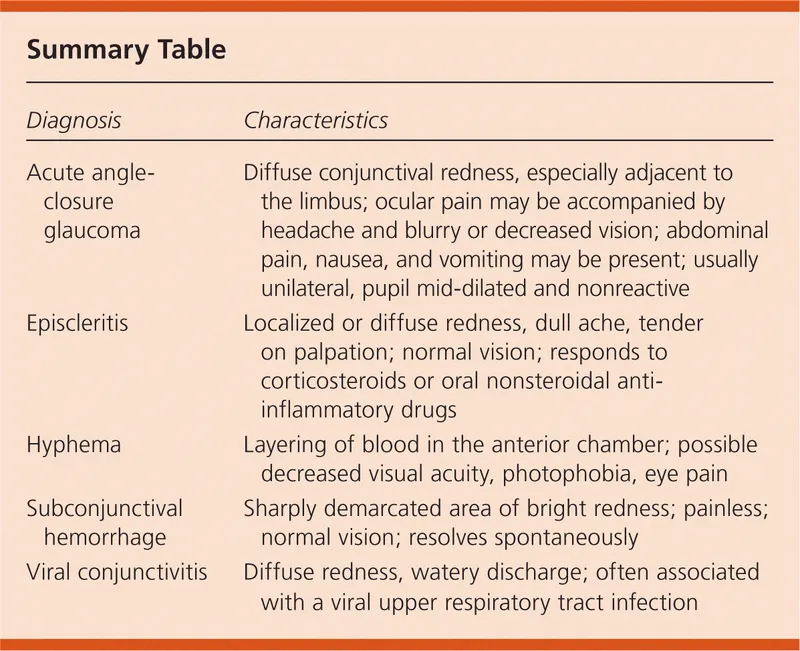
Red Eye Mimics - Spot The Difference
| Condition | Pain | Vision | Discharge | Photophobia | Ciliary Flush | IOP | Pupil |
|---|---|---|---|---|---|---|---|
| SCH | None | Normal | No | No | No | Normal | Normal |
| Acute Conj. | Gritty | Normal | Yes | Mild | No | Normal | Normal |
| Keratitis | Severe | ↓ | Watery | Severe | Yes | Normal | Miotic |
| Episcleritis | Mild | Normal | No | Mild | No (superficial, blanches) | Normal | Normal |
| Scleritis | Severe | ↓ | No | Yes | Yes (deep, no blanch) | Normal/↑ | Normal |
| AACG | Severe | ↓↓ | No | Yes (halos) | Yes | ↑↑↑ | Mid-dilated, Fixed |
| Hyphema | Variable | ↓ | Blood | Variable | Often | Often ↑ | Variable |
Treatment Plan - Calming The Crimson
- General Management:
- Reassurance: Benign, self-limiting.
- Conservative: Usually none needed.
- Artificial tears for mild irritation.
- Avoid Aspirin/NSAIDs if possible (unless medically necessary).
- Specific Management & When to Investigate:
- Hypertension: Check & manage BP.
- Anticoagulants: Check INR/PT; consult before stopping.
- Consider further investigation (CBC, PT/INR, PTT) or referral if:
- Recurrent or bilateral SCH.
- History of bleeding disorder.
- Significant ocular trauma (rule out globe rupture, retrobulbar hemorrhage).
- Associated systemic symptoms or diagnostic uncertainty.
- Prognosis:
- Excellent; resolves spontaneously in 1-3 weeks.
- Color changes: Red → orange → yellowish (like a bruise).
⭐ No specific treatment is usually required for subconjunctival hemorrhage; the primary intervention is reassurance and patient education about its benign nature and resolution time.
High‑Yield Points - ⚡ Biggest Takeaways
- Painless, bright red subconjunctival patch; vision is unaffected.
- Caused by ruptured conjunctival capillaries; often from Valsalva, minor trauma, or spontaneously.
- Key associations: hypertension, diabetes, bleeding disorders, anticoagulant use.
- Self-resolves typically within 1-2 weeks; no specific treatment needed.
- Reassurance is primary; investigate if recurrent, extensive, or with systemic signs.
- Absence of pain, visual loss, and discharge is characteristic.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

