Conjunctivitis: Viral - The Eye Invaders
- Common Causative Viruses:
- Adenovirus (most frequent)
- Herpes Simplex Virus (HSV)
- Varicella-Zoster Virus (VZV)
- Enterovirus
- Molluscum contagiosum virus
- Modes of Transmission:
- Direct contact with infected ocular secretions.
- Contaminated fomites (e.g., towels, makeup).
- Respiratory droplets (especially for Adenovirus).
- Pathophysiology: Viruses replicate within conjunctival and corneal epithelial cells, leading to cell lysis and a subsequent inflammatory response.
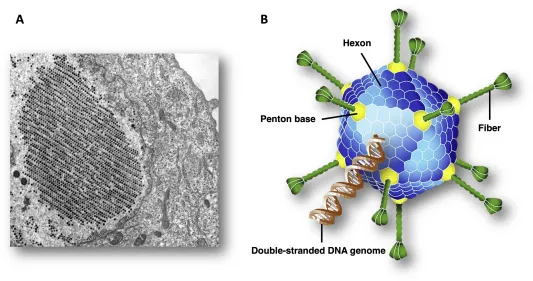
⭐ Adenovirus is responsible for 65-90% of all viral conjunctivitis cases, making it the predominant etiological agent globally for this condition.
Conjunctivitis: Viral - Spotting Red Flags
- Key Symptoms:
- Acute onset; typically unilateral, rapidly becoming bilateral.
- Profuse watery discharge (serous).
- Gritty/foreign body sensation, significant ocular redness (hyperemia), photophobia.
- Itching usually mild (distinguishes from allergic).
- Critical Signs:
-
Diffuse conjunctival hyperemia; chemosis (swelling).
-
Follicular reaction: Small, elevated, translucent lesions, especially on inferior palpebral conjunctiva.
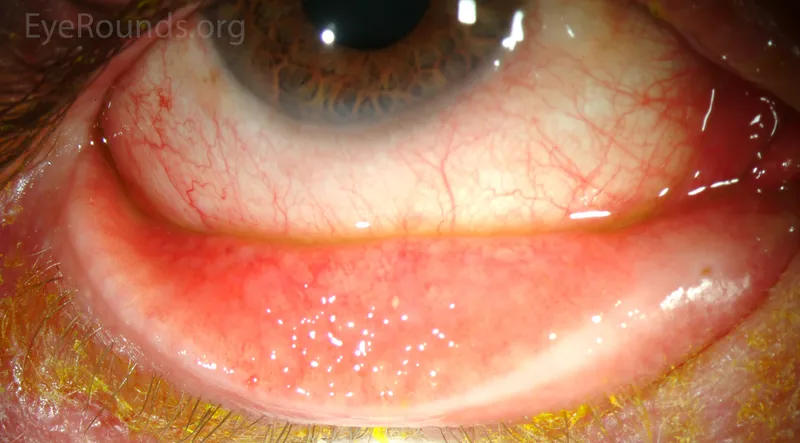
-
Tender preauricular lymphadenopathy: Hallmark sign. 📌 'A ViraL infection makes you PALe' (PreAuricular Lymphadenopathy).
-
Eyelid edema common. Severe cases (e.g., Epidemic Keratoconjunctivitis - EKC) may show petechial hemorrhages, pseudomembranes or true membranes.
-
⭐ The presence of tender preauricular lymphadenopathy is a strong indicator of viral conjunctivitis, particularly adenoviral.
Conjunctivitis: Viral - Identifying the Type
-
Pharyngoconjunctival Fever (PCF): Triad: fever, pharyngitis, bilateral follicular conjunctivitis. Adenovirus types 3, 4, 7. Common in children, swimming pool outbreaks.
-
Epidemic Keratoconjunctivitis (EKC): Highly contagious. Intense follicular conjunctivitis, pseudomembranes, characteristic subepithelial corneal infiltrates (SEIs) that can impair vision (vision ↓). Caused by Adenovirus types 8, 19, 37, 53, 54. Workplace/clinic outbreaks.
-
Acute Hemorrhagic Conjunctivitis (AHC): Rapid onset, dramatic subconjunctival hemorrhages, chemosis, watery discharge. Caused by Enterovirus 70 and Coxsackievirus A24. Highly contagious, epidemic prone.
-
Herpetic Conjunctivitis: Usually unilateral, associated with HSV keratitis (dendritic ulcer). Vesicular lesions on eyelids/margin. Follicular response. Reduced corneal sensation.
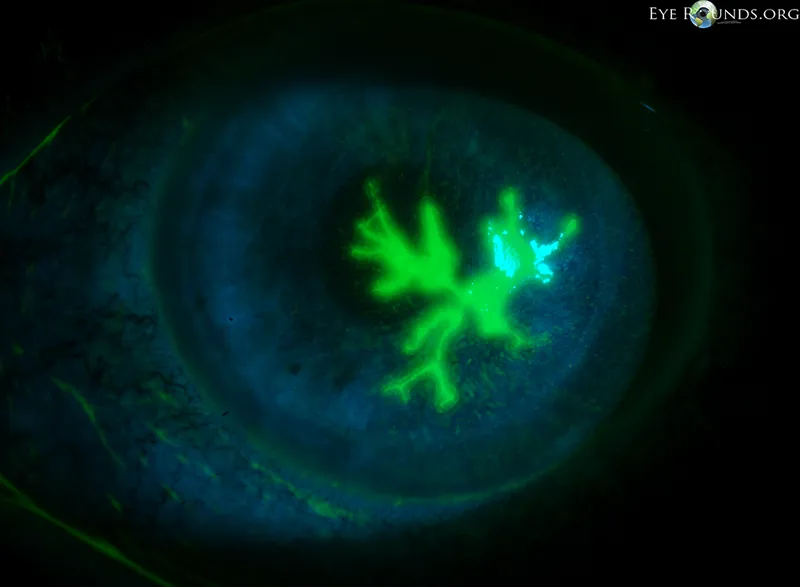
-
Diagnosis: Primarily clinical. Rapid antigen detection tests for Adenovirus (e.g., AdenoPlus) can confirm. Viral culture/PCR for atypical/severe cases or herpetic suspicion.
⭐ Subepithelial infiltrates (SEIs) in Epidemic Keratoconjunctivitis (EKC) can persist for weeks to months, causing glare and decreased vision even after acute infection resolves.
Conjunctivitis: Viral - Damage Control Plan
- General (Most Types):
- Supportive: PF artificial tears, cool compresses.
- Hygiene: Handwash, no sharing.
- Adenoviral (PCF, EKC):
- Self-limiting (1-3 weeks).
- Povidone-Iodine 0.8-1.0% wash.
- Severe (pseudomembranes, SEIs): Topical steroids (Loteprednol 0.5%), short course, taper. Rule out HSV.
⭐ The use of topical corticosteroids in adenoviral conjunctivitis is reserved for severe cases with pseudomembranes or symptomatic subepithelial infiltrates, and only after Herpes Simplex infection has been excluded.
- Herpetic Conjunctivitis:
- Topical antivirals: Ganciclovir 0.15% gel 5x/d, Trifluridine 1% gtts 9x/d.
- Oral acyclovir if extensive/recurrent.
- ⚠️ Topical steroids contraindicated: active HSV epithelial keratitis.
- AHC: Supportive, self-resolves.
- Prevention: Educate re: contagion, isolate EKC/AHC, disinfect instruments.
High‑Yield Points - ⚡ Biggest Takeaways
- Adenovirus is the most common cause of viral conjunctivitis.
- Key signs: acute onset, watery discharge, follicles, tender preauricular lymphadenopathy (PAL).
- EKC (Adenovirus 8, 19, 37) causes severe keratitis with subepithelial infiltrates (SEIs).
- PCF (Adenovirus 3, 4, 7) presents with fever, pharyngitis, and follicular conjunctivitis.
- Treatment is mainly supportive; topical steroids used cautiously for severe non-herpetic keratitis.
- Highly contagious; strict hand hygiene is vital to prevent spread.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

