Conjunctivitis: Bacterial - Red Eye Bugs
Acute bacterial inflammation of the conjunctiva. Presents with conjunctival injection ("red eye"), mucopurulent discharge (sticky lids, worse on waking), and foreign body sensation. Vision typically unaffected.
- Causative "Bugs":
- Adults: Staphylococcus aureus (most common), Streptococcus pneumoniae, Haemophilus influenzae.
- Children: Haemophilus influenzae, Streptococcus pneumoniae, Moraxella catarrhalis.
- Neonates (Ophthalmia Neonatorum):
- Neisseria gonorrhoeae: Hyperacute, copious pus, sight-threatening. Requires urgent systemic & topical Rx.
- Chlamydia trachomatis: Subacute, 1-2 weeks post-birth.
- 📌 Mnemonic: "Sticky eyes in the morning, think bacterial!"
⭐ Most common cause of bacterial conjunctivitis in adults is Staphylococcus aureus, while in children it's often Haemophilus influenzae or Streptococcus pneumoniae.
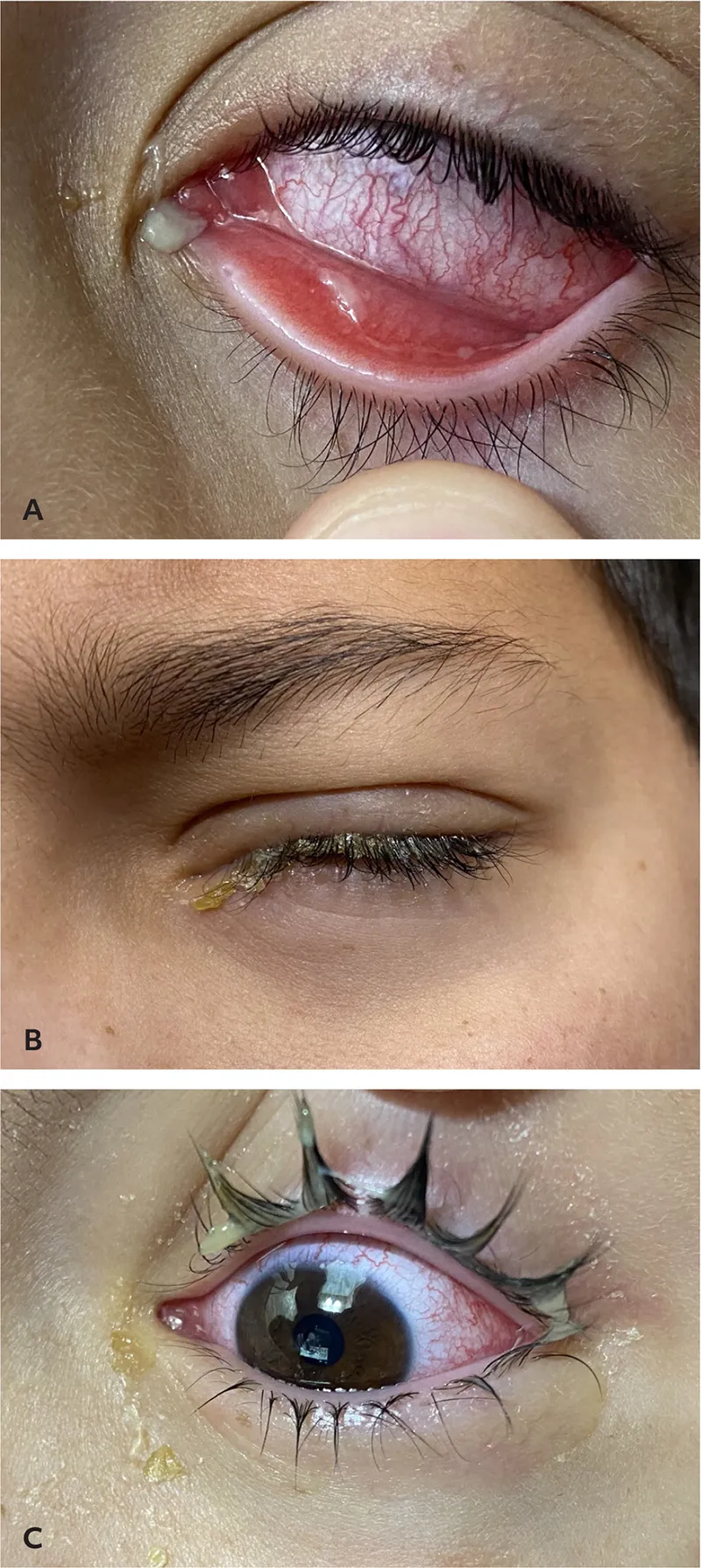
Conjunctivitis: Bacterial - Gooey Eye Clues
- Hallmark: Purulent/mucopurulent discharge ("gooey eye").
- Eyelids stuck, esp. on waking.
- Thick, yellow-green discharge.
- Onset: Acute.
- Laterality: Often bilateral; may start unilaterally.
- Symptoms:
- Beefy red conjunctival injection.
- Grittiness, FBS (Foreign Body Sensation).
- Mild discomfort (⚠️ severe pain = red flag).
- Vision normal (transient blur from discharge).
- Signs:
- Chemosis (conjunctival swelling).
- Papillary reaction (tarsal conjunctiva).
- Preauricular nodes usually absent (common in viral).
- Common Pathogens: S. aureus, Strep. pneumoniae, H. influenzae.
- Hyperacute (profuse discharge, medical emergency!): N. gonorrhoeae ⚠️.
⭐ Purulent or mucopurulent discharge with eyelids stuck together, especially upon waking, is highly characteristic of bacterial conjunctivitis.

Conjunctivitis: Bacterial - ID the Invader
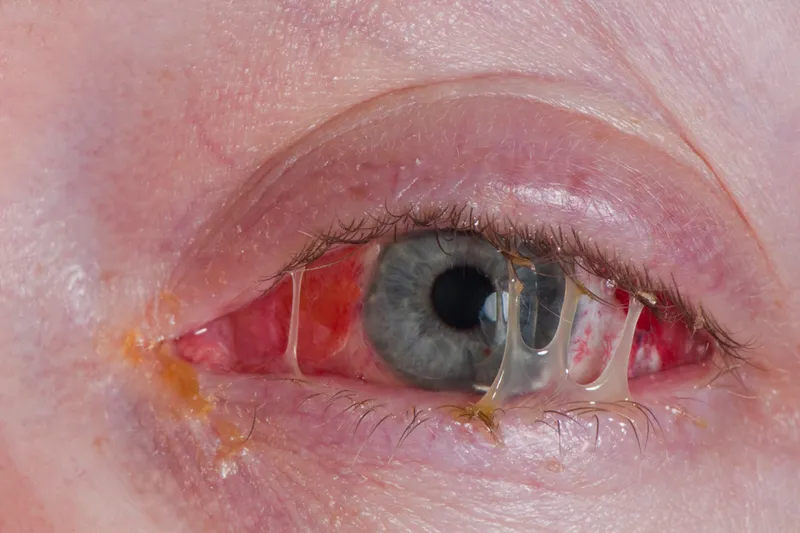
- Hallmarks: Acute onset, redness, irritation, purulent/mucopurulent discharge (yellow-green), lid matting (esp. morning).
- Transmission: Highly contagious; direct contact with secretions/fomites.
- Common Pathogens & Features:
- Staphylococcus aureus: Most frequent in adults; blepharitis common.
- Streptococcus pneumoniae: Children; often concurrent otitis media; petechial hemorrhages.
- Haemophilus influenzae: Children; often concurrent otitis media; URI prodrome.
- Moraxella catarrhalis: Can cause chronic angular blepharoconjunctivitis.
- Lab Investigations Decision:
⭐ Hyperacute conjunctivitis (e.g., N. gonorrhoeae) is an ophthalmic emergency requiring immediate Gram stain, culture, and systemic treatment to prevent corneal perforation.
Conjunctivitis: Bacterial - Banish Redness Fast
Goal: Eradicate infection, relieve symptoms, prevent spread & complications.
- Topical Antibiotics (First-line): Shorten course, ↓ transmission. Typical duration: 5-7 days.
- Fluoroquinolones (e.g., moxifloxacin, gatifloxacin).
- Polymyxin B/trimethoprim.
- Azithromycin (1% solution, BID for 2 days, then QD for 5 days).
- Tobramycin, Gentamicin.
- Chloramphenicol (caution: aplastic anemia).
- Systemic Antibiotics:
- Severe infections (e.g., N. gonorrhoeae - Ceftriaxone 1g IM single dose).
- Chlamydial conjunctivitis (Azithromycin 1g oral single dose).
- Associated systemic illness (e.g., otitis media).
- Adjunctive Therapy:
- Warm compresses.
- Lid hygiene.
- Frequent handwashing.
- Avoid sharing fomites.
⭐ Most cases of acute bacterial conjunctivitis are self-limiting, but topical antibiotics (e.g., fluoroquinolones, polymyxin B/trimethoprim) shorten the clinical course and reduce transmission.
High‑Yield Points - ⚡ Biggest Takeaways
- Common bacterial causes: Staphylococcus aureus, Streptococcus pneumoniae, Haemophilus influenzae.
- Key signs: Mucopurulent discharge, eyelids stuck together (especially in morning), often bilateral.
- Hyperacute conjunctivitis: Caused by Neisseria gonorrhoeae, presents with copious purulent discharge, an ophthalmic emergency.
- Ophthalmia Neonatorum: N. gonorrhoeae (days 2-5), Chlamydia trachomatis (days 5-14).
- Treatment: Primarily broad-spectrum topical antibiotics (e.g., fluoroquinolones, moxifloxacin).
- Systemic antibiotics are crucial for gonococcal and chlamydial infections.
- Highly contagious: Emphasize hand hygiene to prevent transmission and autoinoculation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

