Allergic Conjunctivitis: Overview & Types - Itchy Eye Intro
Inflammation of conjunctiva due to Type I hypersensitivity to allergens (pollen, dust mites, dander).
- Types & Key Features:
- Seasonal (SAC): Acute, recurrent; pollen.
- Perennial (PAC): Chronic, milder; dust mites, dander.
- Vernal Keratoconjunctivitis (VKC): Severe, young males, warm climates; cobblestone papillae, Trantas dots.
- Atopic Keratoconjunctivitis (AKC): Chronic, with atopic dermatitis; severe, potential corneal scarring.
- Giant Papillary Conjunctivitis (GPC): Contact lens wear, ocular prostheses, sutures; large papillae on upper tarsal conjunctiva.
⭐ Itching is the hallmark and most consistent symptom of allergic conjunctivitis.
Allergic Conjunctivitis: Pathophysiology - Allergy Cascade
A Type I (IgE-mediated) hypersensitivity. Allergen re-exposure triggers IgE-coated mast cell degranulation.
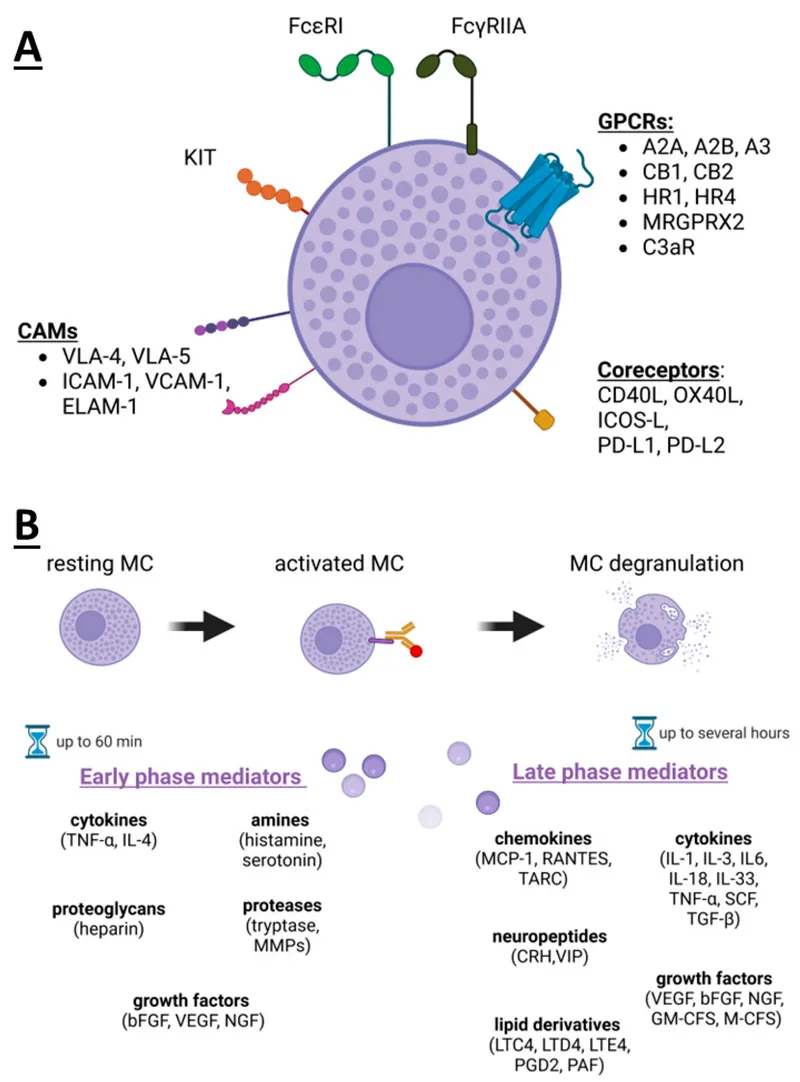
- Early Phase (minutes post-exposure):
- Mediators: Histamine, proteases (pre-formed).
- Effects: Itching, redness (vasodilation), chemosis (↑permeability).
- Late Phase (4-24 hours post-exposure):
- Mediators: Leukotrienes, Prostaglandins, cytokines (newly synthesized).
- Cellular Influx: Eosinophils, neutrophils.
- Effects: Sustained inflammation, potential for chronic changes.
⭐ Allergic conjunctivitis is primarily a Type I (IgE-mediated) hypersensitivity reaction involving mast cell degranulation.
Allergic Conjunctivitis: Clinical Features - Red & Raging
- Symptoms: Itching (pruritus) is the hallmark. Accompanied by redness, watering (epiphora), stringy/mucoid discharge, photophobia, and foreign body sensation.
- Common Signs: Conjunctival hyperemia (redness), chemosis (swelling), eyelid edema. Papillary hypertrophy is the characteristic sign.
Key Distinguishing Features by Type:
| Type | Papillae (Location) | Limbal | Cornea | Other Key Features |
|---|---|---|---|---|
| VKC | Cobblestone (upper tarsus) | Horner-Trantas dots | Shield ulcer | Young males, seasonal peak |
| AKC | Fine/Giant (lower > upper tarsus) | +/- | Keratitis, Neovasc. | Atopy, Dennie-Morgan lines |
| SAC/PAC | Small, diffuse | None | Rare | Acute/Chronic seasonal/perennial |
| GPC | Giant (upper tarsus) | None | Rare | Contact lens/suture-induced |

⭐ Horner-Trantas dots, which are collections of eosinophils at the limbus, are characteristic of Vernal Keratoconjunctivitis (VKC).
Allergic Conjunctivitis: Diagnosis - Spotting the Allergy
- Clinical Diagnosis: Primarily based on:
- History: Atopy, seasonal pattern, allergen exposure.
- Typical signs/symptoms: Bilateral itching (key), redness, watery discharge, chemosis.
- Investigations (Usually not required for simple cases):
- Conjunctival scraping: For eosinophils.
- Serum IgE levels: May be elevated (non-specific).
- Skin prick tests: To identify specific allergens.
- Differential Diagnosis:
- Viral conjunctivitis.
- Bacterial conjunctivitis.
- Dry eye syndrome.
- Toxic/Chemical conjunctivitis.
⭐ The presence of eosinophils in conjunctival scrapings supports the diagnosis of allergic conjunctivitis, especially in severe forms like Vernal Keratoconjunctivitis (VKC) or Atopic Keratoconjunctivitis (AKC).
Allergic Conjunctivitis: Management - Soothing the Storm
- Non-Pharmacological:
- Allergen avoidance
- Cold compresses
- Artificial tears (preservative-free)
- Pharmacological:
- Systemic Therapy:
- Systemic antihistamines for systemic allergy (as needed).
⭐ Dual-acting topical agents (antihistamine + mast cell stabilizer) like olopatadine are often first-line pharmacological treatment for allergic conjunctivitis due to rapid relief and sustained action.
High‑Yield Points - ⚡ Biggest Takeaways
- Primarily a Type I hypersensitivity reaction, leading to intense itching (pruritus).
- Characteristic signs include conjunctival papillae (cobblestone in VKC), chemosis, and watery/mucoid discharge.
- Eosinophils are typically found in conjunctival scrapings, especially in VKC.
- Vernal Keratoconjunctivitis (VKC) is a severe, chronic form, common in young males in warm, dry climates.
- Management involves topical antihistamines, mast cell stabilizers; topical steroids for severe/refractory cases.
- Often associated with a personal or family history of atopy (e.g., asthma, eczema).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

