Conjunctival Trauma: Introduction & Types - Eye's First Shield
Conjunctival trauma involves injury to the conjunctiva, the eye's vital, transparent outer membrane. It acts as the first line of defense.
- Key Conjunctival Roles:
- Protection: Shields underlying ocular structures from external insults.
- Lubrication: Secretes mucin, contributing to tear film stability and ensuring smooth eyelid movement.
- Immune Response: Contains Conjunctiva-Associated Lymphoid Tissue (CALT) for local immunity.

- Types of Conjunctival Trauma:
- Mechanical: e.g., foreign body, abrasion, laceration.
- Chemical: Caused by acids or alkalis (chemical burns).
- Thermal: Burns from extreme heat or cold.
- Radiation: Damage from UV light or ionizing radiation.
⭐ Conjunctiva's rich vascular supply leads to prominent subconjunctival hemorrhage but also facilitates rapid healing due to good blood flow.
Conjunctival Trauma: Mechanical Injuries - Scrapes, Tears, Bits
- Abrasions: Epithelial defect. Stains with fluorescein.
- Lacerations:
- Superficial or deep.
- Assess for scleral/corneal involvement.
- Seidel test if perforation suspected.
- Suture if > 1-1.5 cm or Tenon's capsule involved.
- Foreign Bodies (FB):
- Superficial, embedded, or sub-tarsal (under eyelid).
- Removal techniques vary; irrigation, cotton swab, or needle.
- 📌 Double eversion crucial for superior fornix FBs.
⭐ Always perform double eversion of the upper eyelid to rule out foreign bodies lodged in the superior fornix, especially with linear corneal abrasions.
- Subconjunctival Hemorrhage:
- Causes: Trauma, Valsalva, hypertension, idiopathic.
- Appearance: Bright red blood under conjunctiva.
- Management: Reassurance, artificial tears; resolves spontaneously.


Conjunctival Trauma: Chemical Burns - Splash Zone Peril
| Feature | Acid Burns | Alkali Burns (📌 ALKALI = ALL BAD) |
|---|---|---|
| Mechanism | Coagulation necrosis, eschar | Saponification |
| Penetration | Limited | Deeper, more severe |
| Agents | Battery acid, industrial cleaners | Lime (CaO), ammonia (NH₃) |
| Prognosis | Generally better | Generally worse |
- Irrigate: Normal saline/Ringer's lactate, ~30 min or 2-3L until pH $7.0-7.4$.
- Grading: Roper-Hall/Dua (limbal ischemia > 180° = poor prognosis).
- Medical: Topical steroids, antibiotics, cycloplegics, oral Vit C 1-2g/day, lubricants, ?amniotic membrane.

⭐ The single most important step in managing chemical eye injury is immediate, copious, and prolonged irrigation.
Conjunctival Trauma: Thermal & Radiation - Heat & Zap
- Thermal Burns:
- Causes: Flash, flame, contact (e.g., curling iron, hot liquids).
- Features: Pain, conjunctival injection, chemosis, epithelial defects.
- UV Kerato-conjunctivitis (Welder's Arc, Snow Blindness):
- Symptoms delayed: 6-12 hrs post-exposure.
- Features: Severe bilateral pain, photophobia, foreign body sensation (FBS), diffuse punctate epithelial erosions.
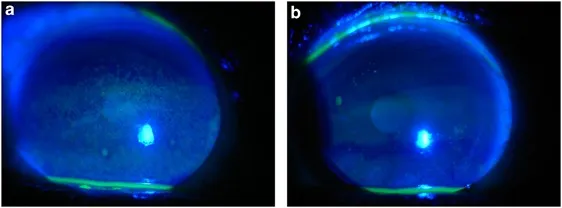
⭐ Welder's arc flash (UV kerato-conjunctivitis) is characterized by a latent period of several hours (6-12 hrs) followed by intense bilateral eye pain, photophobia, and foreign body sensation.
- Radiation Injuries (Ionizing - Radiotherapy):
- Delayed effects: Dry eye, keratinization, telangiectasia.
- General Management:
- Lubrication (artificial tears), topical antibiotics.
- Cycloplegics (for pain), NSAIDs (oral/topical).
- Cool compresses; patching for comfort in UV burns (short-term).
Conjunctival Trauma: Complications & Management - Patch & Protect
- General Principles: Pain relief, infection prevention (topical antibiotics), promote healing, tetanus prophylaxis if indicated.
- Early Complications: Infection, persistent epithelial defect, corneal involvement.
- Key Complications & Management:
| Complication | Key Prevention/Management |
|---|---|
| Infection | Topical antibiotics, debridement |
| Persistent Epithelial Defect | Lubrication, bandage contact lens, amniotic membrane |
| Symblepharon | Symblepharon ring, amniotic membrane, surgical release |
| Xerosis (Dry Eye) | Artificial tears, punctal occlusion |
| Conjunctival Scarring | Mitomycin C, amniotic membrane, mucous membrane graft |
⭐ Symblepharon formation, an adhesion between palpebral and bulbar conjunctiva, is a dreaded complication of severe chemical burns and Stevens-Johnson syndrome, often requiring surgical intervention.
High‑Yield Points - ⚡ Biggest Takeaways
- Subconjunctival hemorrhage (SCH): Common, painless, resolves spontaneously; check BP if recurrent.
- Conjunctival lacerations: Assess for globe perforation (Seidel's); suture if >1 cm or gaping.
- Foreign bodies: Evert eyelids (especially superior fornix); remove with irrigation/swab.
- Chemical injuries: Immediate copious irrigation is critical; alkali burns are worse.
- Symblepharon: Late adhesion, a serious complication of severe trauma/burns.
- Always suspect deeper injuries: corneal abrasion, IOFB, ruptured globe.
- Chemosis (edema) is a common sign_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

