Specialty Contact Lenses - Vaulting Champions
- Indications: 📌 SKOPE: Severe Dry Eye Disease (DED), Keratoconus/Corneal ectasia, Ocular surface protection (e.g., Stevens-Johnson Syndrome), Post-surgical (e.g., corneal graft), Extreme refractive errors.
- Types: Mini-scleral (15-18mm), large/full scleral (>18mm).
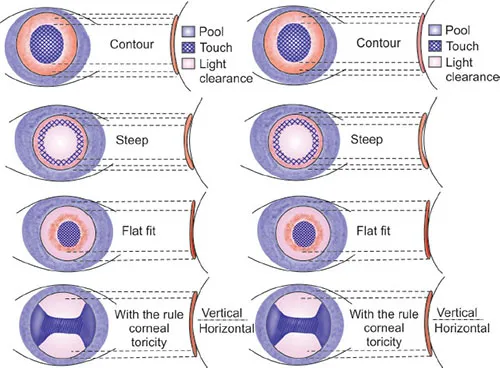
- Fitting Principles:
- Apical (central corneal) vault: typically 200-400 µm.
- Limbal clearance: 50-100 µm.
- Scleral landing zone: even alignment, no impingement.
- Material Properties: High $Dk$ for optimal oxygen permeability.
- Advantages: Stable, clear vision; enhanced comfort; therapeutic tear reservoir.
- Potential Complications: Midday fogging, conjunctival prolapse/hyperemia, suction on removal, handling difficulties.

⭐ Scleral lenses are particularly beneficial for severe keratoconus and ocular surface diseases due to the creation of a pre-corneal fluid reservoir.
Specialty Contact Lenses - Myopia Night Guards
- Mechanism (Ortho-K): Overnight RGP lenses reshape cornea: central epithelial thinning, mid-peripheral thickening.
- Indications: Myopia control (children); temporary myopia (≤ -6.00D), astigmatism (≤ -1.75D).
- Lens Design: Reverse geometry, multiple zones.
- Fitting: Bull's-eye fluorescein pattern, good centration. Post-wear topography: central flattening.
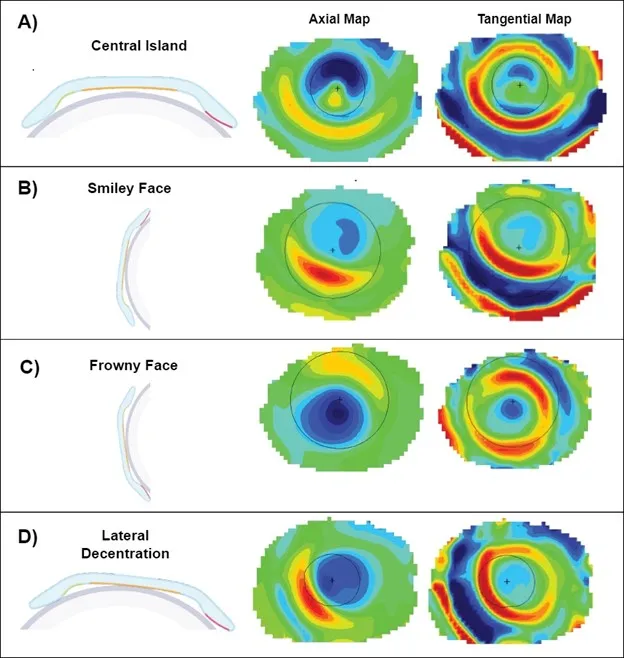
- Materials: High Dk (e.g., Tisilfocon A, Roflufocon D/E) for overnight wear.
- Benefits: Spectacle-free daytime.
- Risks: ⚠️ Microbial keratitis, corneal staining, decentration.
- 📌 Mnemonic: Ortho-K C.A.R.E.S.: Children, Active lifestyle, Refractive stability, Eye health, Slows myopia.
⭐ Ortho-K: central flattening & mid-peripheral steepening creates peripheral myopic defocus, slowing axial elongation in children.
Specialty Contact Lenses - Healing & Hiding
- Therapeutic (Bandage) Lenses: Aid corneal healing.
- Goals: Pain relief, promote re-epithelialization, mechanical protection.
- Materials: High $Dk/t$ silicone hydrogel (extended wear approved).
- Prosthetic Lenses: Address functional/cosmetic defects.
- Goals: Improve cosmesis, ↓ photophobia, occlude pupil.
- Types: Translucent tinted, opaque printed/painted.
Indications Comparison:
| Therapeutic | Prosthetic |
|---|---|
| Corneal abrasions/erosions, bullous keratopathy, post-surgical (PRK/CXL), filamentary keratitis, chemical burns. | Aniridia, iris coloboma, traumatic mydriasis, corneal opacities/leucoma, albinism, intractable diplopia. |
Specialty Contact Lenses - Irregularity Tamers
- Specialty RGPs: For irregular corneas.
- Indications: Keratoconus, Pellucid Marginal Degeneration (PMD), post-keratoplasty, post-refractive ectasia.
- Designs: Rose K2, KCG, Dyna Intra-Limbal; PMD designs: ↑ inferior edge lift.
- Fitting: Apical clearance/light feather touch, good peripheral alignment.
- Hybrid Lenses: RGP optics, soft lens comfort.
- Structure: Central RGP, peripheral soft skirt.
- Indications: RGP optics with soft comfort, irregular corneas, RGP intolerance.
- Pros: RGP vision, soft comfort, stability.
- Cons: ↑ Cost, complex care, skirt tightening, debris trapping.
⭐ Rose K lenses for keratoconus feature complex geometry (multiple posterior peripheral curves, aspheric optic zones) for better conformity to irregular corneas.
High‑Yield Points - ⚡ Biggest Takeaways
- Scleral lenses: For keratoconus, severe dry eye, irregular astigmatism; vault cornea, create tear reservoir.
- Orthokeratology (Ortho-K): For myopia control; overnight corneal reshaping for temporary myopia reduction.
- Hybrid lenses: RGP center (optics) + soft skirt (comfort); for keratoconus, post-surgery.
- Prosthetic lenses: Improve cosmesis in aniridia, albinism, corneal opacities.
- Bandage contact lenses (BCL): Promote corneal healing, pain relief, barrier function.
- Rose K lenses: Popular RGP design specifically for keratoconus management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

