SCL Materials & Properties - Material Marvels
- Materials:
- Hydrogels (e.g., HEMA): O₂ via water.
- SiHy (Silicone Hydrogels; e.g., Lotrafilcon): O₂ via silicone. Higher Dk.
- Key Properties:
- $Dk$ (Oxygen Permeability): Material's O₂ capacity.
- $Dk/t$ (Oxygen Transmissibility): $Dk$/thickness. Corneal health.
- Daily Wear (DW): $Dk/t > \textbf{24} \times 10^{-9}$ (📌 Daily 24)
- Extended Wear (EW): $Dk/t > \textbf{87} \times 10^{-9}$ (📌 Extended 87)
- WC% (Water Content): Hydrogels: ↑WC → ↑Dk. SiHy: Dk less WC-dependent.
- Modulus: Stiffness. ↑Modulus → handling ease, ↓comfort.
- Wettability & Deposit Resistance.
| Property | Hydrogel | SiHy |
|---|---|---|
| Dk | Lower (WC ↑ → Dk ↑) | Higher (Silicone) |
| WC (%) | 38-75 (Higher) | 24-48 (Variable) |
| Modulus | Lower (Softer) | Higher (Stiffer) |
| O₂ Path | Water | Silicone |
⭐ Holden-Mertz: $Dk/t > \textbf{24} \times 10^{-9}$ (DW), $Dk/t > \textbf{87} \times 10^{-9}$ (EW) to prevent corneal edema.
SCL Types & Modalities - Lens Lineup
-
Key SCL Categories:
Modality / Schedule Daily Disposable (DD) Reusable (Bi-weekly/Monthly) Extended Wear (EW) Wear Time Single day use Daily wear, regular cleaning EW: Up to 30 nights (SiHy approved) Replacement Daily 2 weeks / 1 month Per lens type (e.g., monthly for some EW) Pros ↑Hygiene, convenience Cost-effective (lens) Max convenience Cons ↑Cost (annual) Cleaning regimen, deposit risk ↑Hypoxia, ↑Infection risk Common Specialty Lens Availability Toric, Multifocal Toric, Multifocal, Custom Toric, Multifocal
⭐ Extended wear SCLs, especially older generation high water content ionic lenses, carry a significantly higher risk of microbial keratitis (MK), particularly Pseudomonas. Newer SiHy lenses offer better oxygen permeability, reducing hypoxic stress.
SCL Fitting Principles - Finding Fit
- Goal: Optimal vision, comfort, ocular health.
- Key Parameters: Base Curve (BC) for sagittal depth, Diameter (Dia) for overall size.
- Assessment (3-Point Check): Evaluate on eye.
- Corneal Coverage: Complete, extends beyond limbus.
- Centration: Well-centered post-blink, minimal lag.
- Movement: Ideal 0.2-0.4mm with blink.
- Tight Fit: <0.1mm movement; conjunctival drag, vessel blanching, discomfort.
- Loose Fit: >1.0mm movement; decentration, edge lift-off, unstable vision.
- Over-Refraction (OR): Refine spherical/cylindrical power post-fit.
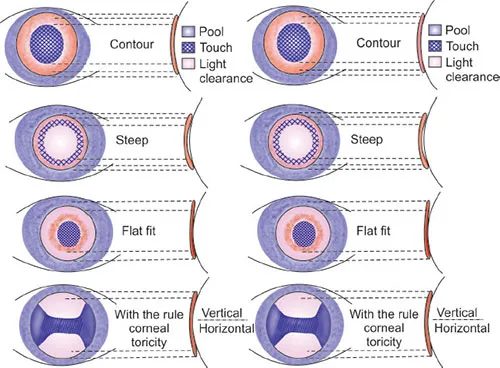
⭐ A tight SCL may initially feel comfortable but can lead to serious complications like corneal hypoxia and neovascularization.
SCL Complications - Red Eye Risks
Differentiating key SCL-related red eye conditions:
| Feature | MK (Infectious) | CLARE (Sterile Inflam.) | CLPU (Sterile Inflam.) | GPC (Allergic/Mech.) |
|---|---|---|---|---|
| Pain | Severe (Acanthamoeba: pain out of proportion) | Mod, Acute onset | Mild | Itching, FBS |
| Vision | ↓↓↓ | Normal | Normal | ↓ (mucus), variable |
| Infiltrate | Central, large, stromal, +AC reaction | Peripheral, small, multiple | Peripheral, small, round | Tarsal Papillae (>0.3mm) |
| Epi. Defect | Yes, overlying | No | Yes (over infiltrate) | No (cornea) |
| Discharge | Purulent | Watery/None | Watery/None | Mucoid strands |
⭐ Pseudomonas aeruginosa is the most common organism in SCL-related microbial keratitis, causing rapid, severe ulceration.
Other risks:
- Corneal Neovascularization: Vessels >1.5mm into cornea (chronic hypoxia).
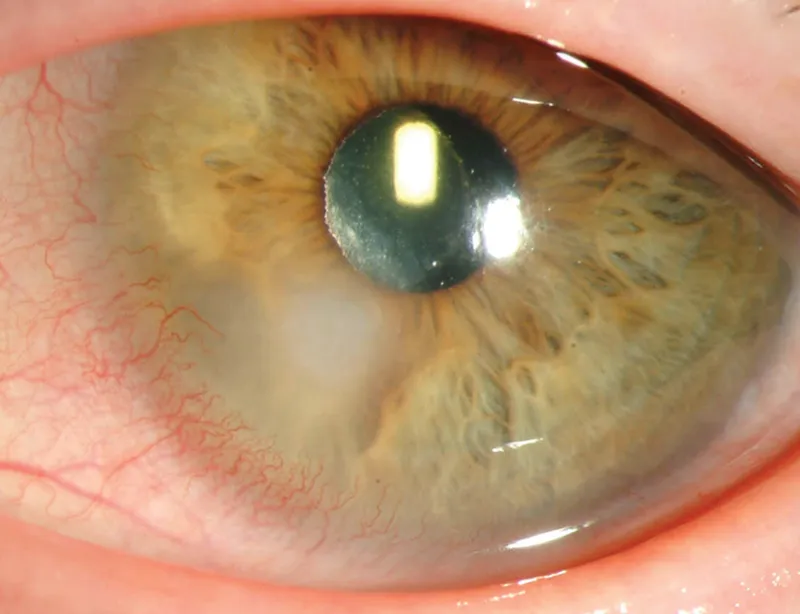
- Superior Epithelial Arcuate Lesion (SEAL): Mechanical trauma from lens edge.
- Tight Lens Syndrome (TLS): Acute pain, halos, corneal edema, often after sleep.
SCL Care Regimens - Clean Routine
- Goal: Prevent microbial keratitis.
- Key Systems:
- MPS: Rub & rinse crucial.
- H2O2: Preservative-free; neutralize (e.g., catalytic disc) for ~6 hours.
- Cleaning Steps:
⭐ Never use tap water for rinsing lenses or cases due to Acanthamoeba keratitis risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Materials: Hydrogels (HEMA) and Silicone Hydrogels (SiHy); SiHy for high oxygen permeability (Dk/t).
- Water Content: High water in hydrogels: ↑ Dk, but more deposits & dehydration.
- Pros: Great initial comfort, easy adaptation, good for intermittent/disposable wear.
- Cons: Less durable, prone to deposits, may blur vision with astigmatism.
- Key Risks: Microbial Keratitis (Pseudomonas), GPC, Corneal Neovascularization, Sterile Infiltrates.
- Fitting: Based on K-readings & HVID; SCLs are larger than cornea.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

