Scleral Contact Lenses: Basics - Giant Shields
- Large-diameter rigid gas permeable (RGP) lenses that rest on the sclera, vaulting over the cornea.
- Create a tear-filled reservoir, providing hydration and optical correction.

- Types (by diameter & bearing zone):
- Corneo-scleral: 12.9-13.5 mm, share bearing with cornea & sclera.
- Mini-scleral: 13.6-14.9 mm, vault cornea, land anterior to conjunctival vessels.
- Large-scleral: ≥15 mm, land on sclera, completely vault cornea & limbus.
- Materials: High Dk (oxygen permeability) RGP polymers (e.g., fluorosilicone acrylate).
- Mechanism: Vaults cornea → tear reservoir forms → neutralizes irregular astigmatism & hydrates ocular surface.
⭐ Scleral lenses are named for their landing zone, the sclera, not for covering the entire sclera. The vault over the cornea is key to their function, especially in irregular corneas and severe ocular surface disease.
- 📌 Mnemonic: Sclerals Sit on Sclera, Save Sight by Shielding & Smoothing cornea.
Scleral Contact Lenses: Indications & Benefits - Cornea Coddlers
- Key Indications:
- Irregular Corneas: Keratoconus, Pellucid Marginal Degeneration (PMD), post-LASIK ectasia, corneal grafts, scarring.
- Severe Ocular Surface Disease (SOSD): Advanced dry eye (e.g., Sjögren's, SJS, GVHD), neurotrophic/exposure keratopathy.
- High/complex refractive errors, uncorrectable by other means.
- Major Benefits:
- Superior Vision: Masks corneal irregularities, reduces aberrations.
- Enhanced Comfort: Vaults sensitive cornea, rests on less sensitive sclera.
- Corneal Protection & Hydration: Liquid reservoir acts as a "tear bandage."
- Stable Fit: Minimal dislodgement, suitable for active lifestyles.
- May defer or avoid corneal surgery (e.g., keratoplasty).
⭐ Scleral lenses provide a unique fluid reservoir between the lens and cornea, offering continuous hydration and promoting healing in severe ocular surface diseases, often improving quality of life significantly.
Scleral Contact Lenses: Fitting Principles - Precision Landing
- Goal: Vault cornea & limbus, land softly on sclera.
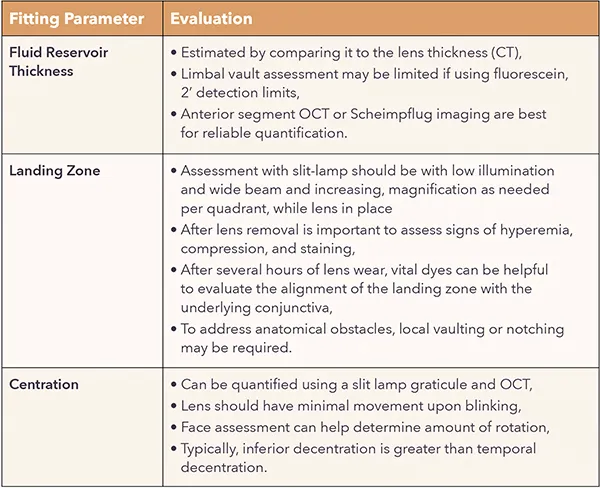
- Key Parameters & Assessment:
- Sagittal Depth (SAG): Overall lens height. Critical for initial selection (corneal profile).
- Central Corneal Clearance (CCC): 100-300 µm post-settling. OCT/optic section. Avoid corneal touch.
- Limbal Clearance: 50-100 µm. Prevents neovasc., protects stem cells.
- Scleral Landing Zone (SLZ): Even alignment on sclera. No blanching/impingement or edge lift/fluting. Toric haptics if needed.
- Over-refraction: Sphero-cylindrical, after optimal physical fit.
⭐ High-Yield Fact: Excessive central corneal clearance (>400 µm) can lead to hypoxic complications and midday fogging due to reduced tear exchange.
- Troubleshooting:
- Bubbles: Poor application or edge lift.
- Conjunctival Prolapse: Excessive limbal clearance.
- Midday Fogging: Debris, poor tear exchange.
- 📌 Mnemonic (Ideal Fit - "SAFE"): Scleral alignment, Apical clearance, Fluid reservoir, Edge lift absent.
Scleral Contact Lenses: Complications & Care - Fog Busters & Fixes
- Complications & Fixes:
- Midday Fogging (MDF): Debris in tear reservoir.
- Fix: Re-apply (fresh saline), PF viscous tears, Hydra-PEG.
- Hypoxia/Edema: Low Dk, tight fit.
- Fix: ↑Dk material, fenestrations, looser fit, ↓wear time.
- Conjunctival Issues: Prolapse, redness (tight haptic).
- Fix: Flatter peripheral curves, toric haptics.
- Giant Papillary Conjunctivitis (GPC): Lens deposits.
- Fix: Hygiene, mast cell stabilizers, lens replacement.
- Midday Fogging (MDF): Debris in tear reservoir.
- Lens Care:
- Insertion: PF saline (e.g., 0.9% NaCl).
- Cleaning/Disinfection: MPS; H2O2 systems (⚠️neutralize!).
- Handling: Hand wash, proper insertion/removal.
⭐ Midday fogging, from debris in post-lens tear reservoir, is the most common scleral lens complication.
High‑Yield Points - ⚡ Biggest Takeaways
- Vaults over the entire cornea, resting on the sclera; creates a tear reservoir.
- Key for irregular corneas (e.g., keratoconus, post-transplant), severe ocular surface disease, and high refractive errors.
- Made from high Dk gas permeable (GP) materials for optimal corneal oxygenation.
- Fitting involves assessing central vault, limbal clearance, and scleral landing zone alignment.
- Offers superior comfort, stability, and visual acuity for complex eyes; protects cornea.
- Potential issues: Midday fogging, hypoxia with poor fit, suction effect, conjunctival impingement.
- Requires preservative-free saline for filling; meticulous cleaning and handling essential for safety.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

