Contact Lenses for Keratoconus - Conical Cornea Conundrum
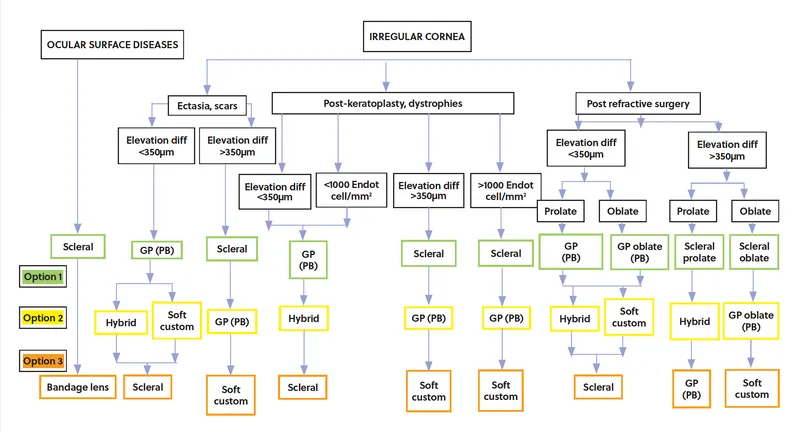
Keratoconus: progressive, non-inflammatory corneal ectasia causing a conical shape. Results in irregular astigmatism, myopia, ↓ visual acuity (VA), ghosting, halos. Spectacles often inadequate due to irregular surface.
- Role of Contact Lenses (CLs):
- Essential for visual rehabilitation.
- Mask corneal irregularity.
- Create a smooth anterior refractive surface.
- Significantly improve VA & vision quality.
- Primary Goals of CL Fitting:
- Achieve optimal VA.
- Ensure good comfort & wear duration.
- Preserve corneal health.
⭐ Rigid Gas Permeable (RGP) lenses are a mainstay for visual correction in keratoconus, effectively neutralizing irregular astigmatism.
Contact Lenses for Keratoconus - Vision's Custom Shields
- Rigid Gas Permeable (RGP) Lenses: Primary choice for KCN, mask corneal irregularity.
- Corneal RGPs: Smaller diameter (8-10 mm), rest on cornea. Best for mild to moderate KCN. Provide crisp vision.
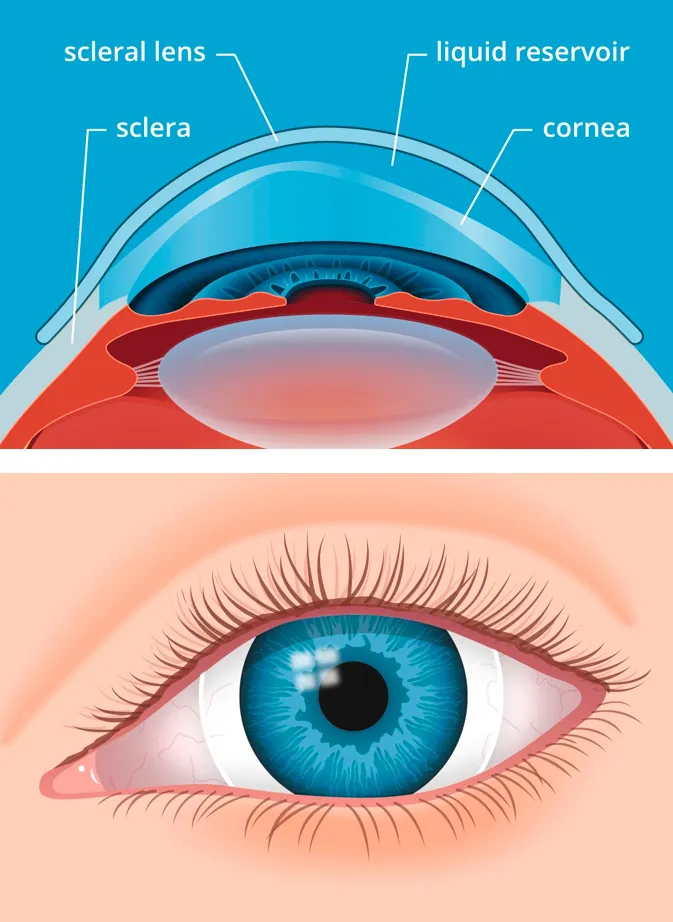
- Scleral RGPs: Larger diameter (15-22 mm), vault over entire cornea, rest on sclera. Indicated for moderate to advanced KCN, irregular astigmatism, or when corneal RGPs fail or are uncomfortable. Offer excellent comfort and stable vision.
- Hybrid Lenses: RGP center with a soft peripheral skirt.
- Combine RGP optical clarity with soft lens comfort. Good for patients with RGP intolerance.
- Specialty Soft Lenses for Keratoconus: Thicker design, custom parameters.
- Suitable for mild KCN or intolerance to RGPs/hybrids. Vision may be less sharp than RGPs for moderate/advanced cases.
- Piggyback System: Soft contact lens worn beneath an RGP lens.
- Enhances RGP comfort and centration, protects cornea.
⭐ Scleral lenses create a tear-filled vault over the irregular cornea, neutralizing aberrations and providing significant visual improvement and comfort, especially in advanced keratoconus and post-hydrops cases. They are also beneficial for ocular surface disease coexisting with KCN.
Contact Lenses for Keratoconus - Precision Lens Crafting
- Primary Goal: Vault corneal apex, optimal vision, comfort, corneal health.
- RGP Fitting Principles:
- Aim for "three-point touch" (apex/periphery light touch) or full apical clearance.
- Fluorescein: Central pooling (clearance), mid-peripheral alignment, peripheral edge lift (0.5-1.0 mm).
- Avoid harsh central bearing (prevents scarring).
- Scleral Lenses:
- Vault entire cornea & limbus; land on sclera. No conjunctival impingement.
- Initial central clearance: 200-300 $\mu$m (settles ~100 $\mu$m).
- Other Options: Hybrid (RGP center, soft skirt), piggyback (soft under RGP).
- Critical Assessment: Over-refraction, VA, comfort, centration & movement.
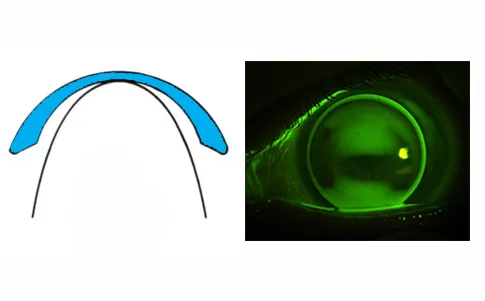
⭐ Ideal RGP fit shows apical clearance or feathery apical touch, avoiding harsh central bearing to prevent corneal scarring and ensure long-term success.
Contact Lenses for Keratoconus - Wearer's Wise Watch
- Regular Follow-ups: Crucial for monitoring fit, corneal health, and vision changes.
- Hygiene: Strict adherence to cleaning and disinfection protocols is paramount to prevent infections.
- Hand washing before handling lenses.
- Use recommended solutions; avoid tap water.
- Potential Complications:
- Corneal Abrasion: Due to poor fit or foreign body.
- Corneal Neovascularization: Often from chronic hypoxia.
- Giant Papillary Conjunctivitis (GPC): Allergic reaction to lens deposits.
- Microbial Keratitis: Serious, sight-threatening infection.
- Lens Intolerance: Discomfort, redness, reduced wear time.
- Management:
- Discontinue wear if pain, redness, or blurred vision occurs.
- Topical antibiotics/steroids as prescribed.
- Refitting or change in lens material/design.
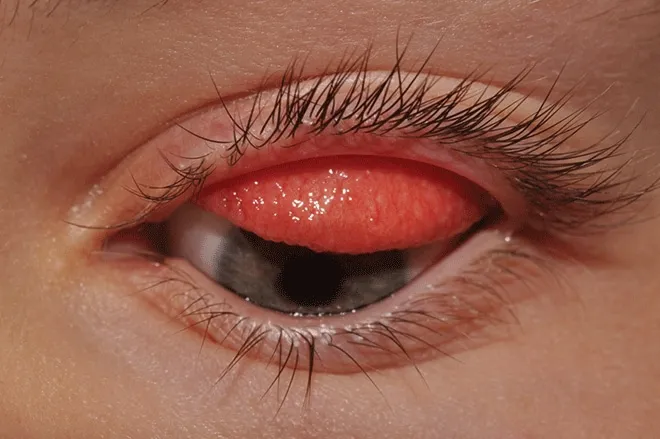
⭐ Fact: Microbial keratitis is a significant risk; Pseudomonas aeruginosa is a common culprit in contact lens-related infections, potentially leading to rapid corneal melt.
- Wear Time: Adhere to prescribed wearing schedule; avoid over-wear.
- Lens Replacement: Follow recommended replacement schedule (daily, monthly, etc.).
High‑Yield Points - ⚡ Biggest Takeaways
- RGP lenses are the mainstay for keratoconus, masking corneal irregularity.
- Optimal fit: apical clearance/light feather touch, good centration, and movement.
- Scleral lenses are vital for advanced keratoconus or RGP intolerance.
- Specialized RGP designs (e.g., Rose K) and hybrid lenses improve fit and comfort.
- Piggyback systems (soft lens under RGP) enhance comfort for sensitive eyes.
- Monitor for hypoxia-related complications like neovascularization and corneal warpage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

