CL Complications: Overview - Trouble in Sight
- Broad Categories:
- Infectious: Microbial Keratitis (MK) - Pseudomonas most common.
- Inflammatory (Sterile): Corneal Infiltrative Events (CIEs), Contact Lens Peripheral Ulcer (CLPU), Contact Lens Acute Red Eye (CLARE).
- Hypoxic: Corneal edema, neovascularization (pannus >1.5mm significant), microcysts.
- Mechanical/Traumatic: Giant Papillary Conjunctivitis (GPC), Superior Limbic Keratoconjunctivitis (SLK), corneal abrasions.
- Toxic/Allergic: Solution toxicity, preservative reactions.
- Lens Fit/Material: Tight Lens Syndrome, deposits, lens spoilage.
⭐ Microbial keratitis (MK) is the most sight-threatening complication, strongly linked to overnight wear and poor hygiene practices. Extended wear increases risk 4-5x.
Microbial Keratitis - Invader Alert!
- Serious, vision-threatening corneal infection, often aggressive.
- Key Risks: Overnight wear, poor lens hygiene, tap water exposure, contaminated solutions/cases.
- Common Pathogens:
- Bacteria: Pseudomonas aeruginosa (most common, rapid progression), Staphylococcus spp., Streptococcus spp.
- Fungi: Fusarium spp., Aspergillus spp.
- Protozoa: Acanthamoeba (severe pain, ring infiltrate).
- Symptoms: Severe pain, photophobia, ↓vision, redness, mucopurulent discharge.
- Signs: Corneal infiltrate/ulcer, epithelial defect, stromal edema, anterior chamber reaction (hypopyon).
- Management: Discontinue CL wear immediately. Corneal scraping for culture. Intensive fortified topical antibiotics.
⭐ Pseudomonas aeruginosa is notorious for causing rapid corneal melt and perforation in contact lens wearers, sometimes within 24-48 hours if not aggressively treated.
Sterile Events & Hypoxia - Suffocation & Flare-Ups
- Sterile Infiltrates (Asymptomatic Infiltrative Keratitis - AIK):
- Small (<1mm), peripheral, non-staining or minimally staining infiltrates.
- Mild/no symptoms. Causes: lens deposits, solutions, tight fit.
- Tx: D/C CL, lubricants. Steroids if severe (rule out infection).
- Contact Lens Peripheral Ulcer (CLPU):
- Acute, moderate pain, focal injection.
- Small (<2mm), round, peripheral infiltrate + overlying epithelial defect.
- Often Staph. aureus hypersensitivity.
- Tx: D/C CL, antibiotic/steroid combination.
- Contact Lens-Associated Red Eye (CLARE):
- Acute pain, redness, photophobia on waking. Often unilateral.
- Gram-negative endotoxins (typically extended wear).
- Diffuse injection, fine infiltrates (may be absent), no epithelial defect.
- Tx: D/C CL. Often self-limiting.
⭐ CLARE: Typically occurs after sleeping in lenses, linked to gram-negative bacterial endotoxins.
- Hypoxia (Chronic O₂ Deprivation):
- Manifestations: Corneal edema (striae, folds, microcysts → hazy vision), Neovascularization, Endothelial changes (polymegethism, pleomorphism).
- Management: Switch to high Dk/t lens, ↓wear time, consider RGP.
Mechanical & Toxic Effects - Lens Annoyances
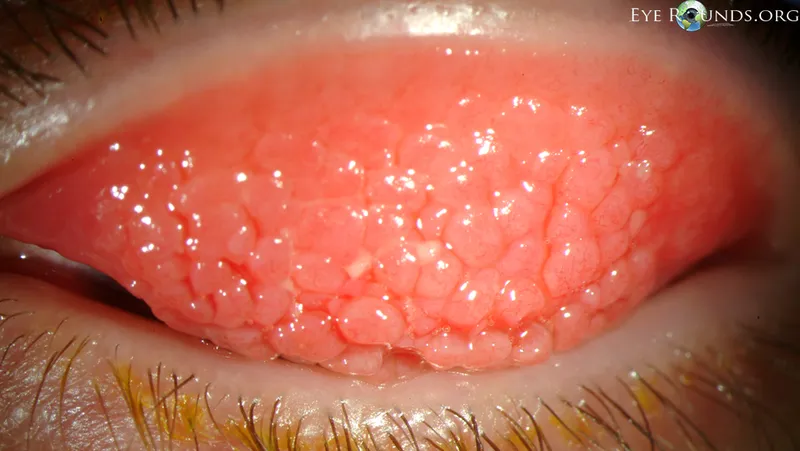
- Giant Papillary Conjunctivitis (GPC)
- Patho: Immune (Type I/IV hypersensitivity) to lens deposits/surface.
- Signs: Papillae >0.3 mm (cobblestone) on upper tarsal conjunctiva.
- Sx: Itching, mucus discharge, lens intolerance, ↓ wear time.
- Rx: Lens holiday, mast cell stabilizers, topical steroids (severe).
- Superior Epithelial Arcuate Lesion (SEAL)
- Etiology: Mechanical chafing by lens edge (tight RGP/soft lenses).
- Signs: Arcuate epithelial defect, superior cornea; fluorescein staining.
- Rx: Lens holiday, refit (looser/different design/material).
- Toxic Keratopathy / Solution-Induced Corneal Staining (SICS)
- Cause: Preservatives in solutions (PHMB, thimerosal, chlorhexidine).
- Signs: Diffuse punctate epithelial erosions (PEE), injection.
- Rx: Preservative-free solutions (e.g., H2O2 systems), ↓ wear time.
- Lens Deposits
- Types: Proteins (commonest), lipids, mucin, calcium.
- Effects: ↓VA, discomfort, FBS, ↑GPC risk, ↑microbial binding.
- Rx: Hygiene, enzyme cleaners, frequent replacement.
⭐ GPC, often triggered by lens deposits, is a leading cause of discomfort and discontinuation of contact lens wear.
High‑Yield Points - ⚡ Biggest Takeaways
- Microbial Keratitis (MK): Most serious; Pseudomonas aeruginosa common with overnight wear, poor hygiene.
- Corneal Neovascularization: Due to chronic hypoxia (low Dk/t); vessels >1.5mm into cornea.
- Giant Papillary Conjunctivitis (GPC): Allergic/mechanical to deposits; papillae >1mm on upper tarsus.
- Corneal Edema/Hypoxia: Causes blurred vision, halos, stromal striae/folds.
- CLPU (Contact Lens Peripheral Ulcer): Sterile peripheral infiltrates; less severe than infectious keratitis.
- Acanthamoeba Keratitis: Severe pain out of proportion to signs; linked to tap water, ring infiltrate (late).
- Solution-induced Keratopathy (SIK): Preservative toxicity; causes diffuse punctate epithelial erosions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

