Contact Lens

On this page
👁️ Contact Lens Fundamentals: The Precision Vision Interface
Contact lenses represent one of medicine's most intimate device-patient interfaces, sitting directly on the living cornea for hours each day. You'll master the engineering principles that govern oxygen permeability and biocompatibility, develop systematic approaches to fitting that balance optical precision with physiological tolerance, and build diagnostic frameworks to detect complications before they threaten vision. This lesson transforms contact lens practice from routine dispensing into evidence-based decision-making across materials, fitting algorithms, and complication management.
Contact Lens Classification Architecture
Contact lenses organize into distinct categories based on material properties, replacement schedules, and clinical applications:
- Material-Based Classification
- Soft Contact Lenses (SCL): 85-90% of global prescriptions
- Hydrogel lenses: 38-78% water content
- Silicone hydrogel: 24-48% water with enhanced oxygen permeability
- Rigid Gas Permeable (RGP): 8-12% of prescriptions
- Oxygen permeability: 15-163 Dk units
- Diameter: 8.5-10.5mm (smaller than soft lenses)
- Hybrid lenses: RGP center with soft skirt
- Central zone: 6-8mm rigid material
- Peripheral zone: 14-15mm soft hydrogel
- Soft Contact Lenses (SCL): 85-90% of global prescriptions
📌 Remember: SOFT - Silicone hydrogel Oxygen Flow Tissues - Modern silicone hydrogels deliver 5-6x more oxygen than traditional hydrogels, preventing corneal hypoxia during extended wear
- Replacement Schedule Framework
- Daily disposable: 24-hour single use, highest safety profile
- Weekly replacement: 7-day cycle with nightly removal
- Bi-weekly: 14-day replacement, most common modality
- Monthly: 30-day cycle requiring meticulous care
- Extended wear: 7-30 days continuous wear (FDA approved)
Corneal Physiology and Contact Lens Interaction
The cornea's 5-layer structure creates unique challenges for contact lens wear:
-
Epithelial Layer Considerations
- Thickness: 50-52 micrometers centrally
- Turnover rate: 7-14 days complete renewal
- Oxygen consumption: 4.2 μL O₂/cm²/hour
- Critical for lens adherence and comfort
-
Stromal Hydration Management
- Normal hydration: 78% water content
- Hypoxic swelling threshold: <11% oxygen availability
- Overnight swelling: 3-4% with proper oxygen transmission
- Pathological swelling: >8% indicates inadequate oxygenation
⭐ Clinical Pearl: Corneal oxygen consumption doubles during sleep due to closed eyelid environment. Extended wear lenses must provide Dk/t >87 to prevent overnight corneal edema and maintain <4% physiological swelling
| Parameter | Normal Cornea | Optimal CL Wear | Hypoxic Stress | Critical Threshold |
|---|---|---|---|---|
| Oxygen Flux | 21% ambient | >11% available | 5-8% available | <5% available |
| Stromal Swelling | 0% baseline | <4% overnight | 6-8% swelling | >8% pathological |
| Epithelial Integrity | 100% coverage | 95-98% intact | 85-90% coverage | <80% breakdown |
| Endothelial Function | 2500-3000 cells/mm² | Stable count | 2-3% annual loss | >5% annual loss |
| Tear pH | 7.4 ± 0.2 | 7.2-7.6 range | 6.8-7.8 range | <6.5 or >8.0 |
Modern contact lens materials balance four critical properties: oxygen permeability, water content, mechanical strength, and biocompatibility.
-
Hydrogel Chemistry
- Base polymer: HEMA (hydroxyethyl methacrylate)
- Water content range: 38-78% by weight
- Oxygen permeability: 8-28 Dk units
- Modulus of elasticity: 0.2-1.5 MPa
- Protein deposition: High due to ionic charges
-
Silicone Hydrogel Innovation
- Silicone content: 20-37% by weight
- Oxygen permeability: 60-163 Dk units
- Water content: 24-48% (lower than hydrogels)
- Surface treatment: Plasma coating or internal wetting agents
- Modulus: 0.7-1.5 MPa (stiffer than hydrogels)
💡 Master This: The Dk/t ratio (oxygen permeability divided by lens thickness) determines corneal oxygenation. Daily wear requires Dk/t >24, extended wear needs Dk/t >87. A 0.08mm thick silicone hydrogel with Dk 140 provides Dk/t 175-sufficient for 30-day continuous wear
Tear Film Dynamics and Lens Interaction
Contact lenses create a tri-layer tear system: pre-lens tear film, lens matrix, and post-lens tear film, each with distinct properties:
-
Pre-Lens Tear Film
- Thickness: 3-9 micrometers
- Breakup time: 8-15 seconds (normal eye 15-30 seconds)
- Lipid layer stability: Critical for lens wettability
- Mucin integration: Essential for surface adhesion
-
Post-Lens Tear Exchange
- Exchange rate: 1-16% per blink (lens design dependent)
- Stagnation zones: Risk areas for metabolic buildup
- Debris clearance: Reduced compared to non-lens wear
- pH buffering: Compromised in poor-fitting lenses
⭐ Clinical Pearl: Soft lens tear exchange averages 1-2% per blink versus 16% for well-fitted RGP lenses. This 8-fold difference explains why RGP lenses show superior resistance to protein deposition and infectious complications
The foundation of contact lens success lies in understanding these material-tissue interactions. Master these principles, and you possess the framework for optimizing every contact lens fitting decision.
👁️ Contact Lens Fundamentals: The Precision Vision Interface
🔬 Material Engineering: The Biocompatibility Matrix
Hydrogel Material Architecture
Traditional hydrogel lenses dominated contact lens practice for 30+ years, establishing the foundation for modern soft lens technology:
-
HEMA-Based Polymers
- Hydroxyethyl methacrylate: Primary monomer since 1971
- Water content: 38-78% determines oxygen permeability
- Oxygen transmission: Linear relationship with hydration
- Dk values: 8-28 units (insufficient for extended wear)
- Protein affinity: High due to hydroxyl groups
-
Ionic vs Non-Ionic Classification
- Non-ionic hydrogels: Lower protein deposition, better comfort
- Ionic hydrogels: Higher water content, increased deposit formation
- Charge density: Determines protein binding affinity
- Clinical preference: Non-ionic for daily wear applications
📌 Remember: HEMA-WOW - Hydroxyethyl Ethyl Methacrylate Absorbs Water Oxygen Well - Higher water content increases oxygen permeability but also increases protein deposition and reduces mechanical strength
Silicone Hydrogel Revolution
Silicone hydrogel materials revolutionized contact lens practice by decoupling oxygen permeability from water content:
-
Silicone Integration Technology
- Siloxane monomers: 20-37% of polymer matrix
- Oxygen pathways: Through silicone channels, not water
- Dk values: 60-163 units (3-6x higher than hydrogels)
- Water content: 24-48% (lower than high-Dk hydrogels)
- Modulus: 0.7-1.5 MPa (stiffer than hydrogels)
-
Surface Treatment Strategies
- Plasma oxidation: Creates hydrophilic surface layer
- Internal wetting agents: Polyvinylpyrrolidone (PVP) integration
- Phosphorylcholine coating: Biomimetic cell membrane surface
- Contact angle: <90 degrees for adequate wettability
- Surface energy: >20 dynes/cm for tear film stability
⭐ Clinical Pearl: First-generation silicone hydrogels showed 3-4x higher mechanical complications due to high modulus (1.5 MPa) and poor surface wettability. Modern materials achieve <0.9 MPa modulus with advanced surface treatments, reducing mechanical complications by 60-70%
| Material Property | Hydrogel | Silicone Hydrogel | RGP | Clinical Impact |
|---|---|---|---|---|
| Oxygen Permeability (Dk) | 8-28 | 60-163 | 15-163 | Corneal health |
| Water Content (%) | 38-78 | 24-48 | 0-1 | Comfort, deposition |
| Modulus (MPa) | 0.2-0.8 | 0.7-1.5 | 1000-3000 | Mechanical interaction |
| Protein Deposition | High | Moderate | Low | Replacement frequency |
| Lipid Deposition | Low | Moderate | High | Care requirements |
RGP materials provide superior optics and corneal health through advanced fluoropolymer chemistry:
-
Fluorosilicone Acrylate Polymers
- Fluorine content: 15-25% for oxygen permeability
- Silicone content: 20-35% for flexibility
- Acrylate backbone: Provides dimensional stability
- Dk range: 15-163 units (material dependent)
- Wetting angle: 40-80 degrees (requires surface treatment)
-
Material Selection Criteria
- Low Dk (15-30): New RGP wearers, stable prescriptions
- Medium Dk (30-60): Experienced wearers, daily wear
- High Dk (60-100): Extended wear, corneal compromise
- Ultra-high Dk (>100): Therapeutic applications, post-surgical
💡 Master This: RGP oxygen permeability increases with fluorine content, but >25% fluorine creates hydrophobic surfaces requiring aggressive wetting treatments. Optimal balance occurs at 18-22% fluorine content, providing Dk 60-100 with manageable surface properties
Advanced Material Technologies
Emerging contact lens materials address specific clinical challenges through targeted engineering:
-
Daily Disposable Innovations
- Water gradient technology: >80% surface water content
- UV blocking: Class I or Class II protection
- Thin design: 0.07-0.09mm center thickness
- Handling tint: Visibility without affecting optics
- Tear-activated lubrication: Hyaluronic acid integration
-
Specialty Material Applications
- Scleral lens materials: High Dk (>100) for 16+ hour wear
- Orthokeratology: Ultra-high Dk (>100) for overnight wear
- Therapeutic lenses: Collagen shields, drug-eluting polymers
- Cosmetic enhancement: FDA-approved pigments and dyes
⭐ Clinical Pearl: Daily disposable lenses eliminate 95% of care-related complications and reduce microbial keratitis risk by 70-80% compared to reusable lenses. The convenience factor drives 60% of new contact lens fits toward daily disposables despite 2-3x higher annual costs
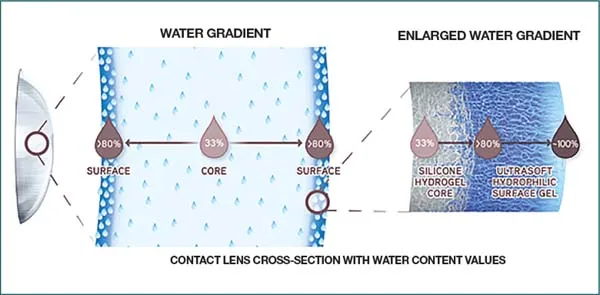
Understanding material science enables predictive contact lens selection based on patient physiology, lifestyle, and ocular surface characteristics. These principles guide every successful fitting decision.
🔬 Material Engineering: The Biocompatibility Matrix
🎯 Fitting Mastery: The Precision Alignment Protocol
Pre-Fitting Assessment Architecture
Comprehensive pre-fitting evaluation establishes the foundation for successful contact lens wear:
-
Corneal Measurements
- Keratometry readings: Central 3mm zone assessment
- Corneal diameter: 11.5-12.5mm horizontal visible iris diameter (HVID)
- Corneal topography: >8000 data points for irregular astigmatism detection
- Pachymetry: Central thickness 540-560 micrometers
- Eccentricity values: 0.3-0.6 for asphericity quantification
-
Tear Film Evaluation
- Tear breakup time: >10 seconds for contact lens candidacy
- Schirmer test: >10mm in 5 minutes for adequate volume
- Tear osmolarity: <308 mOsm/L indicates stable tear film
- Meibomian gland assessment: >50% functional glands required
- Tear meniscus height: 0.2-0.5mm optimal range
📌 Remember: TEARS - Time (breakup >10s), Evaluate (Schirmer >10mm), Assess (osmolarity <308), Review (meibomian function), Size (meniscus 0.2-0.5mm) - All five parameters must be adequate for successful contact lens wear
Soft Contact Lens Fitting Principles
Soft lens fitting relies on centration, coverage, and movement assessment for optimal physiological function:
-
Base Curve Selection
- Relationship: 0.7-1.0mm flatter than flattest keratometry reading
- Standard progression: 8.4mm, 8.8mm, 9.2mm base curves
- Steep fit indicators: Minimal movement, central bearing
- Flat fit indicators: Excessive movement, edge standoff
- Optimal fit: 0.5-1.0mm movement with blink
-
Diameter Considerations
- Standard diameter: 14.0-14.5mm for most eyes
- Large eyes (HVID >12.0mm): 14.5-15.0mm diameter
- Small eyes (HVID <11.5mm): 13.5-14.0mm diameter
- Coverage requirement: 1.5-2.0mm beyond limbus
- Centration tolerance: ±0.5mm from geometric center
⭐ Clinical Pearl: Soft lens fitting follows the "Goldilocks principle"-too tight causes corneal molding and reduced tear exchange, too loose creates lens decentration and visual instability. Optimal fit shows 0.5-1.0mm movement with blink and complete corneal coverage at rest
| Fitting Assessment | Optimal Finding | Steep Fit | Flat Fit | Clinical Action |
|---|---|---|---|---|
| Movement with Blink | 0.5-1.0mm | <0.5mm | >1.5mm | Adjust base curve |
| Centration | ±0.5mm from center | Central bearing | Inferior decentration | Change diameter |
| Edge Position | 1.5-2.0mm past limbus | Tight edge | Edge standoff | Modify parameters |
| Post-Blink Movement | Returns to center | Minimal movement | Excessive lag | Refit lens |
| Comfort Level | Minimal awareness | Tight sensation | Lens awareness | Parameter change |
RGP fitting requires precise fluorescein pattern interpretation and tear exchange optimization:
-
Base Curve Selection Strategy
- Starting point: 0.1-0.2mm steeper than flattest K reading
- With-the-rule astigmatism: Fit flattest meridian
- Against-the-rule astigmatism: Fit steepest meridian
- Irregular astigmatism: Topography-guided fitting
- Presbyopic patients: 0.1mm flatter for better centration
-
Fluorescein Pattern Interpretation
- Optimal pattern: Light central touch, mid-peripheral clearance
- Apical clearance: 10-20 micrometers fluorescein thickness
- Edge clearance: 20-40 micrometers for tear exchange
- Bearing patterns: Indicate steep base curve
- Bubble formation: Suggests inadequate edge lift
💡 Master This: RGP fluorescein patterns reveal corneal-lens relationship with micrometer precision. Central touch with peripheral clearance creates optimal tear pump action, while central pooling indicates steep fitting and edge bearing suggests flat fitting. Pattern interpretation guides 0.05mm base curve adjustments
Specialty Fitting Considerations
Advanced fitting scenarios require modified approaches and specialized techniques:
-
Astigmatic Correction
- Spherical equivalent: ≤0.75D cylinder with soft lenses
- Toric soft lenses: >0.75D cylinder or >0.50D residual
- RGP masking: Up to 2.50D corneal astigmatism
- Axis stability: ±5 degrees for toric lens success
- Rotation assessment: 30-minute settling time required
-
Presbyopic Fitting
- Multifocal designs: Simultaneous or alternating vision
- Add power progression: +1.00D to +2.50D typical range
- Dominant eye: Distance-centered multifocal design
- Non-dominant eye: Near-centered or monovision approach
- Success rate: 70-80% with proper patient selection
⭐ Clinical Pearl: Presbyopic contact lens success depends on realistic expectations and proper trial periods. Simultaneous vision multifocals require 2-4 weeks neural adaptation, while monovision shows immediate but reduced stereopsis. Patient lifestyle and visual demands determine optimal correction strategy
Mastering fitting principles enables predictable contact lens success through systematic assessment and parameter optimization. These protocols transform fitting from art to science.
🎯 Fitting Mastery: The Precision Alignment Protocol
🔍 Diagnostic Excellence: The Clinical Assessment Matrix
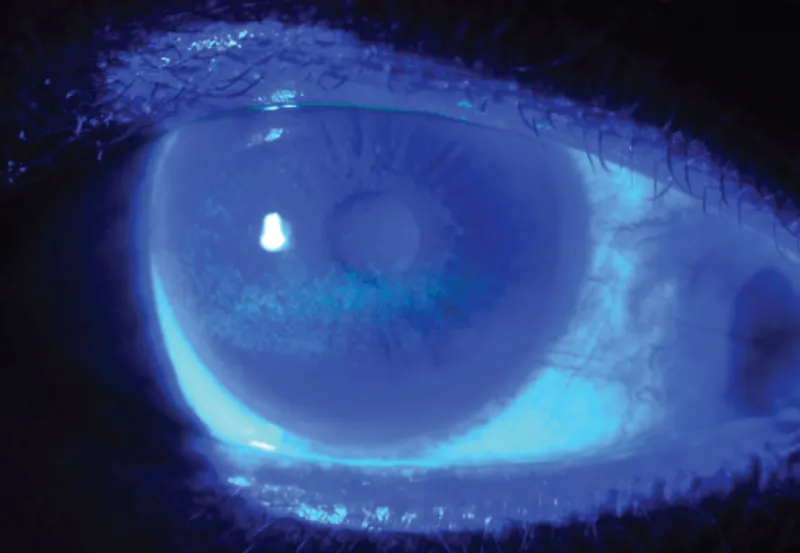
Systematic Examination Protocol
Comprehensive contact lens assessment follows a structured approach to detect subtle changes in ocular physiology:
-
Pre-Lens Evaluation Sequence
- Visual acuity: Baseline and over-refraction assessment
- Slit lamp examination: 16x magnification for epithelial detail
- Fluorescein staining: Cobalt blue filter for epithelial defects
- Tear film assessment: Breakup time and volume measurement
- Lens position: Centration and movement evaluation
-
Lens-Specific Assessment
- Surface deposits: Protein, lipid, and calcium accumulation
- Edge integrity: Chips, tears, and parameter changes
- Optical quality: Clarity and surface smoothness
- Wettability: Contact angle and dewetting patterns
- Dimensional stability: Power and base curve verification
📌 Remember: CLEAR - Cornea (epithelial integrity), Lens (surface quality), Edema (stromal swelling), Artery (conjunctival injection), Redness (inflammatory response) - Systematic assessment prevents 95% of serious complications through early detection
Corneal Health Assessment
The cornea provides critical indicators of contact lens biocompatibility and physiological stress:
-
Epithelial Integrity Evaluation
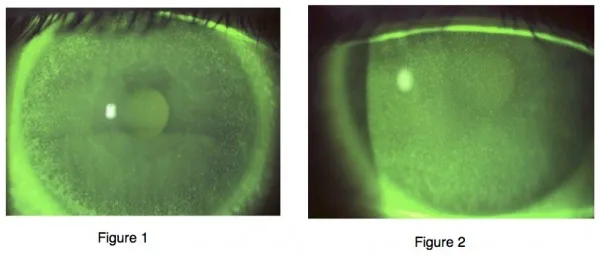
- Fluorescein staining patterns: Punctate, confluent, or geographic
- Staining density: Grade 0-4 scale for severity assessment
- Distribution patterns: Superior (mechanical), inferior (desiccation)
- Healing rate: 24-48 hours for superficial defects
- Recurrence patterns: Indicate chronic irritation sources
-
Stromal Response Monitoring
- Corneal thickness: Pachymetry for edema detection
- Physiological swelling: <4% overnight acceptable
- Pathological edema: >6% indicates hypoxic stress
- Striae formation: Vertical folds in Descemet's membrane
- Recovery time: 2-4 hours post-lens removal
⭐ Clinical Pearl: Superior epithelial arcuate lesions (SEAL) occur in 15-20% of silicone hydrogel wearers due to mechanical interaction with upper lid. Grade 2+ staining requires lens parameter modification or material change to prevent progression to corneal infiltrates
| Complication Type | Clinical Signs | Severity Grading | Treatment Protocol | Follow-up Timing |
|---|---|---|---|---|
| Epithelial Staining | Punctate fluorescein uptake | Grade 1-4 scale | Lens modification | 1-2 weeks |
| Corneal Edema | Stromal thickening | <4% to >8% swelling | Oxygen increase | 24-48 hours |
| Neovascularization | Vessel ingrowth >1mm | Mild to severe | Lens discontinuation | 1-3 months |
| Giant Papillary Conjunctivitis | Papillae >0.3mm | Grade 1-4 severity | Anti-inflammatory | 2-4 weeks |
| Microbial Keratitis | Infiltrate with epithelial defect | Mild to severe | Antibiotic therapy | Daily initially |
Lens performance assessment evaluates optical quality, surface integrity, and parameter stability:
-
Optical Assessment Protocol
- Visual acuity: Distance and near performance
- Over-refraction: Residual refractive error
- Contrast sensitivity: Functional vision quality
- Glare testing: Night vision performance
- Stereopsis: Binocular function maintenance
-
Surface Quality Evaluation
- Deposit classification: Protein (white), lipid (oily), calcium (crystalline)
- Surface roughness: Tactile and visual assessment
- Wetting characteristics: Dewetting patterns and contact angles
- Edge condition: Smoothness and integrity evaluation
- Parameter verification: Power and base curve stability
💡 Master This: Protein deposits appear as white, chalky accumulations and reduce oxygen transmission by 20-30%. Lipid deposits create rainbow patterns and compromise surface wettability. Calcium deposits form crystalline structures and cause mechanical irritation. Each deposit type requires specific cleaning protocols or replacement schedules
Advanced Diagnostic Techniques
Sophisticated assessment tools provide quantitative data for complex contact lens cases:
-
Corneal Topography Applications
- Pre-fitting: Irregular astigmatism detection
- Post-fitting: Corneal molding assessment
- Orthokeratology: Treatment zone evaluation
- Keratoconus: Progression monitoring
- Resolution: >8,000 data points for precision mapping
-
Anterior Segment OCT
- Lens-cornea relationship: Cross-sectional imaging
- Tear film thickness: Quantitative measurement
- Scleral lens vault: Precise clearance assessment
- Epithelial thickness: Remodeling detection
- Resolution: 5-10 micrometer accuracy
⭐ Clinical Pearl: Anterior segment OCT reveals subclinical corneal changes 2-3 weeks before slit lamp detection. Epithelial thinning >10 micrometers centrally indicates chronic mechanical stress, while stromal thickening >20 micrometers suggests hypoxic edema requiring immediate intervention
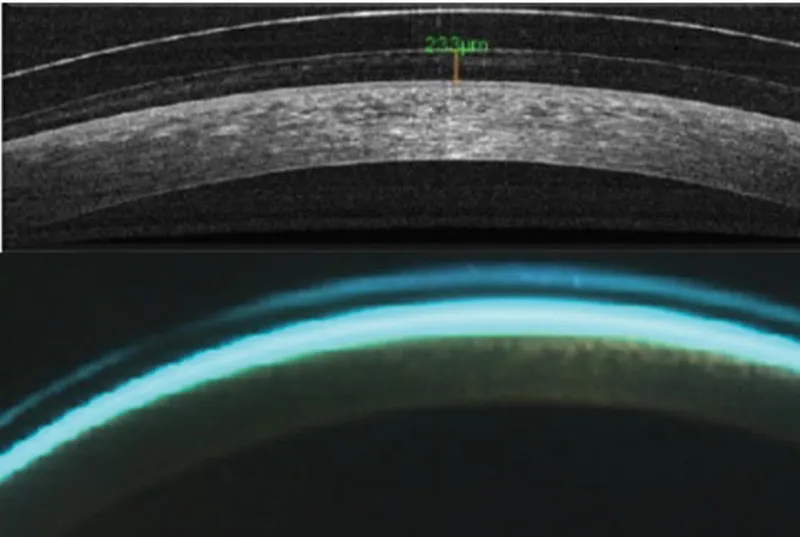
Systematic diagnostic protocols enable early detection and prevention of contact lens complications, transforming reactive care into predictive management. These assessment tools guide evidence-based clinical decisions for optimal patient outcomes.
🔍 Diagnostic Excellence: The Clinical Assessment Matrix
⚖️ Treatment Algorithms: The Evidence-Based Management Matrix
Microbial Keratitis Management Protocol
Microbial keratitis represents the most serious contact lens complication, requiring immediate intervention with standardized protocols:
-
Immediate Assessment Algorithm
- Visual acuity: Document baseline function
- Slit lamp examination: Size, depth, and location of infiltrate
- Fluorescein staining: Epithelial defect presence and extent
- Anterior chamber: Cell and flare assessment
- Culture protocol: Corneal scraping before antibiotic initiation
-
Treatment Initiation Criteria
- Infiltrate size: >1mm diameter requires aggressive therapy
- Central location: Within 4mm of visual axis
- Epithelial defect: Any size with underlying infiltrate
- Anterior chamber reaction: >1+ cells indicates severity
- Contact lens history: Extended wear increases risk 10-15x
📌 Remember: SIGHT - Stop lens wear immediately, Infiltrate measurement and documentation, Get cultures before antibiotics, Hourly fortified antibiotics initially, Topical steroids only after improvement - This protocol reduces vision-threatening outcomes by 70-80%
Inflammatory Response Management
Non-infectious inflammatory responses require differentiated treatment approaches based on severity and underlying etiology:
-
Contact Lens-Induced Acute Red Eye (CLARE)
- Incidence: 5-15% of extended wear users annually
- Presentation: Acute onset pain, photophobia, injection
- Management: Immediate lens discontinuation, topical steroids
- Resolution time: 24-48 hours with appropriate treatment
- Return to wear: 1-2 weeks after complete resolution
-
Giant Papillary Conjunctivitis (GPC)
- Prevalence: 10-15% of contact lens wearers
- Grading: Grade 1-4 based on papillae size and symptoms
- Treatment approach: Anti-inflammatory + lens modification
- Success rate: 80-90% with combined therapy
- Prevention: Daily disposables reduce incidence by 60-70%
⭐ Clinical Pearl: CLARE shows circumlimbal injection with minimal discharge, while microbial keratitis presents with mucopurulent discharge and corneal infiltrate. CLARE resolves within 48 hours of lens discontinuation; persistent symptoms beyond 72 hours require culture and antibiotic therapy
| Complication | Onset Pattern | Key Features | Treatment Protocol | Success Rate |
|---|---|---|---|---|
| CLARE | Acute (<24h) | Circumlimbal injection | Lens stop + steroids | 95-98% |
| GPC | Gradual (weeks) | Upper lid papillae | Anti-inflammatory + lens change | 80-90% |
| SEAL | Chronic (months) | Superior arcuate staining | Parameter modification | 85-95% |
| Corneal Infiltrates | Variable | White/gray lesions | Antibiotics ± steroids | 90-95% |
| Dry Eye | Progressive | Punctate staining | Lubrication + lens change | 70-85% |
Mechanical complications result from lens-tissue interaction and require parameter optimization rather than pharmacological intervention:
-
Superior Epithelial Arcuate Lesions (SEAL)
- Mechanism: Mechanical friction with upper eyelid
- Risk factors: Silicone hydrogel materials, tight lens fit
- Grading: Grade 1-4 based on staining extent
- Management: Lens parameter modification or material change
- Prevention: Lower modulus materials, optimal fitting
-
Corneal Molding and Warpage
- Incidence: 15-25% of long-term soft lens wearers
- Detection: Corneal topography changes from baseline
- Reversibility: 2-8 weeks after lens discontinuation
- Prevention: Proper fitting and adequate tear exchange
- Monitoring: Annual topography for early detection
💡 Master This: SEAL progression follows predictable patterns-Grade 1 (minimal staining) responds to lens parameter changes, Grade 2-3 requires material modification, and Grade 4 (confluent staining) necessitates temporary discontinuation with therapeutic lens protection during healing
Hypoxic Complication Management
Oxygen-related complications require immediate intervention to prevent permanent corneal damage:
-
Corneal Neovascularization
- Threshold: >1mm vessel ingrowth from limbus
- Progression rate: 0.1-0.2mm/month with continued hypoxia
- Treatment: High-Dk materials or lens discontinuation
- Regression: Partial vessel regression over 6-12 months
- Prevention: Dk/t >24 for daily wear, >87 for extended wear
-
Corneal Edema and Striae
- Acute edema: >4% corneal thickening
- Chronic changes: Endothelial cell loss >2% annually
- Recovery: 2-6 hours post-lens removal for acute cases
- Irreversibility: Chronic endothelial damage permanent
- Monitoring: Pachymetry and specular microscopy
⭐ Clinical Pearl: Corneal neovascularization beyond 2mm from the limbus rarely regresses completely, creating permanent vascular channels that increase infection risk by 3-4x. Early detection at 1mm ingrowth allows complete regression with appropriate oxygen management
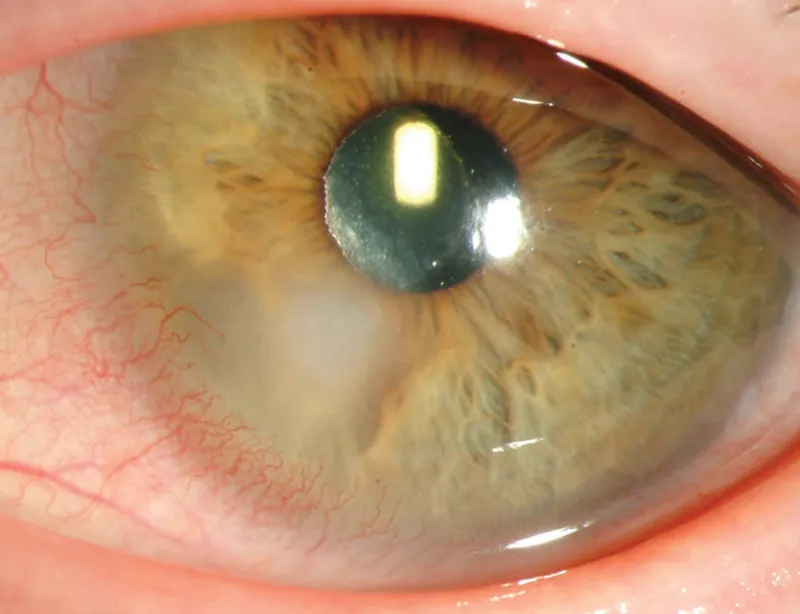
Treatment Outcome Optimization
Evidence-based protocols maximize treatment success through systematic monitoring and objective endpoints:
-
Success Metrics
- Visual acuity: Return to baseline within 1-2 weeks
- Comfort scores: >7/10 on validated scales
- Complication resolution: Complete healing within timeframe
- Recurrence rates: <5% within 6 months
- Patient satisfaction: >85% willing to continue lens wear
-
Follow-up Protocols
- Acute complications: 24-48 hour initial follow-up
- Moderate complications: 1-2 week reassessment
- Chronic issues: Monthly monitoring until resolution
- Return to wear: Graduated schedule with close monitoring
- Long-term surveillance: Annual comprehensive examination
Evidence-based treatment algorithms transform contact lens complication management from reactive intervention to predictive prevention, optimizing outcomes through systematic protocols and quantified success metrics.
⚖️ Treatment Algorithms: The Evidence-Based Management Matrix
🔗 Advanced Integration: The Multi-System Mastery Network
Corneal-Lens-Tear Film Ecosystem
The contact lens creates a tri-compartment system where each component influences the others through dynamic feedback loops:
-
Oxygen Transport Cascade
- Atmospheric oxygen: 21% concentration at sea level
- Pre-lens tear film: Oxygen reservoir and transport medium
- Lens matrix: Rate-limiting step for oxygen delivery
- Post-lens tear film: Metabolic waste removal pathway
- Corneal consumption: 4.2 μL O₂/cm²/hour baseline demand
-
Metabolic Integration Network
- Glucose transport: Tear film primary source (0.5 mM concentration)
- Lactate accumulation: Anaerobic metabolism byproduct
- pH regulation: Bicarbonate buffering system
- Osmotic balance: 280-320 mOsm/L physiological range
- Protein turnover: Continuous epithelial renewal cycle
📌 Remember: ECOSYSTEM - Epithelial renewal, Corneal oxygenation, Osmotic balance, Systemic health, Year-round monitoring, Surface wetting, Tear exchange, Environmental factors, Material compatibility - All nine factors interact continuously during contact lens wear
Circadian Rhythm Integration
Contact lens physiology follows 24-hour cycles that influence fitting decisions and wearing schedules:
-
Diurnal Corneal Changes
- Morning thickness: +3-4% from overnight swelling
- Afternoon stability: Baseline thickness achieved
- Evening dehydration: -1-2% thickness reduction
- Keratometry shifts: ±0.25D throughout day
- Tear production: 50% reduction during sleep
-
Lens Performance Cycles
- Morning insertion: Optimal corneal hydration for comfort
- Midday stability: Peak visual performance period
- Evening accumulation: Maximum deposit formation
- Overnight recovery: Corneal repair and regeneration
- Weekly patterns: Cumulative stress effects
⭐ Clinical Pearl: Corneal thickness varies ±5% throughout the day, with maximum swelling upon awakening and minimum thickness in late afternoon. Extended wear lenses must accommodate overnight swelling of 3-4% without compromising corneal physiology or lens performance
Environmental Adaptation Strategies
Contact lens performance varies significantly across environmental conditions, requiring adaptive management approaches:
-
Climate-Specific Considerations
- Low humidity (<30%): Increased evaporation, enhanced lubrication needed
- High humidity (>70%): Reduced evaporation, deposit accumulation risk
- Temperature extremes: Material property changes, comfort variations
- Altitude effects: Reduced oxygen partial pressure above 8,000 feet
- Seasonal variations: Allergy seasons require modified care regimens
-
Occupational Environment Integration
- Computer users: Reduced blink rates (5-7/minute vs 15-20/minute)
- Outdoor workers: UV protection and debris resistance priorities
- Healthcare workers: Infection control and extended wear considerations
- Athletes: Stability and moisture retention requirements
- Pilots: Altitude and cabin pressure adaptations
💡 Master This: Computer vision syndrome affects 90% of contact lens wearers using digital devices >3 hours daily. Blink rates decrease by 60-70%, tear film stability reduces by 40%, and surface dehydration increases 3-4x. Lubricating drops every 2 hours and 20-20-20 rule (20-second breaks every 20 minutes looking 20 feet away) restore normal physiology
| Environmental Factor | Impact on Lens Wear | Adaptation Strategy | Success Rate |
|---|---|---|---|
| Low Humidity (<30%) | Increased dehydration | Frequent lubrication | 85-90% |
| High Altitude (>8000ft) | Reduced oxygen availability | High-Dk materials | 90-95% |
| Digital Device Use | Reduced blink rate | Scheduled breaks + drops | 80-85% |
| Air Conditioning | Tear film instability | Humidification + protection | 75-85% |
| Allergen Exposure | Inflammatory response | Daily disposables | 90-95% |
Contact lens success depends on systemic health factors that influence ocular surface physiology:
-
Hormonal Influences
- Pregnancy: Corneal thickening and curvature changes
- Menopause: Tear production reduction (30-40% decrease)
- Thyroid disorders: Lid function and tear quality changes
- Diabetes: Corneal sensitivity and healing impairment
- Autoimmune conditions: Dry eye and inflammatory responses
-
Medication Interactions
- Antihistamines: Tear production reduction (20-30%)
- Antidepressants: Anticholinergic effects on tear and saliva
- Diuretics: Systemic and ocular dehydration
- Beta-blockers: Reduced tear production and corneal sensitivity
- Isotretinoin: Severe dry eye and meibomian dysfunction
⭐ Clinical Pearl: Hormonal contraceptives alter tear film composition in 60-70% of users, reducing lysozyme concentration by 25% and increasing protein deposition on contact lenses. Daily disposables show 40% better success rates in hormonal contraceptive users compared to monthly replacement lenses
Technology Integration Frontiers
Emerging technologies create new possibilities for personalized contact lens care:
-
Smart Lens Development
- Glucose monitoring: Tear glucose correlation with blood levels
- Pressure sensing: Intraocular pressure continuous monitoring
- Drug delivery: Sustained release therapeutic agents
- UV protection: Photochromic and UV-blocking technologies
- Augmented reality: Digital display integration possibilities
-
Artificial Intelligence Applications
- Fitting optimization: Machine learning parameter prediction
- Complication prediction: Risk stratification algorithms
- Personalized care: Individual response pattern recognition
- Outcome prediction: Success probability modeling
- Treatment optimization: Evidence-based protocol refinement
💡 Master This: Artificial intelligence analysis of corneal topography, tear film parameters, and patient history can predict contact lens success with 85-90% accuracy before initial fitting. Machine learning algorithms identify subtle patterns in >50 variables that human assessment cannot detect, enabling personalized lens selection and reduced fitting time
Advanced integration recognizes contact lens wear as a complex physiological system requiring multi-factorial optimization. Understanding these interconnections enables predictive management and superior patient outcomes through systems-based approaches.
🔗 Advanced Integration: The Multi-System Mastery Network
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Matrix
Essential Parameter Arsenal
Critical Measurements for Instant Decision-Making:
-
Corneal Assessment Thresholds
- Keratometry range: 40.00-48.00D (normal population 95%)
- Corneal diameter: 11.5-12.5mm HVID for lens selection
- Central thickness: 540-560 micrometers (contact lens candidates)
- Tear breakup time: >10 seconds minimum for lens wear
- Schirmer test: >10mm/5 minutes adequate tear volume
-
Oxygen Requirements by Modality
- Daily wear minimum: Dk/t >24 prevents corneal edema
- Extended wear threshold: Dk/t >87 for overnight safety
- Therapeutic applications: Dk/t >125 for compromised corneas
- Scleral lens requirements: Dk >100 for 16+ hour wear
- Orthokeratology: Dk >100 for overnight corneal reshaping
📌 Remember: RAPID - Range (K readings 40-48D), Adequate (tears >10s), Permeability (Dk/t >24), Integrity (epithelium intact), Diameter (HVID 11.5-12.5mm) - Five essential measurements for 90% of fitting decisions
Complication Recognition Matrix
Instant Pattern Recognition for Critical Interventions:
| Clinical Sign | Severity Grade | Immediate Action | Follow-up Timing | Success Rate |
|---|---|---|---|---|
| Corneal Infiltrate >1mm | Severe | Culture + fortified antibiotics | 24 hours | 85-90% |
| SEAL Grade 3+ | Moderate | Lens parameter change | 1-2 weeks | 90-95% |
| Corneal Edema >6% | Severe | High-Dk lens or discontinue | 48 hours | 95-98% |
| GPC Grade 3+ | Moderate | Anti-inflammatory + lens change | 2-4 weeks | 80-85% |
| Neovascularization >2mm | Severe | Lens discontinuation | 1-3 months | 60-70% |
Evidence-Based Interventions with Quantified Outcomes:
-
Microbial Keratitis Protocol
- Hour 0: Lens removal, culture, visual acuity documentation
- Hour 1: Fortified antibiotics (Vancomycin 50mg/mL + Tobramycin 14mg/mL)
- Hours 1-24: Hourly antibiotic administration
- Day 2-3: Assess response, adjust based on culture
- Week 1-2: Taper frequency, monitor healing
-
CLARE Management Algorithm
- Immediate: Lens discontinuation, document injection pattern
- Day 1: Topical steroid (Prednisolone 1% QID)
- Day 2-3: Assess resolution, continue steroids
- Week 1-2: Gradual return to lens wear
- Success rate: 95-98% complete resolution
⭐ Clinical Pearl: CLARE resolves within 48 hours in 98% of cases with appropriate treatment. Persistent symptoms beyond 72 hours indicate possible infection requiring culture and antibiotic therapy. Never use steroids without ruling out microbial etiology
Material Selection Decision Tree
Systematic Material Matching for Optimal Outcomes:
Fitting Success Optimization
Quantified Parameters for Predictable Outcomes:
-
Soft Lens Fitting Metrics
- Optimal movement: 0.5-1.0mm with blink
- Centration tolerance: ±0.5mm from geometric center
- Edge clearance: 1.5-2.0mm beyond limbus
- Post-blink recovery: <3 seconds to center
- Comfort threshold: >7/10 on validated scales
-
RGP Fitting Benchmarks
- Central clearance: 10-20 micrometers fluorescein thickness
- Edge lift: 20-40 micrometers for tear exchange
- Movement: 1-2mm with blink
- Centration: ±1mm acceptable range
- Adaptation period: 1-2 weeks for 80% success
💡 Master This: Soft lens success correlates with movement patterns-<0.5mm movement indicates tight fit with reduced tear exchange, >1.5mm movement suggests loose fit with decentration risk. Optimal 0.5-1.0mm movement ensures adequate oxygenation and debris clearance while maintaining visual stability
Emergency Response Protocols
Critical Interventions for Sight-Threatening Complications:
-
Red Eye Triage System
- Green Zone: Mild injection, no pain (Continue wear with monitoring)
- Yellow Zone: Moderate injection, mild discomfort (Lens removal, 24-48h follow-up)
- Red Zone: Severe injection, pain, photophobia (Immediate evaluation, culture if indicated)
-
Pain Assessment Matrix
- Grade 1-3: Mild discomfort (Lens adjustment or lubrication)
- Grade 4-6: Moderate pain (Lens removal, evaluation within 24 hours)
- Grade 7-10: Severe pain (Emergency evaluation, rule out infection)
Success Metrics Dashboard
Quantified Outcomes for Practice Optimization:
-
Patient Satisfaction Benchmarks
- >90%: Excellent practice performance
- 85-90%: Good performance, room for improvement
- 80-85%: Adequate performance, systematic review needed
- <80%: Poor performance, protocol revision required
-
Complication Rates (Annual)
- Microbial keratitis: <0.02% daily wear, <0.2% extended wear
- CLARE incidence: <5% extended wear users
- GPC development: <10% all contact lens wearers
- Corneal neovascularization: <2% with proper oxygen management
⭐ Clinical Pearl: Daily disposable lenses reduce overall complication rates by 60-70% compared to monthly replacement schedules. Microbial keratitis risk drops from 4.1 per 10,000 patient-years with monthly lenses to 1.2 per 10,000 with daily disposables-a 70% risk reduction
This clinical arsenal transforms complex contact lens decisions into systematic protocols with predictable outcomes, enabling rapid, evidence-based patient care that optimizes safety and success rates across all practice scenarios.
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Matrix
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























