Introduction to Tele-Ophthalmology - Tele-Eyes Intro
- Definition: Delivery of eye care services using information and communication technology (ICT) where distance is a critical factor.
- Goal: Bridge the gap in eye care access, especially for remote/underserved populations in India.
- Key Modalities:
- Store-and-Forward (Asynchronous): Images/data collected & sent for later review (e.g., diabetic retinopathy screening).
- Real-Time (Synchronous): Live video consultation between patient and specialist.
- Benefits: ↑Accessibility, ↓costs, timely diagnosis, improved patient convenience.

⭐ Tele-ophthalmology has shown significant efficacy in screening for Diabetic Retinopathy, a leading cause of preventable blindness in India.
- Challenges: Internet connectivity, data security, initial setup cost, need for trained personnel at patient-end.
- Essential for: Reaching rural India, screening programs, follow-up care. 📌 Tele-EYES: Electronic Year-round Eye Screening
Tele-Ophthalmology Models & Tech - How It Works
Models Compared:
- 📌 Store-and-Forward (S&F): Screening Focused, asynchronous. Data sent for later review.
- 📌 Real-Time (RT): Rapid Triage, synchronous. Live consultation.
- Hybrid Models: Combine S&F and RT features for flexibility.
| Feature | Store-and-Forward (S&F) | Real-Time (RT) |
|---|---|---|
| Data Exchange | Delayed, offline review | Live, interactive consultation |
| Bandwidth | Low | High |
| Cost | Lower | Higher |
| Interaction | Indirect | Direct |
| Typical Use | Screening (DR, ROP, Glaucoma) | Urgent consults, post-op |
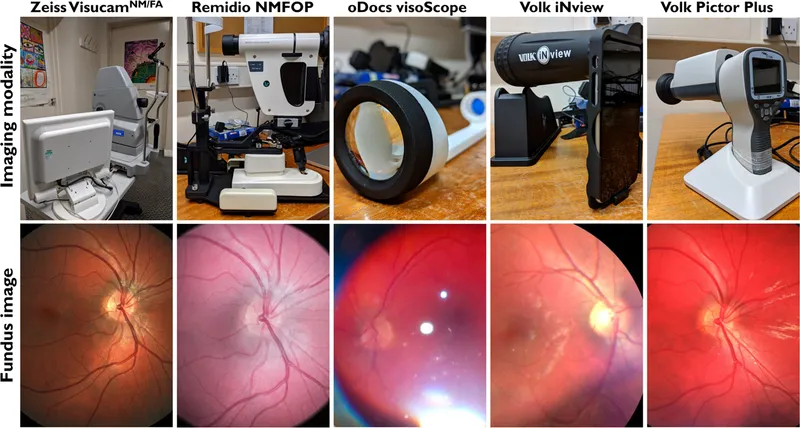
- Image Acquisition:
- Non-mydriatic fundus cameras (NMFC)
- Smartphone retinal imaging
- Portable OCT

- Software & Platforms:
- AI algorithms for automated DR detection
- Secure cloud storage & EMR integration
- DICOM for image standards
- Communication (RT):
- High-resolution video conferencing
⭐ > Store-and-forward is the most widely adopted model for diabetic retinopathy (DR) screening in India due to its cost-effectiveness and lower bandwidth needs.
Applications in Eye Care - Eye Care Anywhere
- Widespread Screening & Monitoring:
- Diabetic Retinopathy (DR): Most validated. Fundus images (by technicians) sent for remote grading. Cost-effective mass screening.
⭐ Tele-ophthalmology for DR screening significantly ↑ detection of sight-threatening retinopathy in underserved areas.
- Retinopathy of Prematurity (ROP): Critical for timely intervention (laser/anti-VEGF) in remote NICUs. (e.g., KIDROP).
- Glaucoma: IOP, optic disc photos (ONH), visual fields (VF) shared for expert opinion.
- Age-related Macular Degeneration (AMD): Monitoring progression, OCT.
- Diabetic Retinopathy (DR): Most validated. Fundus images (by technicians) sent for remote grading. Cost-effective mass screening.
- Remote Consultations & Triage:
- Routine exams (refraction, anterior segment imaging).
- Post-operative follow-up, reducing travel.
- Emergency triage (red eye, minor trauma).
- Enhanced Accessibility:
- Extends care to rural, remote, elderly, disabled.
- Supports eye care during disaster relief.
- Patient Education: Remote counselling, adherence.
Challenges & Indian Scenario - Hurdles & Horizons
- Hurdles (Challenges):
- Technical: Poor internet connectivity, low digital literacy, equipment costs, data security concerns.
- Legal/Ethical: Medico-legal liability, lack of standardized protocols, ensuring patient consent & privacy.
- Operational: Integration issues, personnel training, unclear reimbursement models.
- Indian Scenario (Horizons):
- Key Guidelines: Telemedicine Practice Guidelines (BoG-MCI/NMC, 2020).
- National Platforms: eSanjeevani; pioneering models like ARAVIND.
- NPCB&VI: Actively incorporates tele-ophthalmology for outreach.
- Future Scope: AI-driven diagnostics (e.g., diabetic retinopathy), mHealth expansion, improved rural access.
⭐ The Telemedicine Practice Guidelines 2020 (BoG-MCI/NMC) provide a framework for registered medical practitioners in India.
High‑Yield Points - ⚡ Biggest Takeaways
- Teleophthalmology delivers remote eye care services, crucial for India's vast underserved regions.
- Essential for mass screening like diabetic retinopathy, glaucoma management, and ROP in neonates.
- Utilizes store-and-forward (data sent, reviewed later) and real-time (live video) models.
- Smartphone-based fundus cameras are pivotal for affordable, accessible screening.
- Major benefits include improved healthcare access, cost reduction, and timely intervention for preventable blindness.
- Key challenges involve internet penetration, data security concerns, and standardization of care.
- National initiatives like eSanjeevani actively promote its adoption.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

